Diagnosis and treatment of neurocutaneous melanosis. Hepatic melanosis Melanosis treatment
The following varieties are distinguished:
uremic melanosis of the skin, developing in chronic renal failure;
cachectic melanosis of the skin, observed, for example, in severe forms of tuberculosis;
endocrine melanosis of the skin due to dysfunction of the pituitary gland, adrenal glands, etc.;
hepatic - for cirrhosis and other liver diseases;
toxic (arsenic), toxic reticular melanosis associated with hydrocarbon intoxication and photosensitivity.
Toxic reticular melanosis of the skin is divided into Riehl melanosis, toxic lichenoid and bullous Habermann-Hoffmann, and Siwatt reticular poikiloderma.
Toxic reticular melanosis of the skin:
In toxic reticular melanosis of the skin, the greatest etiological significance is exposure to hydrocarbons, mainly naphthenic, less often coal (motor oil, gasoline, kerosene, toluene, resins, etc.).In the pathogenesis of melanosis of the skin important role dysfunction of the endocrine glands, autonomic neuroses, malnutrition, hypovitaminosis (mainly C and group B), and increased photosensitivity play a role.
Symptoms and signs:
Toxic reticular melanosis of the skin develops gradually: at the beginning of the disease, moderate redness of exposed skin areas (face, neck, forearms) appears, sometimes accompanied by a burning sensation, heat or itching. Subsequently, hyperpigmentation of the skin of a grayish-brown (slate) color appears, first mesh, and then diffuse, spreading to closed areas of the skin (shoulders, armpits, thighs, torso).Gradually, follicular hyperkeratosis (especially pronounced on the flexor surface of the forearms), areas of skin pseudoatrophy (folding resembling tissue paper), moderate peeling, and telangiectasias appear in the affected areas.
Common signs of skin melanosis may include weakness, weakness, easy fatigue, loss of appetite, dizziness, hypotension, weight loss, etc.
Treatment and prognosis:
Treatment - general strengthening and stimulating - is carried out with vitamins C and B complex, glucocorticoids.Whitening creams are used externally. The prognosis is favorable.
Dubreuil's precancerous melanosis:
Women over 50 years of age are more often affected. At the beginning of the disease, a small, irregularly shaped brown pigment spot appears on the skin, most often of the face, as well as the chest and hands.Symptoms and signs:
The formed lesion has the appearance of a spot ranging in size from 2 to 6 cm in diameter with fuzzy, uneven contours and an unevenly colored surface, with areas of brown, gray, black, and bluish color. The skin pattern over the affected areas is usually rougher, and the elasticity of the lesion is reduced. Histologically, the stratified squamous epithelium is thickened due to acanthathic growths; large melanocytes with vacuolated nuclei, a wide zone of cytoplasm, and a large number of melanin granules are located singly or in groups in the basal layer. In the dermis there is a moderately pronounced lymphoplasmacytic infiltration.Differential diagnosis usually performed with senile keratoma.
Treatment and prognosis:
Treatment is surgical.However, when lesions are localized on the face, radiotherapy and cryodestruction are sometimes used for cosmetic purposes. The prognosis is favorable with timely treatment. In other cases, malignancy occurs, with the development of malignant melanoma in approximately 40% of cases.
Becker's melanosis:
Becker melanosis (Becker pigmented hairy hamartoma, Becker nevus) is a benign pigmented skin lesion that develops in the second or third decade of life, more often in men (5:1). Racial predisposition to the disease has not been established. In more than 80% of cases, lesions occur on the body in the form of a brown spot with irregular outlines with an area of 100-500 mm2. Pronounced growth hair is observed in 56% of patients. The disease begins in young people, which makes it easy to differentiate it from congenital nevus and coffee spots in Albright syndrome, which appear at birth. Fully developed Becker melanosis exists without changing throughout life.Treatment not developed.
Nevus spilus- this is a coffee stain, against which dark pigmented papules or spots with a diameter of 1-3 mm are identified.
Nevus appears at birth on any part of the skin. Dark pigment spots and papules represent a borderline or complex nevus.
Natural factors that stimulate epidermal pigmentation:
1) melanocyte-stimulating hormone;
2) stem cell factor;
3) fibroblast growth factor;
4) insulin-like growth factor;
5) endothelin-1;
6) leukotrienes C4 and B4.
