Balanoposthitis - classification, causes, symptoms, diagnosis, treatment, complications and prevention. Adhesive (adhesive) balanoposthitis Bacterial balanoposthitis in men
Balanoposthitis is a fairly common inflammatory disease of the skin of the penis. According to statistics, every year 11% of men on Earth suffer from this disease. Balanoposthitis in men, according to ICD-10 (international classification of diseases), is a double disease, as it involves an inflammatory process in both the head and the inner layer of the foreskin.
Causes of the disease
Acute balanoposthitis develops due to the following factors:
- mechanical damage to the penis;
- washing the foreskin with medications;
- increased concentration of salts in urea;
- uncontrolled use of various medications that lead to irritation of the skin of the head of the penis;
- an infection located in the genital tract, which got there from other organs or from an infected partner.
The reasons that cause the appearance of the disease determine the nature of its course. For example, balanoposthitis in men can be characterized by both the appearance of irritation and erosions on the skin.
Symptoms
The main symptoms of balanoposthitis are:
- burning and itching sensation in the penis area. It is the most common reason for visiting a doctor;
- redness and swelling of the foreskin;
- the appearance of foreign secretions that have an unpleasant odor and purulent nature;
- the presence of detachments of the upper tissue (erosion);
- growth of lymph nodes;
- general weakness;
- headache;
- high body temperature;
- (cessation of opening of the head of the penis, which occurs due to the presence of edema).
If there is no timely treatment for balanoposthitis, then the process of tissue death in the penis area will soon begin.
Characteristic signs of the disease include:
- the appearance of edema;
- hyperemia (flush of blood) to the head of the penis;
- the appearance of spots with defined boundaries of different shapes, sizes and scarlet colors;
- burning and itching, which intensifies during urination and sexual intercourse;
- increased libido, which causes inflammation of the receptors on the head of the penis;
- curdled or purulent discharge with an unpleasant odor;
- cracks in the foreskin;
- fibrosis of the penis.
Candidiasis balanoposthitis in men is a common type of disease that is caused by the yeast type Candida fungus. Typically, men need to be treated for balanoposthitis and balanitis at the same time. Most often the disease occurs in patients. Rare cases suggest the development of the disease against the background of phimosis existing from birth or too long foreskin.
If the patient is diagnosed accordingly, then, in addition to taking medications (antibiotics, antifungal agents), it is necessary to follow a certain diet. The patient will need to completely exclude sweet, spicy or pickled foods from the diet. The consumption of alcoholic beverages is also strictly prohibited.
If a patient is diagnosed with a candida variety of the disease, then he is also recommended to abstain from sexual activity during treatment. If the disease is caused by phimosis, then doctors must dissect the flesh of the penis, and in some cases the patient is also circumcised. If phimosis is absent, then only conservative methods (broad-spectrum drugs) are used for treatment.
It is worth remembering that neglecting to see a doctor can cause inflammation of not only the penis, but also the lymph nodes in the groin, which will lead to the formation of gangrene, and in some cases, death. Therefore, a man should always remember the importance of maintaining genital hygiene.
Types and forms of the disease
The disease, depending on its occurrence and form of progression (according to ICD-10), is divided into:
- acute balanoposthitis. Has more pronounced symptoms and is characterized by faster progression;
- chronic balanoposthitis. It may have phases of remission and relapse, while the symptoms are less pronounced.
The main forms of balanoposthitis include:
- ordinary. Accompanied by inflammation, which over time contributes to the appearance of erosive wounds from which pus is released;
- gangrenous. This type is often complicated by the presence of phimosis. With gangrenous balanoposthitis, the resulting ulcers take a very long time to heal;
- erosive. A large amount of purulent discharge contributes to the appearance of erosive areas that are white in color. Also, characteristic erosive wounds with defined boundaries appear on the head of the penis.
Chronic balanoposthitis is presented in the following forms:
- candidal balanoposthitis. This type of disease affects men much less frequently than women due to the anatomical features of the location of the genital organs. Candidiasis balanoposthitis in males can be triggered by a weakened immune system. In this case, the foreskin is affected, on which a characteristic white coating forms. If it is removed, ulcers and redness may appear in its place. The patient complains of burning or itching during sexual intercourse or when urinating. Candidiasis balanoposthitis is contagious, and is transmitted from an infected partner to a healthy one. Therefore, this disease should be treated in two partners at once;
- allergic balanoposthitis. The patient complains of symptoms typical of the disease (pain, itching, inflammation of the tissues of the foreskin). A characteristic sign is the appearance of blisters or spots. Such chronic balanoposthitis can be caused by the patient having an allergy to latex (a common cause of the development of pathology), eating foods with allergens, as well as the use of local contraceptives;
- circinar balanoposthitis. With this type, spots with clear boundaries form on the head of the penis. They usually arise due to the presence of chlamydial-type diseases or are one of the symptoms. Inflammation occurs on the penis. If left untreated, white or gray spots form on the surface of the penis. As a result, tissue necrosis develops. This type of disease is characterized by the appearance of ulcers that are gangrene-like;
- anaerobic balanoposthitis. It is characterized by the occurrence of an inflammatory process in the prepuncial sac. Anaerobic balanoposthitis is usually provoked by gram-negative microorganisms and can occur in the form of erosion. A mild form of the disease has the following symptoms: the presence of a sticky coating on the head, as well as an unpleasant fishy odor. Anaerobic balanoposthitis requires specific treatment from a qualified specialist;
- ulcerative balanoposthitis. It is characterized by the appearance of a large number of ulcers from which pus is released. The disease is caused by fungi, staphylococci and other pathogenic microorganisms. The patient complains of swelling and a burning sensation on the head of the penis. In addition, the patient may be bothered by pain in the groin and general weakness of the body.
Complications that may arise from the disease include, in addition to phimosis, decreased sensitivity on the head of the penis. This is caused by the fact that the receptors atrophy during the inflammatory process. If the infection gets into the urinary canal, it will also cause. The most serious complication is paraphimosis, in which the head of the penis is pinched due to the fact that the foreskin begins to scar.
Diagnostics
A urologist makes a diagnosis to the patient. When a disease is detected, he prescribes the patient to undergo several tests, such as:
- taking material for bacterial culture. It is taken from the affected areas of the foreskin;
- conducting a potassium hydroxide test if the doctor suspects that the patient is developing a fungal type of illness;
- PCR (polymerase chain reaction).
In order to prescribe the correct treatment, it is necessary to clarify the cause of the development of the pathological process.
It is noted that the disease is quite rarely caused by diseases that are sexually transmitted. At the same time, chronic infection reduces the human body’s resistance to other diseases, which increases the likelihood of developing an illness caused by nonspecific flora. In addition to the urologist, the patient will also be referred to an allergist and dermatovenerologist. He may be prescribed tests to detect diabetes mellitus, since the latter is a common cause of pathology.
Treatment of the disease
A treatment plan for the disease is developed by a specialist only after preliminary diagnosis. It is the results of tests and analyzes that can provide the most complete information about the patient’s health status. Treatment of balanoposthitis involves:
- conservative methods. Antifungal drugs are used to treat the fungal form of the disease. If hormonal levels or metabolism are disturbed, then treatment is adjusted taking into account this problem, since reduced immunity will not contribute to achieving the desired effect during treatment. To overcome the pathology, a man is prescribed Mikosist, Fluconazole or other similar drugs that are prescribed to him by a doctor. Ointments are also used, which are a convenient and inexpensive way to relieve symptoms. Most often, specialists prescribe xeroform or prednisolone ointments. If there is deep damage to the tissues of the penis, doctors must prescribe antibiotics;
- surgical intervention. It is carried out if a severe stage of the disease has developed, which is often accompanied by phimosis. To cure the patient, doctors resort to cutting the foreskin, which has been narrowed as a result of inflammation. Also, in some cases, circumcision of the foreskin is required;
- unconventional methods. These include the use of folk remedies, such as compresses, as well as baths with the addition of herbal tinctures.

For various forms of the disease, a urologist may prescribe:
- medications that are aimed at eliminating inflammation, removing the causative agent of infection and reducing symptoms;
- corticosteroids, combination drugs such as Levomekol or Triderm;
- medications that increase the body’s resistance to various pathogens;
- antifungal agents (for yeast-type balanitis), such as Nizoral or Clotrimazole;
- antibiotics if the patient is diagnosed with an anaerobic type of disease.
