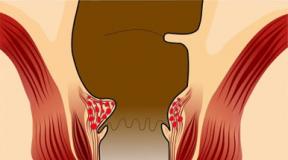
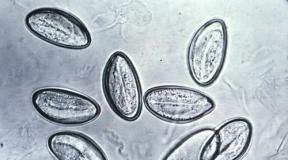
What is Mycoplasma hominis and how is it transmitted? Symptoms of mycoplasmosis in men Signs of damage to the genitourinary system
When infected with Mycoplasma hominis, symptoms do not always appear. This microorganism can live in the urogenital tract for a long time without causing inflammatory reactions.
But at certain moments the population of bacteria increases. As a result, they cause urethritis, cystitis, and inflammation of the internal genital organs in men and women.
Exacerbation of mycoplasmosis occurs against the background of immunodeficiency and antibiotic therapy. This can happen during pregnancy or in case of other sexually transmitted infections.

- First symptoms
- Symptoms of urethritis
- Symptoms of cystitis
- Symptoms in children
- Symptoms of complications
- Symptoms of joint damage
- Symptoms of infertility
- Symptoms of HIV
Incubation period of mycoplasma hominis
Mycoplasmas are transmitted through sexual contact. Household transmission has not been proven.
Children can become infected from their mothers in utero or during childbirth.
The most common route of infection is sexual. After this, symptoms of Mycoplasma hominis do not appear immediately. At least 2-3 weeks must pass before inflammatory processes in the urogenital tract occur.
Sometimes it takes much longer for symptoms to appear. Because Mycoplasma hominis is considered an opportunistic bacterium.
Certain conditions are required for pathogenicity to occur. Mycoplasma hominis is often found in the urogenital tract of clinically healthy individuals.
First symptoms
Initial signs usually occur from the urethra. Mycoplasmas colonize the urethra.
The first symptom may be dysuria. This is a complex of symptoms indicating urinary disorders.
It could be:
- faster
- painful
- difficult
Frequent urination is observed due to irritation of the urethral receptors.
And when spreading to mycoplasma, hominis to the neck Bladder strong, uncontrollable urges are possible. The patient walks frequently, but the volume of urine excreted is insignificant.
Pain may be felt as urine passes through the urethra.  This is due to irritation of the damaged mucous membrane of the urethra.
This is due to irritation of the damaged mucous membrane of the urethra.
In men, there are cases when, after infection with Mycoplasma hominis, urination becomes difficult. This is due to swelling of the urethra.
In men it is thinner than in women. Therefore, in case of swelling, a sluggish stream of urine is possible.
Mycoplasmas can also infect the prostate. Especially if there are already foci of chronic inflammation.
The result of its swelling can also be difficulty urinating. Occasionally, traces of blood are found in the urine.
Mycoplasma hominis is characterized by discharge from the genitals. They are usually not intense. They often go unnoticed by the patient. Because the discharge is mucous and not purulent.
Women may confuse them with various physiological vaginal discharges. However, they differ in that they have an unpleasant odor.
Appear against the background of an inflammatory process. Combined with other signs of urethritis.
Symptoms of urethritis
The urethra becomes the entry point for infection when infected in men and women. Although in female patients the vaginal mucosa may also become inflamed.
With urethritis, those infected with mycoplasma suffer from the following symptoms:
- pain when urinating
- discharge from the urethra
- redness in the area of the outlet
- pain during sexual intercourse, as a result – refusal of intimate life
At night, discharge accumulates. They can cause the walls of the urethra to stick together. The first urination after a night's sleep may be difficult.
Symptoms of cystitis
Sometimes mycoplasma hominis leads to the development of cystitis. 
More often, symptoms of this disease occur in women. Their urethra is much shorter than the male's. Therefore, mycoplasma hominis ascends into the bladder. It causes cystitis.
The symptoms of this disease are as follows:
- pain in the lower abdomen
- the presence of mucus or pus in the urine (threads are detected upon examination)
- frequent urination
- feeling of residual urine in the bladder
There may be a false urge to urinate. They can occur immediately after the next trip to the toilet.
With mycoplasma cystitis, it usually has a mild clinical course. There is no large amount of pus released. There are no signs of intoxication.
Patients do not have an increase in body temperature, no weakness or headache. There is no reflex urinary retention as a result of detrusor spasm. In this way, the symptoms of cystitis due to infection with Mycoplasma hominis differ from nonspecific bacterial inflammation.
Symptoms of colpitis with mycoplasma hominis in women
In women, Mycoplasma hominis can cause inflammation of the vagina. This pathological process is called colpitis. With mycoplasmosis, it can occur in both acute and chronic forms.