Psoralens, or furocoumarins, are strong photosensitizing drugs that are used to stimulate skin pigmentation. The most commonly used photosensitizer in dermatology is 8-methoxypsoralen (8-MOP). The specific mechanism of skin photosensitization is unknown, but 8-MOP is preferentially taken up by epidermal cells, where it binds to cell membranes and then concentrates in the cell nucleus. After photoactivation, 8-MOP disrupts the function of membrane signaling mechanisms and binds covalently to DNA to form a psoralen-DNA complex. Altered signaling mechanisms, together with this complex, trigger a cascade of reactions to stimulate the synthesis of melanin on melanocytes and the transfer of melanin to keratinocytes. All this leads to increased skin pigmentation.
Arsenides (arsenic-containing drugs), busulfan, 5-fluorouracil, cyclophosphamide, nitrogen mustard derivative mechlorethamine (topical) and bleomycin are the most common drugs that increase skin pigmentation. The mechanisms by which this occurs are unknown; it is possible that the drugs or their metabolites directly stimulate melanocytes and increase melanin synthesis or indirectly stimulate metabolic reactions that increase epidermal melanization.
Sun rays stimulate epidermal melanocytes and enhance melanin synthesis, and also increase the transfer of melanosomes to keratinocytes. As a result, a tan develops. The appearance of tanning is caused by the action of ultraviolet rays (range 290-400 nm).
Excessive sun exposure is accompanied by hyperproduction of melanin and increased proliferation of melanocytes. Overproduction of melanin in limited areas leads to the formation of brown spots called freckles.
Skin lesions based on an increase in the number of melanocytes and increased melanin synthesis are called solar lentigines.
Chloasma:
Chloasma is hyperpigmentation of the skin in the form of yellowish-brown spots. Disorders of hormonal activity (thyroid gland, adrenal glands, pituitary gland, gonads) observed during pregnancy, as well as in menopausal women or those suffering from ovarian dysfunction are important in the pathogenesis.In some cases, the occurrence of chloasma is associated with liver diseases and increased sensitivity to sunlight. Histological examination reveals the accumulation of melanin grains in the cells of the basal and spinous layers of the epidermis and an increase in the number of melanophores in the superficial layers of the dermis.
Chloasma occurs, as a rule, in women.
Yellowish-brown spots with uneven contours appear, often on the face. In pregnant women, chloasma can also be found in the area of the mammary glands (peripapillary circles), the white line of the abdomen, around the navel, and on the external genitalia. In winter and when pathogenetic factors are eliminated, chloasma may turn pale and disappear completely. Chloasma should be distinguished from freckles, melasma and secondary skin hyperpigmentation that develop at the site of skin inflammation after prolonged exposure to mustard plasters and a number of cosmetics.
The disappearance of chloasma is facilitated by the correction of hormonal changes, long-term intake of vitamins B, C, calcium supplements, the use of exfoliating ointments (for example, 1-2% salicylic acid), 3-5% hydrogen peroxide. In the summer, protection of facial skin from exposure to UV rays is indicated.
Lentigo:
Lentigo is a limited melanin hyperchromia of the skin, characterized by the formation of small flat hyperpigmented elements. Lentigo is usually classified as pigmented nevi; in addition, lentigo occurs in some hereditary syndromes.Pathohistology:
Characterized by a significant increase in melanocytes along the dermoepidermal border and accumulation of melanin in the epidermis. In some cases, melanin is also found in the papillae of the dermis; Sometimes there is an elongation of the epidermal processes.Symptoms of lentigo at different ages:
Lentigo often appears in the first years of life in the form of single (up to a dozen) elements. A further increase in the number of rashes is observed either in adolescence (adolescent lentigo) or after 50-60 years (senile lentigo).Juvenile lentigo - multiple, scatteredly located on any area of the skin, hyperpigmented oval-round, sharply limited non-inflammatory formations of light brown or dark brown color.
Senile lentigo is localized mainly on the back of the hands, forearms, face, neck and has a dark brown color. There are no subjective sensations with lentigo. In adults, the total number of lentiginous elements varies over a wide range, often reaching 20-30. The formation of a very large number of elements is possible, up to profuse (lentiginosis) rashes, which can also be located on the mucous membranes of the oral cavity and genital organs. Rare varieties include asymmetrical or unilateral lentigine, midfacial Touraine lentigo, which is characterized by localization of elements on the forehead with a transition to the bridge of the nose, nose, less often - lips and neck, perioral lentigo - Peutz-Jeghers-Touraine syndrome.
Some elements of lentigo may over time take on a warty character or the character of pigmented hair nevi.
Diagnosis is made based on characteristic clinical picture. Differential diagnosis includes freckles and actinic keratoses.
Treatment and prognosis:
In uncomplicated cases, lentigo cannot be treated. Removal of individual elements is permissible within healthy tissues with mandatory histological examination. In case of malignancy, surgical intervention followed by radiotherapy is indicated.The prognosis is favorable. Malignancy occurs extremely rarely.