Self-medication can be dangerous to the health and even life of the patient, so folk remedies can only be considered as an auxiliary treatment that alleviates symptoms, but not as the main one. In addition, treatment of balanoposthitis at home should be carried out only with the permission of the attending physician and under his constant supervision. If the doctor has approved the use of certain treatments at home, they can be used, but very carefully.
First of all, when treating a disease at home, you need to remember the need to wash the glans penis. This can be done under running water with the addition of regular soap. Often this is enough to reduce the symptoms. If balanoposthitis does not go away, then the head of the penis is additionally treated with antiseptic agents after each wash. You should not use iodine or potassium permanganate for washing at home - they will only cause dryness in the already inflamed tissue.
Among the traditional methods of treatment, the following are the most popular ways to alleviate the symptoms of pathology:
- black currant leaves. They are brewed in boiling water. The resulting decoction should be taken several times before meals to improve the general condition. In addition, in parallel with the decoction, it is recommended to eat fresh currant berries;
- To cure urethritis that appears as a result of illness, you need to pour milk over the parsley and then put it in the oven at low temperature. After a slight boiling of the milk, the resulting parsley decoction should be drunk every hour, a tablespoon;
- For inflammatory processes of the foreskin, a tincture of water paint is used. One spoon of this herb is poured into a glass of hot water and then infused. You need to drink the decoction 20 minutes before meals;
- If the patient has candidal inflammation, then the calendula flowers must be filled with olive oil. The resulting mixture is covered with a lid and left warm for 3 weeks. After this, you need to strain the olive oil and anoint the affected tissues with it.
Balanoposthitis (ICD 10 code N48.1) is an inflammatory disease, as a result of which the foreskin and head of the male penis are affected. According to statistics, about 11% of men have this diagnosis. But there are cases of the disease being detected in women and children. Your doctor can tell you how to treat balanoposthitis after an examination and some tests. The main therapy is the use of local medications (creams, ointments, etc.).
Treatment of the pathology can be quite long and continues until the symptoms and cause of balanoposthitis are completely eliminated. The duration of the course of therapy is influenced by the form of the disease, the severity of symptoms and the type of pathogen. Acute balanoposthitis is treated within 2-3 weeks.
Urologist Oleg Aleksandrovich Junker will tell you about the disease:
Before starting treatment, the patient needs to review the correctness of hygiene procedures and, together with his sexual partner, be examined for possible STDs. Only after this, the doctor (urologist and venereologist) will be able to prescribe the correct treatment.
If you do not pay attention to the problem in time, the disease can become chronic. Chronic balanoposthitis is much more difficult to treat.
Causes of the disease
All causes that can lead to the appearance of balanoposthitis are infectious and non-infectious in nature.
Infectious causes include:
- Candidiasis.
- Human papillomavirus.
- Trichomoniasis.

Genital herpes is a viral infection of the genital mucosa, characterized by the appearance of a group of blisters, and then erosions and ulcers
- Herpes is genital.
- Streptococci.
- Staphylococci.
- Syphilis.
- Gardnerellosis.
Non-infectious causes include:
- Psoriasis.
- Irritative balanoposthitis.
- Lichen planus.
- Diabetes.
Risk factors contributing to inflammation are:
- Failure to comply with hygiene rules.
- Decrease in the body's defenses.
- Allergic diseases.

- The presence of a chronic infection in the body.
- Infections of the genitourinary system (urethritis, etc.).
- Promiscuous sexual intercourse.
Symptoms of the disease
The main cause of balanoposthitis is considered to be the patient's failure to comply with personal hygiene rules. Signs of the disease depend on the stage of the pathological process.
Simple balanoposthitis
This is the mildest form of the disease. Its manifestations include:
- Feeling of burning and itching. This symptom is considered the very first. When touching the head of the penis, urinating or rubbing against clothing, the unpleasant sensations intensify.
- Discomfort when opening the head of the penis.
- Redness of the affected area. Thus, the inflammatory process makes itself felt.

The table shows general and local symptoms, as well as complications of the disease
- Swelling of tissues.
- Formation of painful cracks and erosions (erosive balanoposthitis).
- Discharge of pus from the urethra. This is how purulent balanoposthitis manifests itself.
Gangrenous balanoposthitis
This form of the disease is considered the most severe. Its signs are:
- Phimosis.
- Ulcers.
- Violation of the patient's condition.
- Appearance of scars.
- Perforation of the foreskin.
Balanoposthitis caused by STIs
Symptoms of the disease will depend on the type of pathogen:
- The gonorrheal type, in addition to the classic signs of balanoposthitis, is accompanied.
- Chlamydial - characterized by clear red spots.
- Trichomonas - pus accumulates under the foreskin. The head swells and turns red.
- Candidiasis is accompanied by itching, burning and pain in the head area. After some time, a cheesy discharge from the urethra appears.
- Herpetic. On the foreskin, bubbles with clear liquid inside can be noted. After opening them, red sores appear in this place. Often this type of disease is chronic.
Immunologist Ermakov Georgy Aleksandrovich will talk about the symptoms and treatment of the disease:
- Syphilitic - diagnosed when a primary chancre is present on the skin.
- Papillomavirus is accompanied by the appearance of condylomas.
- Balanoposthitis with gardnerellosis occurs with virtually no symptoms. If the patient works well the immune system, then after a few days, the disease goes away on its own.
- Circinar balanoposthitis appears as clear red spots on the head of the penis.
The disease is caused by nonspecific causes
In this case, the signs of balanoposthitis will depend on the primary disease:
- With diabetes mellitus, the head of the penis turns red, its sensitivity increases, pain and cracks are possible, in place of which scars remain.
- Psoriatic balanoposthitis is manifested by the appearance of red scales.
- With lichen planus, irregularly shaped nodules appear on the head, covered with white scales. The skin becomes red.
Features of the disease in a child
Sometimes small children can also experience the disease. As a rule, they are diagnosed with irritative or simple infectious balanoposthitis, which lasts for 5-6 days, after which it goes away.
Among the reasons for its appearance in children are:
- Developed foreskin, hanging down and difficult to move.
- Phimosis.

- Copious discharge of sperm, which accumulates in the fold between the foreskin and the head of the penis.
- Failure to comply with simple hygiene rules.
Diagnostics
To make a diagnosis and prescribe treatment, the doctor will examine the patient and prescribe some tests:
- A general blood test, in which you can see the presence of an inflammatory process by the number of leukocytes and ESR.
- A general urine test, in which an increased number of leukocytes will indicate the presence of inflammation.

A blood test for ESR is a nonspecific indicator that makes it possible to detect inflammation of various origins
- Bacterial urine analysis to identify the pathogen and its sensitivity to antibacterial drugs.
- PCR will make it possible to isolate the DNA of the pathogen and determine its type.
- Scraping from the urethra for the presence of Treponema pallidum.
If inflammation has resulted sexually transmitted infection, then it is necessary to examine your partner as well.
Complications
Patients whose immune systems are weakened, as well as those who do not observe personal hygiene rules and do not carry out treatment, may develop complications:
- Chronic balanoposthitis may occur if treatment is not started or completed on time ahead of schedule. In this case, remission is possible at first, but later the symptoms of the disease will worsen again. Treating chronic pathology is much more difficult.
- Decreased sexual function. The inflammatory process can lead to receptor atrophy and decreased sensitivity. At the same time, potency decreases.
- Cystitis, prostatitis and other diseases of the genitourinary system. Pathogenic bacteria that cause balanoposthitis can rise up the urethra and cause these diseases. As a rule, this occurs in people with reduced immunity and those who have not followed the principles of treatment.

Symptoms and complications of prostatitis
- Lymphangitis is the transition of the inflammatory process to the inguinal lymph nodes.
- Paraphimosis is compression of the head by the foreskin. In this case, there is a disturbance in the blood circulation of the organ, lymph flow and an increase in the size of the head of the penis, which becomes red and painful. This condition requires immediate medical attention, otherwise gangrene is possible.
- Gangrene of the penis is characterized by the death of tissue that turns black. The disease begins suddenly for a man. As a result, his general condition worsens, the temperature rises and foci of necrosis appear.
Treatment
How to cure balanoposthitis? This question will be answered by the doctor after examination and passing the necessary tests that can identify the causes of the inflammatory process.
Each patient must follow certain rules:
- Maintain penile hygiene.