A woman complains of itching in the vagina. The external genitalia may also become inflamed at the same time. Discharge appears.
Upon examination, redness of the vaginal mucosa is detected. Small pinpoint hemorrhages are possible.
Sexual intercourse becomes painful. Therefore, women often refuse intimacy. If pain is not felt during sexual intercourse, then it occurs after its completion. 
Clinical signs may improve even without treatment. But mycoplasma hominis remains in the body. It can cause re-inflammation of the bladder at any time.
Symptoms of testicular damage in men
Mycoplasma hominis sometimes affects the testicles of men. Typically, such orchiepididymitis occurs subacutely or chronically. They are accompanied by nagging pain in the scrotum.
Painful sensations are often permanent, although they may intensify after:
- physical activity
- sexual intercourse
- mechanical pressure on the scrotum, even slight
Upon palpation, an edematous appendage and testicle are determined.
Swelling is often detected. There may be redness of the skin of the scrotum. Its folds are smoothed out.
Blood may be present in the ejaculate.
Symptoms in children
Children can become infected with mycoplasmosis through sexual intercourse if they begin to be intimate before the age of 18. In this case, their symptoms are the same as in adult patients. But the difference is that the clinical signs are usually more pronounced.
In children, Mycoplasma hominis rarely causes any symptoms. Much more often, urethritis, cystitis or colpitis occurs in an acute form.
Newborns also suffer from mycoplasmosis. They become infected through the placenta in utero. Transmission of infection during childbirth is also possible.
In children, mycoplasma hominis can affect various organs. The eyes, kidneys, and lungs can become inflamed. Therefore, mycoplasmosis is very dangerous for a pregnant woman.
Symptoms of complications
The insidiousness of mycoplasmosis is that it is often mild. The disease is either not accompanied by symptoms at all or has minimal clinical manifestations.
The patient does not see a doctor for a long time. The pathology can last for years. As a result, complications arise. Sometimes they are quite heavy.
Mycoplasmas can cause infertility in both sexes. They can provoke Reiter's disease. These are reactive inflammatory processes that mainly affect the joints. But they can also affect other organs.
Symptoms of joint damage
Reactive arthritis is an inflammatory process that affects the joints when the inflammatory focus is localized in another part of the body. It sometimes develops against the background of long-term mycoplasmosis. The risk of pathology increases significantly when a chronic focus of inflammation is localized in the prostate gland of men.
Most often, only one joint becomes inflamed. As a rule, this is a large joint lower limb. Less commonly, the joints of the hands become inflamed: elbow, shoulder.
The duration of reactive arthritis caused by Mycoplasma hominis is on average six months. Moreover, inflammation continues, even if mycoplasmosis has already been cured. After all, it is not caused by the bacteria themselves.
This “raging” immunity provokes joint damage. After the inflammation subsides, it may recur again after some time. This happens in 50% of cases. In 20% of patients, the plantar fascia or Achilles tendon becomes inflamed.
The pathology is manifested by pain when walking.
With mycoplasmosis, reactive inflammatory processes can affect the skin.
Sometimes keratoderma occurs and ulcers appear in the mouth.
In rare cases, inflammation of the kidneys, structures of cardio-vascular system or brain.
Symptoms of infertility
Mycoplasma hominis can cause infertility in both men and women. This becomes possible when the inflammatory process is localized in the internal genital organs.
In women, mycoplasma can cause inflammation of the uterus.
When the functional and basal layer of the endometrium is involved in the pathological process, endometritis occurs.
It can be chronic. In this case, the process of growing the endometrium is disrupted. It becomes thin and does not acquire the necessary three-layer structure a few days after ovulation. Accordingly, the endometrium cannot accept the embryo.
Even if the egg is fertilized and reaches the uterus, it simply dies, since it cannot be implanted into the mucous membrane of the uterus. Very often, mycoplasma hominis, if it is detected in the endometrium, is part of a mixed flora. There are cases where this bacterium caused inflammation fallopian tubes.
With a prolonged course of salpingitis, their patency may be impaired. This is fraught with tubal infertility. It develops only when both tubes are affected. If only one of them becomes impassable, pregnancy is possible, but its likelihood is reduced.
Damage to the fallopian tubes by Mycoplasma hominis is also dangerous because it increases the risk of ectopic pregnancy. If the fertilized egg is attached to the tube, it may subsequently be removed. Moreover, this is far from the worst outcome of a tubal pregnancy.
If it remains undiagnosed, it threatens the woman’s life. After all, the pipe can burst at any moment.
Infertility occurs with mycoplasmosis in men.