Moynahan syndrome:
This benign disease of young people is characterized by the rapid appearance of hundreds of lentiginous spots (especially Moynahan syndrome or Peutz-Jeghers syndrome) and is autosomal dominant.Patients with Moynahan syndrome have hundreds of lentigines on the face, trunk, and extremities. The clinical manifestations of the syndrome are easy to remember using the word LEOPARD:
1) L - lentigo (Lentigines);
2) E - electrocardiographic changes (ECY-defects);
3) O - ocular hypertelorism;
4) P - pulmonary artery stenosis (Pulmonic stenosis);
5) A - pathology of the genitals (Abnormal genitalia);
6) R - growth retardation;
7) D - deafness.
Freckles:
Freckles are pigment spots that do not rise above the skin level, do not peel, and do not cause subjective sensations. Spots of brown or yellowish color, small, round or irregular in shape, localized symmetrically on the face, back of the forearms, hands, less often on the back, shoulders and lower limbs. Freckles appear in childhood or adolescence (nevoid nature is possible), more often in fair-haired people. Under the influence of ultraviolet rays and ionizing radiation, the intensity of pigmentation increases.Histology: accumulations of melanin in the germinal layer of the epidermis with a normal number of melanocytes in the dermis.
Treatment provides only a temporary effect. Creams with a whitening effect are used. In spring and summer, photoprotective creams are applied to the skin.
Poikiloderma:
Poikiloderma is a complex of dystrophic skin changes characterized by reticular hyperpigmentation alternating with scattered areas of skin atrophy and telangiectasia. Poikiloderma can be congenital and acquired, symptomatic and independent.Symptoms of poikiloderma:
Symptomatic poikiloderma can be a manifestation of radiation dermatitis, parapsoriasis, dermatomyositis, scleroderma.With poikiloderma, thinning of the epidermis, accumulation of melanin in the basal layer of the skin, smoothing of the papillae of the dermis with expansion of the lumens of blood vessels are observed, around which a stripe-like infiltrate of lymphocytes, histocytes and melanophores lies.
Congenital poikiloderma (Thomson syndrome) appears in early childhood, sometimes from birth. Initially, the rashes are diffuse or patchy erythema, then telangiectasia, reticulated brown hyperpigmentation, and areas of mild atrophy of the skin of the face, neck, buttocks, and limbs appear. Characterized by dystrophy of hair and teeth.
In limited areas of the skin, poikiloderma is observed in the rare Bloom's syndrome (congenital telangiectatic erythema with dwarfism). Skin lesions develop in the first year of life after sun exposure in the form of erythematous lesions on the face and ears, against which telangiectasia and hyperpigmentation appear.
Treatment:
Treatment is carried out with vitamins A, C, E, P, PP, corticosteroid and anabolic hormones, and for Bloom's syndrome - photoprotective agents.Peutz-Jeghers syndrome:
With Peutz-Jeghers syndrome, widespread lentiginous lesions of the skin of the lips, buccal mucosa, palate, tongue and eyelids are noted, as well as gastrointestinal polyps (mainly of the small intestine), manifesting in the second decade of life with diarrhea, hemorrhages, obstruction or intussusception. Malignant degeneration of polyps with the development of carcinomas in the intestines and stomach has also been described.Neurofibromatosis:
Neurofibromatosis-1 (NF-1, Recklinghausen disease) is characterized by coffee spots (cafe au lait) and freckle-like elements in the axillary and groin areas. Brownish spots with a diameter of several millimeters to several centimeters are localized on any part of the skin. More than 20% of spots are present from birth or appear in the first year of life. NF-1 is a relatively common autosomal dominant disorder (1:3000).In 1937, Albright described a syndrome characterized by disseminated osteitis fibrosa, endocrine dysfunction (premature puberty in girls), and coffee spots. The latter differ from those with NF-1 by their predominant localization in the forehead, back of the neck, sacrum and buttocks. In addition, in Albright syndrome, spots appear at or shortly after birth and are located unilaterally, without crossing the midline of the body.
Addison's disease:
Addison's disease is characterized by diffuse hypermelanosis predominantly in the mucous membranes, skin folds, palmar grooves and areas of greatest pressure (elbows, knees, knuckles and tailbone). Adrenocorticotropic hormone (ACTH) or tumors that produce melanocyte-stimulating hormone can increase skin pigmentation; a similar effect is observed when these hormones are administered systemically. Pregnancy and estrogen therapy lead to hyperpigmentation of the nipples and anogenital area. In addition, oily hyperpigmentation (melasma) may develop on the forehead, temples, cheeks, nose, upper lip in pregnant women and against the background of estrogen use.Treatment consists of hormone replacement therapy with prednisolone and hydrocortisone. The dose is selected individually in a hospital setting.