- Eliminate the causative agent of inflammation. For this, antiseptic solutions, herbal tinctures, etc. can be used.
- Carry out antibacterial and antiviral therapy using medications. Only the attending physician can prescribe an individual treatment regimen.
Nikolai Konstantinovich Soloviev, urologist-andrologist at the Moscow Doctor medical center, will tell you what causes the disease and how to treat it:
Main methods of treatment:
- Taking medications (tablets, ointments, solutions) prescribed by a doctor. So “Levomekol” for balanoposthitis is considered a fairly effective drug.
- In case of complications, medications are used that can increase the body's defenses.
- The fungal type of disease is treated with antifungal agents (Nizoral ointment, Clotrimazole, etc.).
- For anaerobic form, antibiotics are indicated (Azithromycin, etc.).
- A surgical intervention that involves excision of the foreskin. In such cases, the patient should not try to open the head on his own, as this can lead to microcracks and further aggravate the inflammatory process.
- It is possible to treat balanoposthitis in men with folk remedies. Decoctions and infusions of medicinal herbs can alleviate the general condition of the patient and reduce the manifestations of the inflammatory process. Doctors recommend doing baths, compresses and rubbing the penis with such drugs.
Use of antibacterial drugs
Very often, the cause of inflammation is pathogenic microorganisms, including: E. coli, staphylococci, streptococci and other aerobic and anaerobic bacteria. In such cases, the doctor will prescribe the patient a course of antibacterial therapy. Depending on what caused the pathogen, broad-spectrum antibiotics are prescribed:
- Antibacterial drugs are prescribed only in cases of severe forms of the disease or when balanoposthitis is caused by sexually transmitted infections.
- Antibacterial therapy is not prescribed when allergic, viral or fungal balanoposthitis is diagnosed.
- Antibiotics for balanoposthitis, which are considered the most effective, are Doxycycline and Levomycetin tablets.
- The following drugs are often prescribed: Erythromycin, Roxithromycin and Oletetrin, quinol derivatives Nevigramon, nitrofuran Furagin or oxyquinoline Nitroxoline.

Azithromycin is an effective antibacterial agent. Price in pharmacies from 32 rubles.
- Anaerobic balanoposthitis is treated with Azithromycin.
- When diagnosing a specific infection, penicillins and cephalosporins (Tsiprolet) are prescribed.
- Treatment of candidal balanoposthitis in men is carried out with Fluconazole or Clotrimazole.
- Chlamydial and ureaplasma types of balanoposthitis are treated with metronidazole derivatives.
Along with tablets, injections and intravenous infusions of medications are used for systemic treatment, depending on the symptoms and severity of the disease.
If balanoposthitis is bacterial in nature, then both partners should take antibacterial medications. During treatment, you should avoid drinking alcohol and having unprotected sex.
Use of ointments
For local treatment of balanoposthitis, various ointments are widely used:
- If the disease is fungal in nature, the ointment should have an antifungal effect. These drugs include: “Fluconazole”, “Candide”, etc. “Clotrimazole” for balanoposthitis is the most popular of this group of drugs. No less effective is the Pimafukort ointment, which incorporates the properties of antifungal and hormonal drugs. It is often prescribed if it is necessary to cure chronic candidiasis balanoposthitis.
- In case of allergic or autoimmune inflammation, doctors recommend using hormonal ointments “Oxycort”, “Lamisil”, “Locacorten”, etc.

Bandages with ointment are applied to the damaged areas at night after careful hygiene of the genitals. This procedure is carried out within 5 days. Treatment must be carried out under the supervision of a doctor
- "Triderm" for balanoposthitis is recommended to be used when a mixed type of infection is detected in the patient. The ointment has antibacterial, antifungal and hormonal effects.
- For nonspecific bacterial infections, the combined ointment “Levomekol” is used. It contains chloramphenicol, which has an antibacterial effect, and methyluracil, which is capable of restoring damaged tissue.
- Baneocin ointment for balanoposthitis has a powerful antibacterial effect. The bacitracin and neomycin included in its composition can cope with the infection and relieve the inflammation process.
Ointments should be used for a long period of time. In this case, they are applied to the affected area several times a day.
Ointments cannot be used to treat balanoposthitis if the patient has:
- Malignant neoplasms.
- Trophic ulcers.
- Cutaneous tuberculosis.
- Necrosis.
- Allergy to individual components of the drug.
What ointments are used for the disease? Venereologist, urologist Sergey Gennadievich Lenkin will tell you:
Before you start using any drug, you need to do a test. To do this, apply a small amount of ointment to the back of the hand or near the elbow. If after some time redness, itching, rash or burning occurs in this area, then this remedy should not be used.
If you use the ointment in large quantities, symptoms of overdose may occur: redness, swelling, rash. Periodically, any drug must be changed, since long-term use can reduce its effectiveness.
Use of antiseptic solutions
For local treatment of the disease, various antiseptic solutions are often used. They can be used at home. The most popular are:
- Water-based Chlorophyllipt solution. It has anti-inflammatory and antibacterial effects.
- Erosive balanoposthitis, accompanied by the formation of ulcers and erosions, is treated with “Fukorcin” (Castellani liquid), which can cope not only with pathogenic bacteria, but also with fungi.
- Chlorhexidine is used to disinfect and treat inflammation. The solution is used for washing, lotions, baths and applications. Miramistin has a similar effect. But when using these solutions you need to be careful, as there is a possibility of damage to the mucous membrane and dry skin.
Using baths
If the disease does not have complications such as phimosis, the doctor may recommend medicinal baths. To prepare them, you can use “Furacilin”, “Dioxidin” or “Miramistin”. The duration of the procedure should not exceed 15 minutes. To achieve maximum effect, the penis should be carefully moistened with the solution. After the bath, the site of inflammation is carefully wiped with a sterile napkin and treated with any antiseptic drug.

Chamomile decoction baths are prepared as follows: add about 20 grams of chamomile flowers to a liter of hot water. Use the resulting solution for disinfectant lotions.
A doctor may recommend the following baths:
- If yeast-like fungi are detected in the test results, you should use baking soda, which dissolves in warm water.
- If you have phimosis, then after surgery you should use baths with decoctions of medicinal herbs (chamomile, calendula or sage).
- When balanoposthitis has become chronic, the patient is prescribed baths with Miramistin. Additionally, it is necessary to use corticosteroids (Prednisolone ointment, Oxycort, etc.).
Use of folk remedies
Treatment of balanoposthitis at home can be supplemented with folk remedies. It has been proven that some medicinal herbs can relieve inflammation, eliminate burning sensations and other signs of the disease. To the most popular means traditional medicine include:
- Aloe leaves have anti-inflammatory effects. They are applied to the affected area, having previously been peeled.
- Compresses with a decoction of chamomile. To prepare it, dried flowers are poured with boiling water and kept in a water bath for 5-10 minutes. After cooling, the broth is filtered and used to prepare compresses.

Preparation of a product from olive oil and calendula tincture
- Treatment of erosive balanoposthitis involves the use of olive oil and tincture made from calendula. To prepare the product, one spoon of dried calendula flowers is poured with 70 ml of olive oil. You need to infuse the drug for 3 weeks, placing it in the sun. When the tincture is ready, wipe all the sores and cracks with it.
- Plantain is considered an excellent anti-inflammatory agent. The leaf of the plant should be washed well and applied to the sore spot, secured with a gauze bandage. Every half hour, the bandage with the sheet should be changed to a new one.
Dear readers, from the video below you will learn some tips on how to treat pathology at home:
- A good remedy considered to be sage, which is used to prepare baths. To do this, pour a few tablespoons of dried herbs into 500 ml of boiling water and leave in a water bath for 5-10 minutes. After complete cooling, the broth is filtered and used for baths, rubdowns or lotions.
- St. John's wort has medicinal properties. A decoction of it is prepared and used in the same way as the sage remedy.
Treatment of balanoposthitis with folk remedies will only be effective if used regularly over a long period of time. It is important to pay attention to the characteristics of your body and possible individual intolerance to traditional medicine.
List of popular medicines
Treatment of balanoposthitis is inextricably linked with the use of medications. A special place is given to local drugs:
- "Miramistin" is the best ointment for treatment, which has a bactericidal effect. Due to its wide spectrum of action, it is prescribed for the treatment of any type of balanoposthitis. The ointment has one side effect - a burning sensation, which goes away on its own after a few minutes. The medicine is not prescribed to people with individual intolerance to its individual components.