When the prostate is damaged, secretion production is disrupted. And it is necessary to maintain the vital activity of male reproductive cells. The quality of sperm deteriorates and pregnancy becomes impossible.
When the testicles become inflamed, spermatogenesis is disrupted.
This is the process of sperm formation. For men it should go continuously. When it is disturbed, the number of sperm in the ejaculate decreases, and the percentage of morphologically irregular forms of germ cells increases.
Sometimes Mycoplasma hominis causes bilateral inflammation of the vas deferens. In this case, obstructive male infertility develops.
Sperm are produced by the testes. But they cannot enter the urethra and, accordingly, the woman’s vagina. Because the “tubes” through which germ cells move are blocked as a result of a long-term inflammatory process.
Mycoplasma hominis without symptoms
Very often, mycoplasma hominis occurs without symptoms.
Therefore, the diagnosis of mycoplasmosis is established only when:
- there is an inflammatory process
- no pathogens other than mycoplasma that could provoke it have been identified
The mere fact of identifying mycoplasmas is not considered an indication for treatment. Many venereologists believe that since there are no symptoms, there is nothing to worry about.
In fact, mycoplasma hominis is dangerous, even if there is no inflammation of the urogenital tract, and here’s why:
- the disease can become active at any time
- any additional infection will be much more severe
- mycoplasma can spread to the internal genital organs
- a carrier of mycoplasma hominis will infect other people
- with mycoplasmosis in women, it often worsens during pregnancy and threatens its normal course
For these reasons, if Mycoplasma hominis is detected, it is better to be treated immediately. You should not wait for symptoms or spontaneous abortion to begin treatment.
When symptoms disappear with treatment
If there are symptoms of mycoplasmosis, then with treatment they disappear quite quickly. The course of therapy itself lasts from 10 to 14 days. But after 3-5 days of antibiotic therapy, a person’s discharge may stop.
His dysuric symptoms and signs of inflammation in the urethra disappear. This does not mean that you need to stop treatment. The course of antibiotics should be completed to the end.
Any infectious disease, including mycoplasmosis, is treated for as many days as the symptoms last, plus another 3-4 days.
Symptoms of HIV
Very often, mycoplasmas are combined with other STDs. Mycoplasmosis can also occur against the background of HIV. If the immunodeficiency virus has not yet caused pronounced immune disorders, then the disease will proceed as usual.
Mycoplasma hominis may not cause symptoms for a long time. Or has minimal clinical manifestations.
But with severe immunodeficiency, the disease progresses rapidly. The mycoplasma population is increasing. It extends to the lower parts of the urogenital tract. Cystitis, salpingitis, orchiepididymitis, and prostatitis develop. Other infections come along.
The risk of complications of mycoplasmosis increases.
Mycoplasma hominis symptoms reappeared after treatment
It happens that a person has undergone treatment for mycoplasma hominis, and the symptoms have disappeared. But time passes and they appear again.
Why is this happening?
The reasons are as follows:
- The patient did not fully recover
- He did not undergo control diagnostics and was not convinced that mycoplasma hominis was no longer in his urogenital tract
- The person became infected again
You can guess the cause by doing a blood test. Detection of class G antibodies will indicate that the infection has not gone away.  Because they are not synthesized immediately after infection.
Because they are not synthesized immediately after infection.
The production of these immunoglobulins takes a long time. If antibodies G are not detected, but immunoglobulins M are detected, most likely, we are talking about re-infection. In any case, it is necessary to undergo a second course of therapy.
If this is an exacerbation of an old infection, the doctor may change the drug. Especially if the relapse occurred in a short time after the previous inflammation. If infection recurs, the antibiotic does not need to be changed.
However, before starting treatment, you should make sure that it was Mycoplasma hominis that caused the symptoms again. To do this, it is necessary to be examined not only for mycoplasmosis, but also for other STIs.
You can take the necessary tests and receive treatment in our clinic. Experienced venereologists work here who will help you get rid of any infections of the urogenital tract.
If you suspect Mycoplasma hominis, contact the author of this article, a venereologist in Moscow with many years of experience.
Mycoplasma hominis is one of 16 types of mycoplasmas that can be found in the body. It is classified as conditionally pathogenic, but under certain conditions it can provoke pathology, the treatment of which is carried out on an outpatient basis. Let's consider the causes, signs, and methods of combating the pathogen.
Mycoplasmosis - causes
Mycoplasma in women is always present in the vaginal microflora. Its concentration is low to cause disease. With the deterioration of local immunity and the development of the inflammatory process, there is increased growth and reproduction of this tiny microorganism. The following patients are predisposed to mycoplasmosis:
- women with high sexual activity;
- having concomitant urogenital pathologies – trichomoniasis, gonorrhea;
- pregnant women.