Blue-gray dispigmentation:
Blue-gray dispigmentation develops when melanin is present in dermal melanocytes, melanin deposits in the dermis, or non-melanin discolorations in the dermis.Nevus of Ota (oculodermal melanocytosis):
Nevus of Ota (oculodermal melanocytosis) is an acquired disorder of dermal melanocytosis that develops in early childhood or young adulthood. It occurs in less than 1% of people of Asian descent, and is even less common among other races. In women, dermatosis is observed 5 times more often than in men. Nevus colors range from dark brown to violet-brown and blue-black. Most often, the periorbital region of one eye is involved in the process, although bilateral lesions can also occur, as well as the spread of the process to the temporal region, forehead, periorbital areas of the cheeks, nose and eye structures.Nevus Ito:
Nevus of Ito is a variant of nevus of Ota, differing from it only in localization (the neck and shoulder areas are affected).Fixed drug rashes are localized variants of drug reactions in the form of reddish-brown to gray-blue spots. They appear in the same place after each dose of the drug that caused the dermatosis. Initially, the skin changes are erythematous, swollen and scaly, sometimes forming a blister. The inflammation resolves, leaving hyperpigmentation with clear edges. The process can involve any area of the skin, including the face, fingers, oral mucosa and genitals.
The most common causes of fixed rashes are tetracyclines, barbiturates, salicylates, and phenolphthalein. Cure occurs after discontinuation of the corresponding drug.
Erythema:
Erythema (ab igne) is a skin reaction to heat. Constant use of heating blankets (mats) is the most common cause of the disease. The affected areas of the skin are characterized by network-like gray-blue dispigmentation, sometimes erythema and peeling are noted. Patients complain of a burning sensation and itching. The basis of treatment is to stop using heating agents for a period of several months to a year. Scars and hyperpigmentation sometimes remain in damaged areas.Ochronosis (alkaptonuria):
Ochronosis (alkaptonuria) is a rare autosomal recessive inherited deficiency of homogentisic acid oxidase, leading to the accumulation of this acid in connective tissue. As a result, skin color changes from dark brown to bluish-gray develop.Most often the process involves the auricles, tip of the nose, sclera, dorsum of the hands, nail plates of the fingers and tympanic membranes; less often - the central part of the face, axillary areas, genitals.
Homogentisic acid is also deposited in bones and articular cartilage, causing ochronic arthropathy, which later transforms into premature degenerative arthritis. The course of ochronosis is accompanied by progressive dyspigmentation and degeneration of joints. The treatment has no effect.
Deposits of silver, mercury, bismuth, arsenic and gold in the dermis can cause changes in skin color from brown to grayish-blue. The toxic effect of silver, mercury and bismuth causes the gray-blue color of the skin, nails and mucous membranes. Lesions due to the action of silver (argyria) are most pronounced in areas of the skin exposed to sunlight. Chrysoderma- rare brown pigmentation of the skin, which develops as a result of parenteral administration of gold preparations, is also most pronounced on open areas of the skin.
Amiodarone, bleomycin, busulfan, chloroquine, chlorpromazine, clofazimine, minocycline, trifluoroperazine, thioridazine and zidovudine cause blue-gray pigmentation of the skin and mucous membranes.
Sturge-Weber syndrome:
Bilateral port-wine stain involving the innervation zones of the ophthalmic and maxillary branches of the trigeminal nerve. The syndrome is not inherited. It is a sporadically occurring disorder of the development of the leptomeningeal vessels, facial capillaries, and (often) ocular vessels.In leptomeningeal angiomatosis, the formation of meningeal vessels is complicated by calcification of the meningeal artery, the underlying cerebral cortex, and cerebral atrophy.
This leads to epilepsy in 75-90% of cases, mental retardation (especially in people with severe epilepsy) and sometimes to contralateral hemiplegia.
In Sturge-Weber syndrome, the vascular nevus is most often localized in the area of innervation of the ophthalmic (VI) and maxillary (V2) branches of the trigeminal nerve. The forehead, upper eyelids, and base of the nose are partially involved. The vascular spot can be bilateral and affect the nose and oral mucosa, and in 40% of cases - the trunk and limbs.