- "Levomekol" - helps speed up the healing process. The ointment has proven its effectiveness against many bacteria (aerobes and anaerobes). In case of individual intolerance to its components, an allergic reaction is possible.
- "Triderm" is able to treat balanoposthitis not only at the initial stage, but also when the disease has become chronic. The active components of the ointment are able to relieve inflammation, have antiallergic, antifungal, and antibacterial effects. The drug should be used several times a day for 2-4 weeks. In case of intolerance to the components of the drug, irritation, itching, dry skin, and the appearance of a rash are possible. Triderm should not be used for skin tuberculosis, chickenpox, or skin reactions that occur as a result of vaccination.
- "Furacilin" is used to prepare baths or lotions. The medicine has a broad antimicrobial effect. Skin reactions in the form of rashes and dermatitis are possible. With prolonged use, nerve inflammation may occur. People with kidney disease should be careful.

A very effective remedy. Its price is low, within 100 rubles
- Chlorhexidine is an antiseptic that can be used for rinsing, lotions, baths or compresses. It is allowed to be introduced into the urethra. Adverse reactions are extremely rare and manifest themselves in the form of itching, rash or dry skin. Chlorhexidine does not cause an overdose.
- Hydrogen peroxide is used for disinfection. To do this, it is used to treat the affected areas of the skin. Among the disadvantages of the product is a temporary effect that completely disappears a few hours after use. It is recommended to use peroxide when the first signs of balanoposthitis occur. It is not used if the patient has phimosis.
- Clotrimazole is known for its antimicrobial effect. The medicine is prescribed for candidal balanoposthitis. To do this, the ointment is applied to the skin after hygiene procedures. The duration of use depends on the severity of the disease. In some cases there were adverse reactions(redness and burning of the skin). In this case, the drug should be discontinued and reused only after the side symptoms disappear. "Clotrimazole" is not prescribed to children and people with hypersensitivity to its components.
- Potassium permanganate has excellent antiseptic properties and accelerates the healing process of wounds. It can be used at different stages of pathology. But this must be done carefully, since undissolved grains of potassium permanganate can cause a severe burn. It has no contraindications for use.

In addition to treating inflammation, potassium permanganate baths can be prescribed as additional hygiene measures for patients
- Fluconazole is effective only in the case of candidiasis balanoposthitis. It is quickly absorbed into the skin and acts for a long period of time. Analogues of the drug are ointments "Flucostat" and "Diflucan".
- "Bepanten" is used to speed up the healing process of wounds. The ointment has an anti-inflammatory, moisturizing and regenerating effect. The cream is prescribed for the prevention and treatment of balanoposthitis. It is applied to clean and dry skin several times a day. The duration of use depends on the degree of damage and the individual characteristics of the patient. In some cases, a skin reaction may occur, so it is better not to use it for people with high sensitivity to the active components of the drug.
- "Pimafukort" has powerful anti-inflammatory, antifungal and antibacterial effects and is effective against many pathogens. With prolonged use, stretch marks may appear at the site of application. The medicine is not prescribed to children under 1 year of age and to those who are allergic to certain components of the ointment.
- "Fukortsin" is prescribed as an antimicrobial and antifungal agent. It is used to prepare baths, compresses and applications. After it dries on the skin, the treated area must be lubricated with cream. A possible side effect is burning. "Fukortsin" is not used in case of high sensitivity of the patient's body to its components. It is not recommended to treat large areas of skin with it, since the active components can penetrate the bloodstream and have a toxic effect.

Fukortsin is an antiseptic solution with high bactericidal and disinfectant properties. average price in pharmacies from 75 rubles.
- “Syntomycin ointment” for balanoposthitis is a broad-spectrum antibiotic. It is active against many pathogenic bacteria. It is applied to the affected areas in a thin layer several times a day for 3-5 days. With long-term use, the medicine may cause side effects such as itching, burning and redness of the skin.
- Tetracycline ointment has an antibacterial effect and can stop the proliferation of pathogenic microflora.
Is balanoposthitis contagious?
If not treated promptly, this disease can cause a lot of unpleasant consequences. Therefore, many men are interested in the question: “Is balanoposthitis contagious and can it be contracted from a partner?” Urologists assure that this disease is not contagious. However, there are a number of infections that are sexually transmitted and can cause inflammation of the foreskin and glans penis.
Another question that often arises among men: “Is it possible to go to a sauna or bathhouse if you have balanoposthitis?”
Water procedures have a good effect on the patient’s condition, but in this case, a sauna would not be the best option. This is due to the fact that:
- In such places there is a risk of contracting various infections, which will negatively affect the patient’s condition.
- At elevated temperatures, existing bacteria will develop more rapidly.
Therefore, until complete recovery, it is better to avoid visiting such places.
At first glance, balanoposthitis is a harmless disease. But if you don’t pay attention to it in time, the consequences can be extremely unpleasant. The course of treatment should be prescribed by a doctor after identifying the causes of the disease.
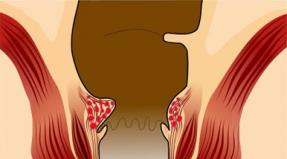
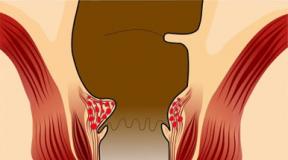
Balanoposthitis- an inflammatory process that spreads to the foreskin and glans penis. In the majority of cases, the inflammation affects both the head and the foreskin, however, in medical terminology, a distinction is made between balanitis (inflammation of the head of the penis) and posthitis (inflammation of the foreskin). Since, in the presence of the foreskin, its inner layer always comes into contact with the head, the inflammation spreads to both elements.
Consequently, posthitis and balanitis in the vast majority of cases develop simultaneously and are combined under one term - balanoposthitis. Of course, this disease can only develop in uncircumcised men, since otherwise there is no foreskin. Balanoposthitis can have different courses depending on the location. The inflammatory process develops due to a combination of several factors.
Classification of balanoposthitis
Balanoposthitis, as a disease, has a lot of distinctive subtypes, which are classified according to foci of inflammation, pathogens and severity of the lesion.
Classification of balanoposthitis by pathogens
- Candidiasis balanoposthitis;
- Chlamydial balanoposthitis;
- Circinar balanoposthitis;
- Follicular balanoposthitis;
- Gangrenous balanoposthitis;
- Allergic balanoposthitis;
- Anaerobic balanoposthitis.
Classification of balanoposthitis by origin of pathogens
- fungal balanoposthitis,
- bacterial balanoposthitis,
- traumatic balanoposthitis,
- balanoposthitis Zooba,
- microelement balanoposthitis (caused by residual urine entering the foreskin sac).
Classification of balanoposthitis according to the nature of the disease
- Acute form
- simple, characterized by discomfort in the glans penis and tissue thinning;
- erosive, in which painful erosions of a bright red color appear, pain occurs during sexual intercourse and urination, accompanied by phimosis;
- gangrenous - the most severe form, characterized by the appearance of purulent ulcers, pain and swelling.
- Chronic form
- indurative, in which the glans penis and foreskin shrink;
- ulcerative-hypertrophic, characterized by the appearance of non-healing painful ulcers.
Causes of balanoposthitis
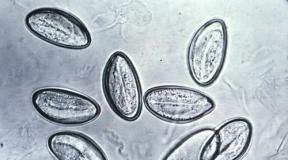
The occurrence of balanoposthitis is accompanied by a combination of two factors: the causative agent of the infection and the conditions for its development. The first role can be played by various bacteria, fungi and viruses:
- gardnerella,
- staphylococci,
- streptococci,
- yeasts, etc.
Most often, the disease develops due to insufficient compliance with the rules of personal hygiene, especially after sexual intercourse, oral-genital and anal-genital contacts. Predisposing factors may be:
- narrowing of the foreskin (phimosis),
- traumatic skin damage (abrasions, local irritation),
- sexually transmitted diseases (gonorrhea, trichomoniasis, chlamydia, syphilis),
- skin diseases (contact dermatitis, lichen planus, psoriasis, etc.),
- increased skin sensitivity and predisposition to allergic reactions,
- weakened immunity (after chemotherapy, HIV infection, etc.).
Balanoposthitis often occurs in patients with diabetes mellitus, as a consequence of impaired tissue trophism. Allergic and toxic forms of balanoposthitis are much less common.