Mycoplasma hominis is less pathogenic than other types. But the microorganism is often found in a smear when other diseases of the genitourinary system are detected: urethritis, cystitis, pyelonephritis. Doctors call such pathologies directly as a provoking agent that triggers the rapid growth of conditionally pathogenic microflora.
How is Mycoplasma hominis transmitted?
Primary infection with mycoplasma occurs during childbirth. During the advancement of the fetus along the birth canal of the mother, who is the carrier of this microorganism, penetration of the pathogen into the urogenital tract of girls is noted. In addition, intrauterine infection through the placenta is also possible (very rare). When considering Mycoplasma hominis and the routes of transmission of the pathogen, doctors put the sexual route in the first place. Unprotected sexual intercourse with a carrier of microorganisms leads to infection. Predisposing factors for this are:
- frequent change of sexual partners;
- promiscuous sexual relations.
Mycoplasma in women - symptoms
Mycoplasmosis in women, the symptoms of which are listed below, has a hidden course. Because of this, women learn about the presence of the disease after a certain time after infection. Often, the microorganism provokes other diseases of the urogenital tract, during the diagnosis of which mycoplasmas are detected. These microorganisms often provoke:
- inflammation of the uterus and appendages;
- pyelonephritis.
The immediate symptoms of these pathologies often indicate mycoplasmosis. Mycoplasmosis, the symptoms of which do not appear immediately after infection, is accompanied by copious discharge from the genital tract. This phenomenon causes a burning sensation, which intensifies during urination. Discomfort and unpleasant sensations can also accompany sexual intercourse. A feature of the disease caused by Mycoplasma hominis is the presence of periods of remission - when the symptoms disappear for a while and then reappear.

Mycoplasmosis - incubation period
Mycoplasmosis in women manifests itself after 3-55 days. This long incubation period explains the difficulty of diagnosing the disease in the early stages. Symptoms of the disease are more pronounced in men. Often, the pathology is diagnosed during a joint examination of spouses before planning a pregnancy. Obvious symptoms of the disease in women appear only during an exacerbation of inflammatory diseases of the genitourinary system. Some ladies may ignore periodic burning sensations without seeking medical help.
Discharge from mycoplasmosis
Reproduction in the reproductive system of a pathogen such as mycoplasma, the symptoms of the disease are mentioned above, is accompanied by the appearance of light discharge. At the same time, their character may be different. More often it is mucous discharge of a small volume. Their spontaneous disappearance short period creates a deceptive feeling of recovery. The appearance of pathological discharge after 2-3 weeks in a larger volume often forces the girl to consult a gynecologist.
Mycoplasma hominis - diagnosis
Diagnosis of pathology is carried out comprehensively. Analysis for mycoplasmosis allows you to identify the pathogen even at low concentrations. A smear is taken from the vagina, cervix and urethra. This study is preceded by an examination of the woman in a gynecological chair, during which the doctor may notice changes in the cervical uterus. These changes directly become the reason for a comprehensive examination of the patient.
Mycoplasma analysis
Sowing for mycoplasma is carried out with the collection of material from the urethra, vagina, and cervix. After collecting the material, it is examined under a microscope and evaluated. An additional method for diagnosing pathology, which helps to identify the pathogen at low concentrations, is PCR. This reaction detects the presence of pathogen DNA in a blood sample, so pathology can be diagnosed even in the absence of clinical manifestations of the disease.

Mycoplasma is normal
A smear for mycoplasma determines the presence of opportunistic microorganisms. However, a small amount of them is allowed and is normal. Because of this, when making a diagnosis, the gynecologist pays attention to the concentration of mycoplasmas in the results of the analysis. The borderline normal state is 104 CFU/ml. When performing PCR, the patient receives a positive result - mycoplasmas are present in the blood (carriage or acute stage of mycoplasmosis) and a negative result - there are no mycoplasmas. This analysis is used as a supplementary analysis.
Mycoplasma - treatment
Mycoplasma in women, the symptoms and treatment of which depend directly on the type of pathogen, is often diagnosed at a late stage. This necessitates long-term therapy. The basis of treatment is antibacterial drugs aimed at suppressing the growth and development of the pathogen. Medicines are selected taking into account sensitivity, so the prescription is carried out according to the results of laboratory tests.
To exclude Mycoplasma hominis, treatment is carried out comprehensively. Both sexual partners must take the course. In addition to antibiotics and physiotherapeutic procedures, the following groups of drugs are used in the treatment of mycoplasmosis:
- immunomodulators;
- antifungal;
- antiprotozoal.