Epilepsy in Sturge-Weber syndrome usually begins between the second and seventh months of life, but in rare cases it occurs in late childhood. At first the seizures are minor, but they progress with age. There is no correlation between the prevalence of vascular nevus, leptomeningeal angiomatosis and the severity of neurological disorders.
Diagnosis Leptomeningeal angiomatosis can be confirmed by computed tomography with contrast agent or MRI.
In late childhood ( average age 7 years) X-ray examination of the flat bones of the skull can reveal typical double-circuit tortuous calcifications. Eye lesions occur in 30-60% of cases and are represented by damage to the capillaries, conjunctiva, iris, glaucoma, and an increase in the size of the cornea. These complications can only be associated with a nevus in the area of the ophthalmic branch n. trigeminus and do not necessarily indicate involvement of the central nervous system in the pathological process. Glaucoma most often begins in the first 2 years of life, therefore, regular ophthalmological examination of children with facial vascular nevus is necessary.
Most effective method treatment of vascular nevus of the face - the use of a tunable pulsating laser (wavelength 577/585 nm). Regular laser therapy leads to a significant reduction in the manifestations of the disease and prevents soft tissue hypertrophy, which can gradually develop with such nevi.
Hippel-Lindau disease:
Bilateral retinal angiomatosis (50%), cerebral or spinal hemangioblastoma (40%), renal carcinoma (25%) and rarely pheochromocytoma also occur in Hippel-Lindau disease.In some cases, hyperpigmentation (melasma) may be caused by intoxication (arsenic, etc.), long-term use of certain medications (sulfonamide drugs, etc.). Anthracosis of the skin is caused by the introduction of particles coal, tattoo (tattoo) - introducing dyes into the skin by pricking. Skin argyria develops in persons in contact with metallic silver and lapis; in this case, silver enters the body through the skin, gastrointestinal tract or Airways, as a result of which the skin, especially the face, hands and folds, acquires a gray color with a bluish tint.
There is a group of hereditary diseases that are characterized by massive damage to the skin, nervous system and other important organs. What is neurocutaneous melanosis? In this brief review, we have collected complete information about this rare disease, so we will tell you about the main symptoms of the disease and how to get rid of it.
Neurocutaneous melanosis is a fairly rare disease.
reference Information
The disease was first recorded in the second half of the 19th century by the German scientist Rudolf Virchow. After 120 years, the name neurocutaneous melanosis was officially recognized. The origin and culprits of the disease have not been precisely established. Doctors believe that the occurrence of abnormalities is an early somatic mutation. As a result of chromosome breakage, the movement of melanocytes is disrupted, which leads to their accumulation on the skin and central nervous system.
The disease is rare and often inherited. Children are born without any abnormalities in weight or skin color. The only indicator of the presence of the disease is a nevus - a small mole or tumor that has a different color (from dark brown to deep black) and shape. The rough surface of the spot is covered with fine hairs. The formation rises slightly above the level of the dermis.
The surface is rough and bumpy, covered with crusts. Nevi have irregular outlines.
Most often the disease is recorded:
- lumbosacral region;
- on the neck and back of the head;
- on the back.
The disease is complex and does not have any sexual preferences. Destructive actions affect:
- vessels (blood, lymphatic);
- sebaceous and sweat glands;
- hair follicles;
- subcutaneous tissue;
- muscles;
- skeleton.
Initially, the child develops without any deviations. But from the second year of life, characteristic signs begin to appear.
- Mental retardation. The inability to quickly and effectively learn and remember becomes noticeable.
- Cramps. Epileptic seizures occur due to the penetration of melanoblastomas into the brain.
- The appearance of nevus on other parts of the body. The spots invade new areas, growing and changing shape.
- Mutation. The tumor is activated, as a result of which doctors note a modification of color and structure. An unpleasant itching occurs.
- Neurological transformation. The meninges thicken and melanomas and benign neoplasms appear in the organ tissue, and cysts often appear. Externally, this manifests itself in the form of increased intracranial pressure from the first year of life.
Children with the disease suffer from birth defects heart or bone changes. Sometimes pigment is deposited at the bottom of the eye, which causes cataracts. In combination with tumors of various natures, nevi gradually degenerate into oncology. This serious and terrible disease occurs in more than 50% of patients with melanosis.

Sometimes pigment is deposited at the bottom of the eye
Treatment
To draw up a treatment plan, the specialist collects information about the medical history and conducts a series of tests. A biopsy of the affected area of the dermis will help assess the condition of the muscles and skin. For a complete clinical picture, ultrasound data must be considered. Parents are worried that they have to take a lot of tests. Such checks are aimed at getting an idea of the extent to which the body is affected by the disease. Scintigraphy, MRI, CT are mandatory procedures.