Symptoms of balanoposthitis
With balanoposthitis, the affected areas of the glans penis and foreskin become red and swollen, which leads to an even greater narrowing of the opening in the foreskin, as a result of which the process of urination becomes difficult and becomes extremely painful. The main subjective symptoms of balanoposthitis are:
- discomfort,
- burning sensation in the area of the head of the penis,
- swelling of the skin,
- dyspareunia (painful sexual intercourse),
- sometimes the appearance of erosions and ulcers.
The clinical picture of the disease is characterized by hyperemia, swelling of the skin of the glans penis, the presence of discharge in the preputial sac, while urethral discharge is usually absent. The nature of the symptoms of balanoposthitis in each specific case depends on the type of damaging agent (infectious and non-infectious) and the presence of predisposing factors (diabetes mellitus, long foreskin, etc.).
Symptoms of simple balanoposthitis
Simple balanoposthitis is characterized by diffuse redness, swelling and maceration of the skin of the head and inner layer of the foreskin, followed by the formation of superficial isolated and confluent erosions of various sizes and shapes with purulent discharge, surrounded by scraps of macerated epithelium. Subjective mild burning and itching.
Symptoms of erosive balanoposthitis
Erosive balanoposthitis is characterized by the formation of white swollen areas of dead epithelium, and then large, sharply demarcated bright red painful erosions with a rim of maceration along the periphery. The process may be complicated by phimosis. Painful regional lymphangitis and inguinal lymphadenitis are often observed. After regression of simple and erosive balanoposthitis, no traces remain.
Symptoms of gangrenous balanoposthitis
Gangrenous balanoposthitis is accompanied by fever and general weakness. Deep painful purulent-necrotic ulcers of various sizes appear against the background of severe swelling and redness of the head and foreskin. As a rule, phimosis develops; Possible perforation of the foreskin. Ulcers heal slowly. In all cases of balanoposthitis, it is necessary to exclude syphilis (tests for Treponema pallidum, serological tests, confrontation).
Diagnosis of balanoposthitis
The diagnosis of “balanoposthitis” is made on the basis of urine analysis, general and biochemical blood tests for signs of a bacterial inflammatory process in the body. In addition, a bacteriological examination of the discharge from the urethra is carried out. Especially if this discharge is purulent in nature. In addition, testing for HIV and AIDS is mandatory.
Most often, the most modern and accurate method used for this is the polymerase chain reaction (PCR). In some cases, urethroscopy may be necessary. However, since this procedure is still invasive and extremely painful for the patient, they try to avoid it. Sometimes an ultrasound examination of the genitourinary tract is also prescribed. Most often for the purpose of differential diagnosis.
Treatment of balanoposthitis
Treatment of balanoposthitis is always prescribed based on the results of the examination, since they provide reliable information about the causes that caused them and the stage of the disease.
When diagnosed with balanoposthitis, treatment with tablets involves the use of antibacterial and antifungal agents. In cases where a metabolic or general hormonal disorder is detected, treatment is prescribed that eliminates this problem, since the reduced immunity as a result does not contribute to the effective elimination of balanoposthitis.
In case of balanoposthitis, treatment with ointment is attractive for patients due to the ease of its use. Most often, a urologist-andrologist prescribes prednisolone, decamin and xeroform ointments. In case of deep tissue damage, ointments must be supplemented with antibiotics. In advanced cases, it is strongly recommended to dissect the narrowed foreskin.
In cases where men do not treat balanoposthitis at home, not only the lymphatic vessels of the penis become inflamed, but also the inguinal lymph nodes, the disastrous result of which is gangrene of the genital organ and even death. Therefore, it is necessary to understand that even failure to comply with basic rules of personal hygiene can cause a disease, if not treated in a timely manner, a man will begin to experience severe pain in the genital organ itself.
Drugs for the treatment of balanoposthitis
You should not refuse to use various medications at home to treat balanoposthitis in men. The most popular is Clotrimazole, which can be purchased at the pharmacy in the form of an ointment, aerosol or solution. The drug contains an imidazole derivative, which is famous for its antifungal, antibacterial and anti-inflammatory effects. Apply a thin layer of Clotrimazole to the head of the penis and do not wipe off. Repeat the procedure 2 to 4 times a day for 10-14 days.
To enhance the effect and quickly recover, it is recommended to take Diflucam tablets orally three times a day, 1 pc. For preventive purposes, Levorin and Nystatin are used, which effectively fight fungal infections.
Ointments for the treatment of balanoposthitis
The most common ointment that contains an antibiotic is syntomycin ointment. Synthomycin liniment actively fights against many bacteria, including balanoposthitis microbes. Apply the ointment to the head of the penis so that it gets between all the folds of the foreskin. You can apply a bandage over it.
Treat before bed every day until complete recovery. Triderm ointment is a combined preparation with antifungal and antibacterial properties. Effectively reduces itching, inflammation on the head and pain. For treatment to be effective, it is enough to smear the penis twice a day and this will lead to healing of the skin.
Triderm ointment is a combined preparation with antifungal and antibacterial properties. Effectively reduces itching, inflammation on the head and pain. For treatment to be effective, it is enough to smear the penis twice a day and this will lead to healing of the skin.
Levomikol ointment is quite often popular in the treatment of balanoposthitis in men. It contains methyluracil, which stimulates the restoration of the skin, and an antibiotic. Apply the ointment to the genitals before going to bed and apply a bandage, leave it until the morning. After three days of intensive treatment, significant improvement will occur.
Treatment of balanoposthitis at home
Treatment of balanoposthitis is carried out mainly at home. The patient is prescribed drugs used as part of antibacterial and anti-inflammatory therapy. Balanoposthitis is rarely accompanied by intolerable pain, and therefore the prescription of analgesics is rarely used. It is advisable to use medications in combination with folk recipes- this can speed up the healing process, but consulting a doctor on this topic will not be superfluous.
Throughout the entire period of treatment or at its individual stages, the doctor may prescribe the patient a course of immunity-strengthening medications and vitamins, and will also recommend adherence to a gentle diet and the principles of a healthy lifestyle in general. During the period of treatment, the man is advised to abstain from sexual activity.
If the disease is detected late, hospitalization may be indicated in order to continuously monitor the patient's health. In a hospital setting, among other things, surgical intervention is performed, the indications for which are determined by the attending physician.
Treatment of balanoposthitis with traditional methods
The use of rinses and baths for the penis as part of therapy allows you to realize all the possibilities of traditional medicine - for preparing infusions, decoctions and compresses with bactericidal and anti-inflammatory properties.
Candidiasis balanoposthitis
The development of candidal balanoposthitis in men is provoked by a yeast-like fungus of the Candida family. Most often, this nature of the disease occurs in men with diabetes. Even with a course of antibacterial therapy, a positive result with the combination of candidal balanoposthitis and diabetes mellitus practically does not occur. As a rule, the simultaneous development of balanoposthitis and balanitis is observed.
In rare cases, candidal balanoposthitis develops against the background of congenital phimosis and in the presence of an elongated foreskin. When diagnosed with candidal balanoposthitis, treatment, in addition to taking specific medications, also involves following a diet, which consists of completely excluding sweet, hot, spicy and pickled foods from the diet. The consumption of alcohol in this case is strictly prohibited.
To achieve the greatest effect, doctors for the disease “candidal balanoposthitis” accompany treatment in men with a strong recommendation to abstain from sexual activity for this period. If this disease is caused by phimosis, specialists always perform a longitudinal dissection of the foreskin. After the pathological process subsides, the patient is circumcised. But in the absence of phimosis, they resort only to conservative methods of treatment (drugs Biseptol, chloramphenicol, erythromycin and others are prescribed). In severe forms, treatment is supplemented with intramuscular administration of broad-spectrum antibiotics.
Complications of balanoposthitis
In addition to phimosis, paraphimosis is the most common complication. Chronic balanoposthitis, accompanied by phimosis, can be complicated by the development of leukoplakia.
A long-term inflammatory process on the glans penis can lead to atrophy of the receptor apparatus and a decrease in the sensitivity of the glans penis. This causes inconvenience during sexual activity, reduces the pleasant sensations during sexual intercourse, reduces the feeling of orgasm, and ultimately can negatively affect potency and the quality of sexual life.
In addition, the inflammatory process from the head of the penis can move to the urethra, that is, lead to the development of urethritis.