Mycoplasmosis - treatment, drugs
The treatment regimen for mycoplasmosis is determined individually. When prescribing a course, doctors take into account the severity of the disease, its stage, and the presence of concomitant gynecological pathologies. Before treating mycoplasmosis, the type of pathogen is determined. The basis of therapy is tetracycline preparations:
- Tetracycline;
Macrolides are also effective in the fight against mycoplasma, which include:
- Clarithromycin;
- Azithromycin.
Doctors often prescribe fluoroquinolones as alternative antibacterial agents:
- Ciprofloxacin;
- Ofloxacin.
The course of antibiotics lasts 3-7 days. At the same time, antifungal drugs are prescribed to suppress the growth and reproduction of fungal infections, which occurs due to long-term use of antibiotics. In this case the following is prescribed:
- Clotrimazole;
- Nystatin.
At the final stage, to restore and normalize the vaginal microflora, use:
- Vagilak;
- Gynoflor.

Mycoplasmosis - consequences in women
Untimely detection of mycoplasma hominis in women can provoke diseases of the urogenital system. Due to the absence of clear symptoms when infected with Mycoplasma hominis, the pathogen is detected during the diagnosis of an existing disease of the reproductive system. Often, latent mycoplasmosis causes disorders in the reproductive system such as:
- adhesions in the pelvis;
- postpartum endometritis;
- ectopic pregnancy;
- infertility.
Avoiding casual intimate relationships and using barrier contraception helps protect against infection. A woman should be regularly examined by a gynecologist, eat well, and monitor her condition. immune system. Timely elimination of inflammatory foci in the tissues of the genitourinary system is necessary.

Characteristics of mycoplasma
 The pathogenic qualities of mycoplasma are associated with the presence of antigens, toxins, aggression enzymes and adhesins. The latter are used by microbes to early stages for fixation on epithelial cells. Toxins penetrate the blood, contributing to the development of leukopenia, hemorrhage, and swelling. The most pathogenic is Mycoplasma hominis, which most often causes inflammation of the genital organs in women. How is mycoplasmosis transmitted?
The pathogenic qualities of mycoplasma are associated with the presence of antigens, toxins, aggression enzymes and adhesins. The latter are used by microbes to early stages for fixation on epithelial cells. Toxins penetrate the blood, contributing to the development of leukopenia, hemorrhage, and swelling. The most pathogenic is Mycoplasma hominis, which most often causes inflammation of the genital organs in women. How is mycoplasmosis transmitted?
Methods of infection

There are various routes of infection, the most common of which is sexually transmitted. Transmission of the infection during fetal development or childbirth is possible. Since the microorganism is unstable in the external environment, its spread through household means is impossible.
Provoking factors that contribute to increased proliferation of bacteria include:
- long-term use of antibacterial and hormonal drugs;
- stress;
- immunodeficiency states;
- alcoholism;
- endocrine disorders;
- bacterial vaginosis;
- surgical interventions.
 The risk of infection is high if a person is promiscuous and refuses to use a condom. Most often, the disease is diagnosed in women who do not observe personal hygiene rules, homosexuals and people with other STDs.
The risk of infection is high if a person is promiscuous and refuses to use a condom. Most often, the disease is diagnosed in women who do not observe personal hygiene rules, homosexuals and people with other STDs.
Symptoms
The bacterium can cause the development of the disease immediately, or it can remain in the body without giving any symptoms. If there is one reason or another, mycoplasma is activated, causing pronounced symptoms to appear. manifested by inflammation:
- urethra;
- Bladder;
- prostate gland;
- kidney

In women it is most often found:
- vaginosis;
- cervicitis;
- endometritis;
- salpingitis.
A prolonged course of the inflammatory process can lead to infertility. It is necessary to begin treatment of urogenital mycoplasmosis in a timely manner.
The main symptoms of infection in men are pain and burning in the urinary canal, a feeling of heaviness in the groin area, radiating to the anus, problems with erection.
Activation of mycoplasma in pregnant women can contribute to damage to the brain, kidneys, skin and visual organs of the fetus. The infected child has low body weight due to impaired blood flow. Death can occur in the first days after birth. Infection in the first trimester significantly increases the risk of spontaneous abortion. With perinatal infection, meningitis or pneumonia develops.
How to detect the pathogen
 Diagnosis of mycoplasma infection begins with laboratory tests, examination of the patient and medical history. Serological tests provide detection of bacterial DNA. The material for analysis is vaginal secretion, urethral smear, and urine. The preparation is stained and examined under a microscope. If DNA of the infectious agent is detected during PCR, we are talking about the presence of urogenital mycoplasmosis.