There is still no effective cure or method for neurocutaneous melanosis. For more than 150 years, scientists around the world have been trying to find a safe solution to get rid of a dangerous disease. Therapy follows a specific regimen prescribed by the doctor. They use drugs that block the growth and reproduction of pathogenic cells. Drugs that affect protein and carbohydrate metabolism have an antishock and antitoxic effect, so they are taken in increased doses.
To reduce seizures, the doctor prescribes anticonvulsants. Additionally, it is necessary to support the immune system, which recombinant cytostatics must cope with.
If the disease was diagnosed in the first years of life, then the specialist decides on surgical intervention. Early tumor removal will reduce the negative impact of the disease on the child's development.
If a nevus is detected on the baby’s body, then it is better to immediately visit a doctor. A professional will carefully monitor all transformations in the body and begin treatment at the first changes. To prevent a hairy mole from mutating into melanoma, they may suggest excision of the skin followed by transplantation of healthy samples.
The progression of neurocutaneous melanosis intensifies pathological processes. Activation of the disease and the capture of a larger area of the dermis cannot be stopped by radiation therapy. Patients rarely live beyond the age of twenty-five. Remember: the more attentive you are to your baby, the greater the chance of finding the disease before destructive activity begins.
If similar problems have been recorded in the family, then the child is at risk.
Neurocutaneous melanosis is a dangerous hereditary disease that is very difficult to cure if neglected. Our recommendations will help you determine the symptoms, and entrust the therapy to a professional oncologist.
Constant scratching and rubbing leads to hyperpigmentation secondary to the increased amount of melanin in the skin, and the combination of melanin and bile pigments gives the skin a bronze color.
Melanosis uremic
In patients with chronic renal failure, hyperpigmentation of the skin may occur: in 30% of cases it is localized only on the palms and soles, in 22% of cases it is diffuse or located on open areas of the body.
The cause of hyperpigmentation is an increase in the amount of melanin in the basal layer of the epidermis and the superficial layers of the dermis. It is assumed that in such patients the metabolism of 6-melanocyte-stimulating hormone is reduced due to kidney disease, which leads to an increase in the level of this hormone in plasma.
This hormone, in turn, stimulates the production of melanin by melanocytes. Initially, with kidney disease (chronic interstitial nephritis), a diffuse brown coloration of the skin occurs. Subsequently, depending on the severity of renal anemia and with the progression of chronic renal failure, the skin pigmentation gradually acquires an ash-gray tint.
Melanosis cachectic
Currently, the dependence of increased skin pigmentation on severe chronic diseases accompanied by general cachexia, anemia and marasmus (tuberculosis, malignant tumors, peritonitis and others) is unclear.
In this case, changes in the skin can be further aggravated by hyperkeratosis and hypertrophy of the papillae, resulting in the picture of acanthosis nigricans: the skin thickens, darkens, and becomes similar to shagreen. Hyperpigmentation has a dirty brown color and is localized on the neck, abdomen and genitals.
It is believed that this melasma is an abortive form of Addison's disease, which is why it is called "Addisonism." However, with this melanosis, darkening of the skin of the face and limbs is not observed, and there is no damage to the mucous membranes. It is possible that these changes are based on some “toxic” influences or increased protein breakdown, which is known to be important for the formation of melanin.

Melanosis of the skin is an excessive deposition of the melanin pigment in the epidermis. This substance is produced by special cells (melanocytes) and is designed to protect skin cells from the sun's rays. Light-skinned people produce this pigment in smaller quantities than dark-skinned people. Normally, melanin is activated only under the influence of ultraviolet light. In this case, a tan appears on the skin. If this pigment is deposited in large quantities, a disease occurs - melanosis. It is accompanied by a change in skin color.
Causes of the disease
Melanosis of the skin can be caused by various reasons. Changes in the color of the epidermis can be caused by the following factors:
- pathologies of the endocrine glands (pituitary gland, adrenal glands, ovaries, thyroid gland);
- infectious diseases(syphilis, dysentery, tuberculosis, malaria);
- carbon compounds and toxic resins;
- advanced forms of pediculosis;
- liver diseases;
- blood diseases (porphyria);
- pathology of connective tissue (collagenosis);
- taking medications (sulfonamides, tetracycline antibiotics, photosensitizing drugs).
In addition to pathological reasons, changes in skin color can occur due to poor nutrition and metabolic disorders in the epidermis. There is also a hereditary form of melanosis, in which the disease is transmitted from parents to children.