Prevention of balanoposthitis
In most cases, the cause of balanoposthitis is infection as a result of sexual intercourse with a partner with disturbed vaginal microflora (vaginal dysbiosis). Most women suffer from this disorder to one degree or another, which is why periodic examination by a gynecologist is recommended. To avoid the development of balanoposthitis, men need to maintain hygiene and undergo regular examinations by a urologist.
Balanoposthitis in children
Balanoposthitis is a disease that affects exclusively male children, most often between the ages of 0 and 5 years. It is an inflammation of the glans penis and the inner side of the foreskin. The disease affects boys for many reasons, the most common of which are infectious.
Causes of balanoposthitis in children
The main reason for the occurrence of this disease is neglect of the rules of genital hygiene. Because of this, in boys, a special secretory fluid, smegma, accumulates right under the foreskin, which provides a good environment for the development and reproduction of pathogenic bacteria.
The development of the disease in young boys is also associated with age characteristics: up to 4-5 years, the head of the penis does not yet open on its own (physiological phimosis), so hygienic care can be difficult. On the other hand, when trying to open the head on your own, harmful microorganisms can enter the foreskin from the external environment. The most common pathogens of balanoposthitis are staphylococci, streptococci, Escherichia coli, herpes virus, Proteus, yeast fungi.
Symptoms of balanoposthitis in children
Malaise during illness does not appear immediately. But after a few days, the symptoms of balanoposthitis look like this:
- Decreased appetite
- Body temperature reaching 38 degrees
- Poor sleep, weakness and irritability
- Enlarged lymph nodes in the groin
- Development of daytime or nocturnal enuresis
Symptoms increase in intensity over 5-6 days - all these are manifestations of balanoposthitis in an acute form. Sometimes, when the foreskin is independently moved and the head of the penis is exposed, self-healing is possible if the accumulated smegma is carefully removed and everything is disinfected. But more often, in the absence of correct or timely treatment, acute balanoposthitis migrates to the chronic form, which is fraught with big problems for boys in the future. Therefore, it is much wiser to contact pediatric specialists - a surgeon or urologist.
Treatment of balanoposthitis in children
Rules and recommendations for the treatment of balanoposthitis in boys will differ depending on the cause that provoked inflammation of the glans and foreskin of the penis. If the disease is just a consequence of poor hygiene, then therapy comes down to daily washing of the penis with a weak furatsilin solution or a solution of potassium permanganate.
If an infection is suspected, a smear is taken from under the foreskin and examined for the presence of pathogenic bacteria, as well as their level of sensitivity to various drugs. Based on the information received and the diagnosis, certain drug therapy is prescribed.
Thus, not all antibiotics will affect pathogenic bacteria in balanoposthitis, and some even, on the contrary, promote the further vital activity of microorganisms. Therefore, antibiotics should be prescribed by a specialist and only after the root cause of the disease becomes known.
Local treatment of balanoposthitis in boys consists of treating the affected area with an antiseptic. You can also apply gauze compresses soaked in antiseptic on both sides of the child’s penis.
At night, it is recommended to use levomikol - this ointment with a powerful disinfecting effect is prescribed by many doctors. If balanoposthitis is caused by fungal diseases, then clotrimazole will be used. Medicinal ointments, as well as antibiotics, are prescribed only after microbiological examination.
Prevention of balanoposthitis in children
Basic effective method Prevention of balanoposthitis is compliance with the rules and norms of intimate hygiene. At the same time, when bathing a child, it is not necessary to use detergent every time when washing the head under the foreskin - just water is enough. The main thing is daily. Infant boys should also change diapers regularly, use baby creams and hypoallergenic powders. For older boys, choose comfortable underwear without seams in the front and made from natural materials.
Questions and answers on the topic "Balanoposthitis"
Question:Hello, I have fluid discharge from the penis, there is no pain, except discomfort when urinating. What could it be? The liquid is clear with a characteristic odor.
Answer: Hello! You need to get tested for sexually transmitted infections.
Question:Hello. The other day I’m going to the hospital with chronic balanoposthitis. I will be circumcised, but I have another problem - epididymitis orchioepididymitis on the left. I've had it treated before. Antibiotics, lidase, instillations, applied Vishnevsky ointment, warming up. It seemed to have gone away, but now it has appeared again. Now he is starting to move not only from the left, but also to the right. I wanted to ask you - if I tell the head of the department that I have another complaint - after circumcision, will they also treat me for epididymitis orchioepididymitis? So that I don’t have to run to the hospital again later. They should respond to my other complaint, right?
Answer: Hello! Of course, you need to inform your doctor about this. There you will decide with him whether he will treat your orchitis before circumcision (and whether he will undertake it) or after (if it is orchitis). But eggs are expensive, so take care of them.
Question:Hello. My son (7 years old) often has an inflamed penis after untreated balanoposthitis. When I go to doctors, I only receive recommendations on daily hygiene, but the fact of the matter is that missing a day of walking immediately leads to an inflammatory process (redness) and inflammation now occurs even with regular hygiene. General urine tests, according to Nechiporenko, ultrasound of the kidneys are normal. It was also suggested to do circumcision, but apparently I don’t understand something here: if the head opens well, then how can this help? Isn’t the problem with “aggressive” secretions that constantly provoke inflammation?
Answer: Show your child to a pediatric urologist, since there are many reasons for recurrent balanoposthitis (infection, synechiae of the foreskin, diabetes mellitus, etc.). If the inflammation cannot be dealt with, then it is better to have an operation and the cause will be eliminated.
Question:Hello! A 5-year-old boy has been experiencing yellowish discharge on his underwear towards the end of the day for 3 weeks. We made baths with chamomile and miramistin, but did not achieve a lasting result. Is it possible to use antibiotics without examination with tests? Friends recommend Ciprolet, but the contraindications scare me. Is it even possible to use any antibiotics in this case?
Answer: Hello. We never use antibiotics for balanoposthitis. It is always cured in children with local antiseptics.
Question:Hello! Is it possible to use Miramistin instead of the prescribed furatsilin when treating the foreskin with balanoposthitis. The child is 2 years old.
Answer: Hello, you can use Miramistin, but the main treatment is regular rinsing of the head, even with saline solution.
Question:A child aged 2 years and 9 months was diagnosed with purulent balanoposthitis. They opened the head and removed the pus. Afterwards they prescribed baths of chamomile and potassium permanganate 3-4 times and also told me to make a compress with chlorhydroxydine. Tell me, maybe I need to apply some other ointment so that everything goes away faster. The child is screaming because the compress is stuck to the head. And the foreskin is very swollen and red, the head cannot close. Is this normal or not?
Answer: It is impossible to accurately assess the situation without an examination; continue treatment as usual. After the procedure with the head, it should close completely. If the head is pinched by the foreskin and does not close, it is called paraphimosis, a very dangerous condition. Therefore, I recommend visiting your surgeon again. With it, resolve the issue of painkillers and antihistamines to reduce swelling (Nurofen syrup, Suprastin or Zodak). Take baths more often, and let him urinate in them, so that the urine does not irritate the wound.
Question:I probably already have chronic balanoposthitis, since I started having it about 7 years ago. It appears and then disappears. I am 51 years old, I have been suffering from a mild form of diabetes for 5 years, glycated hemoglobin is in the range of 6.5-6.8, I take metfarmines. Regarding the issue of balanoposthitis, I contacted a urologist I knew about five years ago. he advised: fluconazole, 150 mg once, baths with chlorhexidine, Triderm cream 1-2 times a day, 5-7 days, then for about 5 days a mixture of zinc-salicylic ointment and hydrocortisone 1% in a 1:1 ratio. As long as I'm flying, everything is fine. I noticed that it worsens in the spring and autumn, as well as after sexual intercourse (I am not married, sex is not frequent). It may all calm down for a while and not bother you, or redness may appear again, then after 2-3 days there will be swelling and a cheesy formation like smegma. It seems that only Triderm cream helps. While I’m walking, smeared with triderm, the head and everything adjacent to it are beautiful, pale in color, dry, i.e. not inflamed or swollen. Tell me, maybe I can be treated according to your advice? Yes, at one time they took a smear, there were candida, i.e. probably balanoposthitis of candidal etiology.