Diagnosis of mycoplasma infection begins with laboratory tests, examination of the patient and medical history. Serological tests provide detection of bacterial DNA. The material for analysis is vaginal secretion, urethral smear, and urine. The preparation is stained and examined under a microscope. If DNA of the infectious agent is detected during PCR, we are talking about the presence of urogenital mycoplasmosis.
ELISA helps to detect antibodies to mycoplasma in the blood. The result is considered negative if all types of indicators have a sign (-). In the presence of IgG class antibodies, we are talking about the formation of immunity to the bacterium. If specific cells of type 2 are present, further diagnosis and therapy are necessary. The absence of antibodies in the blood after therapy indicates its effectiveness. To determine sensitivity to antibacterial drugs, genital secretions are placed on nutrient media.
Therapeutic measures
Broad-spectrum antibiotics (Doxycycline), macrolides (Azithromycin), fluoroquinolones (Cifran), antiprotozoal agents (Trichopol), and local antiseptics (Metronidazole suppositories) are considered the most effective. Oflokain ointment is used to treat the genital organs of men. To prevent candidiasis, which often occurs during the treatment of bacterial infections, Nystatin, Fluconazole, Clotrimazole are prescribed. Probiotics are used to normalize vaginal microflora.
Interferon and Polyoxidonium restore the functions of the immune system and increase the body's resistance. In the presence of pain, non-steroidal anti-inflammatory drugs are prescribed. Additionally, taking multivitamins is recommended. Douching with a decoction of chamomile and sage, Miramistin, helps to alleviate the condition. Both partners should be treated for mycoplasmosis at the same time. Otherwise, the risk of re-infection remains, and therapy becomes useless. A month after completion of treatment, a control test is carried out.
Prevention of urogenital mycoplasmosis involves management healthy image life. It is necessary to refuse casual sexual contacts, observe the rules of intimate hygiene, and use a condom during sex with an unfamiliar partner. The activation of mycoplasma infection is prevented by the timely elimination of foci of infection in the body. With mycoplasmosis, you should not self-medicate; if a person shows signs of the disease, he should visit a doctor and start taking medications.
18 713
Mycoplasmosis and ureaplasmosis is an inflammatory process in the organs of the genitourinary system, caused by mycoplasmas or ureaplasmas, respectively.
How does infection with mycoplasma and ureaplasma occur?
- Infection can occur through any type of unprotected sexual contact (vaginal, oral, anal) with a carrier of the infection. Depending on the state of the body (primarily the immune system), the probability of transmission of mycoplasma and ureaplasma during one-time unprotected sex is 5-60%. Women are most often asymptomatic carriers of the infection, while men become infected through sexual contact.
- Transmission of the pathogen in utero or during childbirth from an infected mother is also possible. The probability of infection reaches 50-80%.
- The everyday route of infection (in the gym, swimming pool, through a towel, dishes, dirty hands, etc.) is practically impossible, because mycoplasmas cannot live outside the body.
- Domestic animals also cannot be a source and carrier of mycoplasmas and ureaplasmas.
What happens after infection with mycoplasmas and ureaplasmas?
The mere fact of transmission of a pathogen does not mean that it will necessarily lead to disease.
Depending on whether mycoplasmas cause disease or peacefully coexist with humans, they are distinguished:
- Carriage of mycoplasmas or ureaplasmas. In this case, mycoplasmas are representatives of the natural microflora of the body and do not cause any changes in the genitourinary tract. It does not manifest itself clinically.
- The development of the disease - mycoplasmosis or ureaplasmosis. As a rule, this occurs with a decrease in local and general immunity. In this case, an inflammatory process develops in the organs of the genitourinary system.
What are the types of mycoplasmosis and ureaplasmosis?
If the transmission of the pathogen nevertheless led to the development of the disease, then depending on the time of its occurrence and the severity of the symptoms, they are distinguished:
- Fresh, i.e. new mycoplasmosis or ureaplasmosis. Depending on the severity of symptoms, it can be acute or sluggish.
- Chronic, which is characterized by an asymptomatic course and a disease duration of more than 2 months. Chronic infection may periodically worsen under the influence of various factors.
Symptoms of mycoplasmosis and ureaplasmosis.
Because Mycoplasma and ureaplasma are related bacteria, and the nature of the infection and symptoms are very similar.
Incubation period can last from 2 to 5 weeks, after which the first signs of infection appear.
Mycoplasmosis and ureaplasmosis are characterized by the absence of a pronounced immune response of the body, the absence of symptoms of infection, a long chronic course, and the absence of stable immunity. All this is explained by the characteristics of the pathogens themselves - mycoplasmas and ureaplasmas.