Localized and generalized forms
There are localized and generalized types of melanosis of the skin. What does this mean? In the first case, pigmented areas appear on the epidermis. With generalized melanosis, the color of the entire skin changes.
Most often, generalized melanosis of the skin is observed with Addison's disease, pituitary pathologies, diabetes, collagenosis, arsenic poisoning, as well as with an excess of porphyrins in the blood. In this case, the entire human skin becomes bronze in color.
Localized melanosis is a symptom of the following diseases:
- Poikiloderma Siwatt. This pathology occurs in women of childbearing age. The disease is associated with a functional malfunction of the ovaries or adrenal glands.
- Riehl's melanosis. The cause of this disease is not exactly clear. It is believed to be caused by contact with hydrocarbons.
- Toxic melasma of Hoffmann-Habermann. This disease occurs only in men. It is caused by poisoning with hydrocarbon substances. This disease usually affects people who sweat excessively.
With the above diseases, pigmented spots are noted on the patient’s face and neck. At the same time, other areas of the skin do not change their color.
Types of pathology by origin
There is also a classification of pathology depending on its origin. The following types of skin melanosis are distinguished:
- Uremic. It is observed in case of insufficiency of kidney function.
- Endocrine. Occurs with diseases of the adrenal glands, pituitary gland, ovaries or thyroid gland.
- Toxic. It is caused by arsenic and hydrocarbon poisoning.
- Hepatic. This form of melanosis is associated with cirrhosis, hepatitis and other liver diseases.
- Cachectic. It is observed with severe exhaustion, most often with pulmonary tuberculosis.

These forms of pathology are secondary. Melanosis in these cases is only one of the symptoms of other diseases. However, there are also primary forms of cutaneous melanosis. Some of them are dangerous because they are prone to malignant degeneration. These types of pathologies include the following diseases:
- Chloasma. These are large brown spots on the epidermis. They usually appear on the face. The reasons for their appearance have not been established. Supposed. that they are formed due to hormonal disorders.
- Lentigo. These are small yellow or benign formations. However, with injury or excessive exposure to the sun, malignant degeneration of cells is possible.
- Becker's melanosis. This disease mainly affects young men. A mole appears on the skin, which is then covered with thick hair. This formation is not dangerous, as it does not degenerate into cancer.
- This formation occurs in people over 50 years of age. It appears as a raised brown spot, similar to a mole. This disease is a precancerous condition and requires immediate treatment. The neoplasm consists of atypical melanocytes, which easily degenerate into malignant cells.
Symptoms
Symptoms of pathology depend on its form and cause. If the patient's entire skin turns bronze or yellowish, this indicates a generalized form of cutaneous melanosis. Photos of the manifestations of the disease can be seen below.

If melanosis occurs in a localized form, then the rash is observed only on the face and neck. In toxic melasma, these areas of the body are uniformly colored grayish-yellow. Rashes in the form of age spots, moles and freckles are most often of a primary nature.
Complications
If melanosis is secondary, then one should not be afraid of malignant degeneration of the rash. In this case, only the underlying disease poses a health hazard. If melanosis is primary in nature, and a mole or spot appears on the skin, then you should immediately consult a doctor. Some of these formations are prone to malignant degeneration and can develop into skin cancer - melanoma. Malignancy (malignancy) of a mole is indicated by its accelerated growth, changes in shape and color, the appearance of ulcers and bleeding. Malignancy can be triggered by exposure to ultraviolet rays and trauma to the formation. It should be remembered that moles covered with hair are not dangerous.
Diagnostics
Melanosis is treated by a dermatologist. However, if the change in skin color is caused by other diseases, then consultation with an endocrinologist, therapist, infectious disease specialist and other specialists is necessary.
The following examinations are prescribed:
- The patient's skin is examined using a special black light lamp (Wood's lamp).
- A biopsy of the affected skin is performed. Particles of the epidermis are taken for histological examination.
- They do a dermoscopy. This is an absolutely painless examination that does not require excision of the affected areas. New growths on the epidermis are examined under a special device - a dermatoscope.

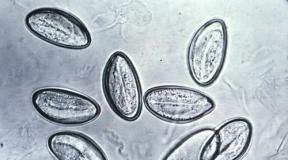
Dermoscopy allows you to examine the mole in detail. If there is doubt about the benign quality of the formation, then a biopsy is prescribed. Histological examination allows one to distinguish a melanoma tumor from cutaneous melanosis. A microscopic specimen of the epidermis can be seen in the photo above; black-brown granules are accumulations of melanin.