Answer: Hello. Candidiasis balanoposthitis is an indicator of immune status against the background of diabetes mellitus. You need to eliminate complications as much as possible. diabetes with an endocrinologist and immunologist. I do not recommend using Triderm topically for a long time; it contains a hormone that reduces immunity. To improve the local condition, try Viferon ointment for 1 month, hygiene 2 a day without the use of chemicals. Normal flora should live on the head. In case of exacerbation, Exoderil cream.
Balanoposthitis is an inflammatory disease of the skin of the penis. According to statistics, this pathology is diagnosed annually in 11% of men. With this disease, inflammation develops in the glans penis or on the inside of the foreskin.
Concept and types of disease balanoposthitis (photo)
Balanoposthitis is one of the common urological diseases. His treatment is carried out according to standard and proven regimens. To select the most effective one, the urologist determines the level of complexity of the pathology and the type of disease.
The term “balanoposthitis” combines two concepts:
- balanitis (inflammation of the glans penis);
- posthitis (inflammatory process of the inner layer of the foreskin).
Due to the fact that the inner part of the foreskin is in contact with the surface of the head, the developing inflammatory process always affects both parts of the genital organ. The development of balanitis and posthitis occurs simultaneously, so these pathologies are often combined into one name - balanoposthitis.
Balanoposthitis in men (photo) can develop only if they have a foreskin. If this element of the reproductive organ is already circumcised, pathology will not occur. The disease in question has several types of course, depending on the location and severity of the inflammatory process. A combination of several factors contributes to the spread of inflammation.
The disease is classified according to the foci of the inflammatory process, the level of severity of the lesion, and the type of pathogen. Depending on the type of pathogen, balanoposthitis occurs:
- anaerobic;
- allergic;
- circinar;
- chlamydial;
- candida;
- gangrenous;
- follicular.
This disease is also divided according to the origin of the pathogenic microorganisms that cause it. In this direction, the following types of balanoposthitis are distinguished:
- balanoposthitis Zooba;
- bacterial;
- traumatic;
- fungal;
- microelement.
There is another option for dividing balanoposthitis - by form.
The acute stage of the disease is characterized by pronounced symptoms and rapid progression. It happens:
- simple (accompanied by slight discomfort in the head of the penis and severe thinning of the skin of the external genitalia);
- erosive (the surface of the genital organ is covered with painful bright red ulcers, the processes of urination and sexual intercourse are accompanied by severe painful sensations, and phimosis of the penis often develops against the background of this form);
- gangrenous (the most severe variant of the acute form of balanoposthitis, characterized by the formation of ulcers and wounds with purulent contents, the appearance of severe swelling and inflammation).
The chronic stage of balanoposthitis is divided into ulcerative-hypertrophic and indurative. In the first case, the penis becomes covered with painful, long-term non-healing ulcers and wounds, and in the second, wrinkling of the foreskin and head of the genital organ is observed. Symptoms in the chronic form of balanoposthitis are mild, alternating periods of relapses and remissions occur.
Each type of balanoposthitis has its own characteristics and features. For example, the bacterial form of the disease occurs after pathogens enter directly onto the head of the genital organ. Interestingly, phimosis and balanoposthitis are described in ICD 10 as interrelated diseases of the male genital organs. If a patient with phimosis does not follow the rules of personal hygiene, a favorable environment for life and development of pathogenic microorganisms is formed in his external genitalia. They lead to the development of a strong inflammatory process - balanoposthitis. Bacterial balanoposthitis can be classified according to the type of pathogen. This pathology often develops due to gonorrhea or syphilis. The causative agent of the disease can be female Gardnerella bacteria if a man has unprotected sex with his partner. Another type of bacterial balanoposthitis is associated with anaerobic bacteria. The disease is diagnosed quite rarely, since the life activity of such bacteria occurs outside of an oxygen environment. Certain types of anaerobic pathogens of balanoposthitis even die when exposed to air. Anaerobes penetrate into a man's body after contact with the ground, with injuries to the genital organ or wearing too tight underwear.
One of the most severe forms of the disease is chronic purulent balanoposthitis. Simultaneously with inflammation of the inner layer of the prepuce and the head of the penis, a man develops purulent discharge from the urethral canal. The disease is provoked by streptococci, staphylococci and yeast fungi. Also, purulent balanoposthitis occurs in patients with diabetes mellitus, against the background of allergic reactions or purulent urethritis. If staphylococcal balanoposthitis develops, from the reviews of men about it, one can understand that the disease is accompanied by a rash, severe itching and swelling of the penis. Sometimes the inflammatory process affects other organs of the genitourinary system. If antibacterial therapy is not started in a timely manner, purulent balanoposthitis turns into an erosive form, with the formation of wounds and ulcers on the genital organ.
Recurrent balanoposthitis is one of the most discussed topics on medical forums. The disease belongs to the common forms of chronic balanoposthitis. Most often it develops as a result of an advanced infectious-inflammatory process. Relapses of balanoposthitis are provoked by infectious pathogens, sexually transmitted diseases, and can also occur due to non-compliance with the rules of intimate hygiene. Relapses of the pathology are accompanied by painful symptoms, aggravated by the prolonged course of the inflammatory process.
Balanitis and balanoposthitis: ICD code
Balanoposthitis and balanitis have the same code in the International Classification of Diseases, 10th revision (ICD-10). These pathologies are assigned parameter N48.1. True, to identify the infectious agent, an additional code B95-B98 is used. Balanitis also has an individual code (together with plastic hardening of the penis and Peyronie's disease) - N48.6. The international classification helps urologists accurately and quickly diagnose balanoposthitis in boys (photo) and adult men, prescribe effective treatment for the disease, taking into account the severity of symptoms and the presence of complications. In addition, by referring to this classification, you can understand what balanoposthitis looks like in a child (photo), teenager or adult male patient.
Balanoposthitis: how long does the disease last?
The duration of balanoposthitis depends on many factors. The cause of the disease, the stage of development of the pathology, and the individual response of the patient’s body to the selected set of antibacterial drugs are important.
If balanoposthitis is triggered by the accumulation of secretory lubricant under the foreskin and the development of pathological bacilli in it, it can be cured in just 5-7 days, simply by adhering to the rules of intimate hygiene. Erosive forms of balanoposthitis take longer to treat. The addition of a bacterial infection to the underlying disease extends the course of therapy to 1 or 2 weeks. Treatment of balanoposthitis caused by phimosis is most often eliminated surgically. In this situation, recovery time extends to 2-3 weeks. Balanitis, which develops against the background of underlying diseases (diabetes mellitus, purulent urethritis, allergies), is cured only after they are eliminated. The causes of balanoposthitis help doctors quickly diagnose the disease and prescribe a course of effective therapy.
Causes
One of the main tasks of a urologist when diagnosing balanoposthitis in a patient is to determine the factors that provoked the disease. In order to quickly and effectively get rid of balanoposthitis, the causes and treatment of the disease should be determined with the help of a qualified andrologist in a hospital setting.
The main causes of balanoposthitis
Regardless of what form balanoposthitis takes, doctors associate the causes of the disease with the following unfavorable factors:
- dermatological problems (psoriasis, dermatitis, lichen);
- reduced immunity (most often the problem occurs after concomitant diseases, HIV infection or after undergoing treatment procedures);
- increased skin sensitivity, its tendency to allergic reactions;
- congenital phimosis (anatomical feature of the foreskin of the penis associated with its narrowing) is the most common cause of erosive balanoposthitis in boys;
- sexually transmitted diseases and accompanied by suppuration (purulent masses irritate the external genitalia and provoke the development of balanoposthitis);
- injury to the skin on the penis (scratches, abrasions, cracks);
- lack of proper and daily genital hygiene, leading to the formation of a favorable environment for the proliferation of pathogenic bacteria;
- diabetes mellitus, which interferes with the supply of nutrients to tissues;
- frequent washing of the genitals with soap, which irritates the skin;
- unprotected sexual intercourse with partners who have too dry microflora in the vagina (infection from there will definitely get to the head of the penis);
- bad heredity;
- autoimmune diseases;
- hormonal imbalances;
- exposure to various bacteria (for example, streptococci, staphylococci, E. coli).
Balanoposthitis in men, causes, symptoms and treatment of the disease are often associated with general diseases that weaken the natural resistance of the skin of the genital organs to the effects of foreign bacteria and pathological microorganisms. Inflammatory processes characteristic of balanoposthitis can develop against the background of hypovitaminosis, diabetes mellitus, allergies or anemia. Local factors also contribute to the activation of the disease:
- improper fulfillment of intimate hygiene requirements;
- penile injuries;
- foreskin too narrow.