Mycoplasmosis and ureaplasmosis do not have any specific symptoms that would indicate them specifically. All clinical manifestations are almost the same as with other urogenital infections.
However, acute manifestations of mycoplasmosis and ureaplasmosis are extremely rare.
Most often, erased or hidden forms of these infections with rapid chronicity of the process are observed.
In this case, usually no complaints arise at all, or they are so insignificant and disappear quickly without any treatment that they are simply not paid attention to. But under certain conditions of the body, for example, stress, the previous symptoms reappear.
What is characteristic of mycoplasmosis is that, as a monoinfection, it occurs in only 10-15% of patients; in other cases, it occurs together with other microorganisms. Of these, in 25 - 30% of cases - together with chlamydia. Mycoplasmas can often be found in trichomoniasis, gonorrhea and chlamydia, so so-called mixed infections are distinguished: mycoplasma-trichomoniasis, mycoplasma-chlamydia, mycoplasma-gonococcal.
And if at first mycoplasmosis and ureaplasmosis occur as low-symptomatic urethritis or vulvovaginitis, then when it becomes chronic, the inflammatory process affects deeper parts - the fallopian tubes, ovaries, prostate, testicles.
Symptoms of mycoplasmosis and ureaplasmosis in women:
Manifestations of fresh mycoplasmosis and ureaplasmosis in women are rarely observed. Most often they are asymptomatic carriers of mycoplasmas.
But even if the disease does occur, the inflammatory process in the genitourinary organs during mycoplasma infection in women is mild and often hardly bothers us. Fresh mycoplasmosis manifests itself as inflammation of the urethra, vagina and cervix. However, pathological vaginal discharge in these diseases does not always occur. In addition, it is impossible to distinguish them from normal discharge without tests.
However, if complaints do arise, they are often like this:
- Slight clear vaginal discharge, maybe a little more than usual.
- Slight pain and burning when urinating.
- Brownish spotting before or after menstruation.
- Pain in the lower abdomen and during sexual intercourse.
- Slight itching of the external genitalia.
- Seeing a doctor, as a rule, is associated with complications of mycoplasmosis, for example, infertility, miscarriage, menstrual irregularities, inflammation of the ovaries, etc.
Ureaplasmas, unlike mycoplasmas, do not have the ability for deep invasion, therefore they damage only the superficial epithelium of the external genitalia.
Symptoms of ureaplasmosis and mycoplasmosis in men
In men, carriage is much less common than in women, and fresh mycoplasmosis causes inflammation of the urethra and foreskin. These infections also do not cause any particular concern for men, but signs of the disease appear more often and are more pronounced than in women.
- Moderate pain and burning in the penis area, intensifying during urination or sexual intercourse.
- Redness and irritation of the urethral sponges.
- Slight transparent discharge from the urethra.
- Unpleasant sensations or soreness in the testicular area.
- Nagging pain and discomfort in the lower and deep abdomen, as well as in the perineal area.
- There may be some weakening of potency.
Complications of urogenital mycoplasmosis, ureaplasmosis.
- Miscarriage (spontaneous miscarriage or premature birth). Often associated with autoimmune processes. Mycoplasma infection leads to termination of pregnancy in 70 - 80% of cases.
- Complicated pregnancy - late toxicosis, polyhydramnios, threat of miscarriage, premature placental abruption and its abnormal attachment. More often associated with autoimmune processes.
- Urethritis, cystitis, pyelonephritis, urolithiasis.
- Endometritis, salpingitis, salpingoophoritis, adnexitis, endocervicitis and cervical erosion.
- Conjunctivitis.
- Autoimmune diseases (most often arthritis of the knee, ankle and hip joints).
- Epididymitis with nagging pain in the groin, perineum, scrotum, enlargement of the epididymis and redness of the skin of the scrotum.
- Prostatitis with frequent painful urination, pain in the lower abdomen and perineum, decreased erection and potency, painful, erased early orgasm. If more than 104 colony-forming units per 1 ml of mycoplasmas or ureaplasmas are found in the secretion of the prostate gland, this indicates that these pathogens cause prostatitis.
- Female and male infertility. In women, with a prolonged course of the inflammatory process, changes occur in the fallopian tubes and uterine mucosa. In men, spermatogenesis is disrupted: the number of sperm and their motility decreases, immature forms and morphological changes appear in them.
- Intrauterine infection of the fetus.
- Mycoplasmas and ureaplasmas are capable of causing chromosomal changes in cells, including reproductive cells (sperm and eggs). This can cause spontaneous abortions, as well as chromosomal abnormalities in the fetus and birth defects development.