Treatment
If melanosis is secondary, then it is necessary to treat the underlying disease. In this case, the skin color returns to normal after the end of the course of therapy. For primary melanosis of the skin, treatment is carried out using both conservative and surgical methods. The following drugs are prescribed:
- vitamins A, E, ascorbic and nicotinic acid;
- corticosteroid hormones;
- antihistamines.
External preparations are also used:
- hydrogen peroxide;
- creams and ointments with vitamin A;
- citric acid solution.

Nowadays, there are cosmetic procedures that help whiten the skin and eliminate blemishes. However, before using such methods, it is necessary to undergo diagnostics and make sure that the tumor is benign. The following procedures will help get rid of spots on the skin:
- Chemical peeling. A special composition is applied to the face, which helps exfoliate the upper layer of the epidermis.
- Phototherapy. The skin is exposed to pulsed light. This causes a change in the structure of melanin. As a result, the epidermis whitens.
- Laser resurfacing. Under the influence of a laser beam, the problem area of the skin evaporates.

In some cases, surgical treatment is indicated. This is necessary when the mole is prone to malignancy. The nevus is removed under local anesthesia, and the resulting material is sent for histological examination. If the operation cannot be performed, then irradiation of the mole is used.
Prevention
Prevention of secondary forms of melanosis involves timely treatment of diseases that lead to changes in skin color. Great care should also be taken when working with arsenic and hydrocarbon compounds. Prevention of primary forms of melanosis has not been developed, since the causes of their occurrence are not known. If moles and spots appear on the skin, you should consult a dermatologist as soon as possible. Such rashes can be dangerous. In these cases, it is necessary to avoid exposure to sunlight and trauma to moles and spots.
Skin inflammation is a condition in which the body accumulates excess amounts of a pigment called melanin.
Melanosis can be physiological (for example, in some races due to excess sunlight, or during pregnancy), or pathological, when accumulation occurs in those places and organs where it should be normal.
Pathological accumulation usually occurs on organs, in the membrane of the brain, on mucous membranes, and in the substance of the brain.
The formation of melanin is regulated by the sympathetic nervous system and endocrine glands. Therefore, the most common cause is dysfunction of these systems.
Reasons for development
The reasons for the development of the accumulation process are not fully understood. Among the most likely are:
- heredity;
- irregularities in work endocrine system(insufficiency of the adrenal cortex, improper production of the hormone by the pituitary gland, pathology of the gonads);
- vitamin deficiency (pellagra, scurvy, etc.).
Kinds
Scientists identify several types of the disease. Pathological melanosis can be:
- congenital:
- reticular progressive;
- Excessive melanoblastosis.
- purchased:
- diffuse;
- focal.
The reticular progressive type is very rare. It is associated with increased skin sensitivity to sunlight. It manifests itself in the form of patchy pigmentation, as well as the formation of melanophores in the skin, hyperkeratosis and swelling of the skin.
The excessive type is usually diagnosed in babies under 1 month of age. It is tumor in nature and is associated with metastases of maternal melanoma that cross the placenta. Such a newborn will have dark areas on the skin, and melanin is found in the nucleus of nerve cells and in the brain. Histological analysis reveals clusters of nevus- and melanophore-like cells, which contain a lot of pigment.
Acquired types of the disease are much more common.
The diffuse type affects the skin and is associated with disruption of the endocrine system. Often diagnosed with Addison's disease. Focal affects internal organs, especially the intestines. It most often affects people with intestinal obstruction, as well as chronic constipation. Localization occurs in the ileocecal region, sigmoid and rectum. The mucous membrane becomes brown or black.
Treatment
Treatment is carried out with hormone therapy and large amounts of vitamin C.
 For external use, creams are prescribed that contain kojic and azelaic acid, as well as hydroquinone and tretinoin.
For external use, creams are prescribed that contain kojic and azelaic acid, as well as hydroquinone and tretinoin.
Laser stain removal is prescribed in particularly severe cases. If the formation of melanotic spots on the skin is caused by hormonal drugs, their use should be stopped. In pregnant women, the spots disappear on their own after childbirth and normalization of the hormonal system.
There are also a number of folk remedies that can help remove melanosis spots from the skin.
You can prepare masks at home from:
- banana (apply the crushed fruit to the stains and leave for 15 minutes);
- eggplant (use the pulp wrapped in gauze - leave on the stain for 15 minutes);
- oxygenated water (washing will have a positive effect on skin color);
- honey, milk powder and lemon juice (mix until smooth and apply to face for 20 minutes. Then rinse and anoint face with yogurt);
Melanosis is hereditary, so if there have been cases of the disease in the family, a person needs to take more care of himself, use good sunscreen, and not take medications that can cause such a reaction.