At an appointment with a gynecologist, even an absolutely healthy woman can receive test results that reveal mycoplasma. Conditionally pathogenic flora, which doctors take into account only if titers are high, is quite common.
If the growth of flora is very active and there are prerequisites for a decrease in the immune system, then a diagnosis of mycoplasmosis is made. Let's figure out what it is and what treatment methods can overcome these microorganisms.
Causes
Why does mycoplasma occur in women, and what is it? Mycoplasma is considered the smallest form of organisms belonging to the mycoplasmataceae family. It is considered a cross between unicellular organisms and multicellular viruses and bacteria.
Despite this, scientists tend to consider them (mycoplasmas) more like viruses, since they do not have a cell membrane. In the mycoplasmataceae family, there are two genera of microorganisms, mycoplasma and ureaplasma, which can cause the development of a wide variety of diseases.
The source of infection is a person with manifest or asymptomatic mycoplasmosis. The infection is transmitted by airborne droplets (with respiratory mycoplasmosis), sexually (with urogenital mycoplasmosis) and vertical (from mother to fetus - more often with urogenital mycoplasmosis) routes.
The incubation period of the disease is from 3 days to 5 weeks, on average 15-19 days.
Symptoms of mycoplasma in women
 As a rule, the presence of mycoplasmas in the body is characterized by erased, low-symptomatic forms. Approximately 10-20% of women do not feel any obvious symptoms of mycoplasma until a stressful situation, such as abortion or severe hypothermia, activates the infection, often leading to quite serious complications.
As a rule, the presence of mycoplasmas in the body is characterized by erased, low-symptomatic forms. Approximately 10-20% of women do not feel any obvious symptoms of mycoplasma until a stressful situation, such as abortion or severe hypothermia, activates the infection, often leading to quite serious complications.
Urogenital mycoplasmosis in women it manifests itself as:
- (gardnerellosis);
- mycoplasma urethritis;
- inflammation of the uterus, fallopian tubes and ovaries;
- mycoplasmosis is often combined with and.
The insidiousness of mycoplasma in women is that the disease can be completely asymptomatic for many years. During this period, the woman is a carrier of the infection and can transmit it to her sexual partners.
Diagnostics
Diagnosis of urogenital mycoplasmosis is based on the PCR (polymerase chain reaction) method, which determines the DNA of mycoplasmas. They also use the classic cultural method, with sowing the material on a liquid medium and then reseeding it on a solid one.
Mycoplasmas are identified by the fluorescence of colonies after the addition of specific antisera. Serological methods for detecting mycoplasmas are the complement fixation reaction (CFR) and the indirect agglutination reaction (IRGA).
As a material for laboratory research In women, a smear is taken from the cervix, vestibule of the vagina, urethra and anus, and the first portion of urine in the morning.
Treatment of mycoplasma in women
When diagnosing mycoplasma in women, the attending physician prescribes a treatment regimen consisting of complex therapy, including:
- Antibacterial drugs(due to the resistance of mycoplasma to penicillin, antibiotics for mycoplasmosis are used from the tetracycline group, and macrolides are also used; the course of this treatment is up to 2 weeks);
- Local treatment (suppositories, douching);
- Immunomodulators (these drugs enhance the effect medicines, use cycloferon or lykopid in treatment);
- Compliance with the diet recommended by the doctor;
- Physiotherapy.
Unfortunately, the human body is not able to develop immunity to this infection, and therefore both sexual partners need to be treated with drugs at the same time. On average, the course of treatment for mycoplasmosis is 10 days. Then, after 2 or 3 weeks, the patient is prescribed bacterial culture, and after 30 days - PCR.

Chronic form
In the treatment of chronic forms, immune-oriented and local therapy. The goal of immune-oriented therapy is to correct the immunodeficiency state that caused chronic course illness and intensified against its background. It is prescribed taking into account immunogram parameters.
Local therapy is carried out simultaneously with systemic antibiotic therapy for 5-7 days. Typically, ethmotropic, anti-inflammatory drugs and enzymes (trypsin, chymotrypsin, etc.) are prescribed in the form of installations or using cotton-gauze swabs to treat the vagina. Immediately after its completion, it is recommended to undergo a course of treatment with probiotics to restore the microflora.
Consequences
A long course of mycoplasmosis without symptoms leads to the development of endometritis - inflammation of the uterine mucosa. In women with mycoplasma endometritis, miscarriages and missed pregnancies are common.
From the uterus, M. hominis and M. genitalium can spread to its appendages with development. Then adhesions appear in the tubes, which can lead to an ectopic pregnancy.