There are other reasons for the development of balanoposthitis that are characteristic only of a certain age.
Balanoposthitis: causes in men
Balanoposthitis in adult men often develops due to insufficient or excessive hygiene of the external genital organs. If you clean out smegma from under the foreskin too thoroughly or, conversely, do not perform hygiene procedures at all, this leads to balanoposthitis in adult men and balanitis in minor boys. The foreskin can become inflamed due to mechanical or chemical stress (for example, if a man uses irritating disinfectants while washing or bathing). An allergic reaction of the body to medications, latex materials (condoms are made from them), cosmetic compositions and perfumes can sometimes trigger the development of balanoposthitis.
For balanoposthitis in men, treatment and the causes of the pathology are interconnected. Factors that provoke the disease can be infectious, and in this case they are eliminated using broad- or narrow-spectrum antibacterial drugs. For example, if candidal balanoposthitis develops in men, the causes of the disease are associated with yeast-like fungi of the genus Candida Albicans. They are transmitted mainly through unprotected sexual contact. Candida exclusively affects men with uncircumcised foreskins.
The occurrence of chronic balanoposthitis in adult men is provoked by sexually transmitted diseases. For example, this type of pathology is diagnosed when infected with the human papillomavirus. However, the main factor in the formation of balanoposthitis remains poor intimate hygiene. Sometimes a man cannot clean the cavity under the foreskin due to phimosis (when the skin does not move well or stops moving at all). Thus, this pathology favors the occurrence of balanoposthitis and balanitis. Trimming the fold of skin that forms the prepuce helps eliminate the risk of inflammation.
Balanoposthitis in a child: causes
In childhood, balanoposthitis develops as a result of “clogging” of the preputial cavity with urine, exfoliated epithelial cells and secretory fluid (smegma). Various reasons contribute to the formation of inflammation:
- deposited urine salts;
- various constrictions;
- poor hygiene of the child’s genital organs.
Smegma becomes an ideal environment for the life of pathological bacteria, fungi and microorganisms. Unfavorable processes in the preputial cavity lead to inflammation, against which balanoposthitis develops. There are other negative factors that lead to the occurrence of balanoposthitis in a child:
- obesity;
- endocrine diseases;
- vitamin deficiency;
- hypothermia;
- permanent injuries to the penis associated with constant wearing of tight underwear.
Childhood and adult balanoposthitis is dangerous due to its complications. The disease can become chronic, and the inflammatory process affects neighboring internal organs.
Balanoposthitis - chronicity of the process and causes
Diagnosis of chronic balanoposthitis in men, the causes of the disease and treatment are the responsibility of a urologist. The main causes of chronic disease are associated with the following factors:
- permanent mechanical injuries to the foreskin from allergic and chemical substances;
- hard sex, systematic masturbation;
- wearing underwear that is too tight and made from synthetic materials;
- use of low-quality cosmetics for intimate hygiene;
- infectious pathologies that practically cannot be treated with antibacterial drugs (the problem is often associated with improper treatment of acute balanoposthitis, due to which pathogenic microflora develops resistance to pathogenic bacteria);
- systematic infection of the male genitourinary system, provoked by pathogens of sexually transmitted diseases, unprotected sexual intercourse, promiscuity, anal and oral sex, attempts to independently expose the head of the penis during phimosis (these factors initially lead to the development of acute balanoposthitis, which subsequently acquires chronic forms);
- diabetes mellitus, herpes, HPV, Reiter's syndrome, psoriasis.
The causes of acute or chronic balanoposthitis are also determined by the complex of symptoms that accompany this disease.
Symptoms
If a man develops balanoposthitis, the signs (photos) are varied. They depend on the causes and forms of the disease. Sometimes the patient complains of severe pain in the genitals in the absence of external manifestations of the disease. The opposite situations also happen. The appearance of the genital organ changes greatly, but no pain or discomfort occurs. The patient's age also affects the complex of signs of this disease.
Balanoposthitis: symptoms (photos)
In medical practice, the following symptoms of balanoposthitis are distinguished.
Pain. Pain is a common but not obligatory sign of balanoposthitis. Unpleasant sensations usually occur at the site of localization of skin lesions (ulcers, erosions, allergic rashes). Exacerbation of pain occurs if the penis is touched with hands or during sex. If the inflammatory process affects the urethra, pain also manifests itself at the time of urination. The nature of pain with balanoposthitis in men is different. Most patients complain of itching, burning, stabbing and cutting sensations. In advanced cases, a man cannot make love due to severe discomfort. There are cases when pain in the head and foreskin of the penis occurs without external manifestations. This indicates hypersensitivity of some areas of the genital organ. Probably, the inflammatory process affected the blood vessels and nerves that penetrate the foreskin and the head of the genital organ.
Swelling. The appearance of swelling on the genital organ during balanoposthitis indicates poor drainage of lymph and blood from the affected areas. Severe disease, tissue necrosis and the development of gangrene are often accompanied by this particular symptom. When edema appears, it is important to differentiate balanoposthitis from other diseases with similar clinical course(for example, atypical angioedema or filariasis).
Redness of the skin. Local dilation of blood vessels during balanoposthitis leads to severe redness of the skin on the genitals. The skin reacts in this way to small defects and damage, into which pathogenic microorganisms enter. Increased blood flow in the vessels helps to neutralize them faster. The reddened glans and foreskin on the penis in men with balanoposthitis is the most characteristic symptom of the pathology in question. Regardless of the form of balanoposthitis, this symptom appears one of the first.
Allergic skin lesions, rash. External damage to the skin, the appearance of rashes, ulcers, erosions, changes in the color of the skin are symptoms indicating the development of an inflammatory process characteristic of balanoposthitis. Sometimes the skin on the penis becomes rough and thick due to numerous erosive lesions. The form and severity of the disease are the determining factor for determining the type of skin lesion.
Itching. A common sign of balanoposthitis, preceding pain and burning. The appearance of itching is caused by allergies or poor genital hygiene. The symptom does not always appear.
Difficulty urinating. If inflammation from the head of the penis spreads to the urethral canal and the urethra itself, the patient has problems emptying the bladder. The lumen in the urethra narrows due to the inflammatory process, and the focus of inflammation can form in the bladder, kidneys or prostate. This symptom practically does not appear in mild forms of balanoposthitis. If from the first days of the development of the pathology a patient complains of difficulty urinating, the infection probably got under the foreskin from the internal organs ( bladder, kidneys).
Enlarged lymph nodes. Lymphatic fluid from the penis always flows to the inguinal lymph nodes. Along with it, part of the metabolic products enters there. When inflammation develops in the genitourinary system, pathogenic bacilli, toxins, and pus enter the lymph. Pathological components enter the lymph nodes, accumulate there and lead to moderate inflammation. An unfavorable process provokes enlargement of the lymph nodes 2-3 days after the onset of inflammation. They may be painful when palpated.
The appearance of discharge from the urethral canal. Discharge from the outlet of the urethral canal during balanoposthitis most often signals the transition of the inflammatory process to the mucous membranes of the urethra. This is facilitated by bacterial pathogens. If the lower parts of the urethral canal are affected, uncontrolled discharge of secretions occurs. If the urine contains impurities of pus and blood, it is likely that the inflammatory focus caused by balanoposthitis is located in the bladder or kidneys. In general, with balanoposthitis, discharge from the urethra rarely appears. Sometimes pathological fluids accumulate on the surface of the foreskin or glans, forming plaque. It becomes a favorable environment for the life and development of pathological microorganisms, so these secretions should not be allowed to dry out. It is recommended to wash off such plaque immediately to prevent the condition from worsening.
False urge to urinate. This symptom occurs rarely with balanoposthitis. It is associated with irritation of the mucous membranes of the urethra and often accompanies kidney pathologies and cystitis.
Erectile dysfunction. The appearance of a sudden erection when a man is in a calm state is a characteristic sign of balanoposthitis. The failure occurs due to reflex excitation that occurs at the slightest irritation of the head or foreskin. These areas become very sensitive when balanoposthitis develops. The factors that provoke an erection with this disease are minor pain and itching. If there is damage to the skin of the penis (erosions, ulcers, wounds, cracks), the erection becomes painful. There is also the opposite situation, when there is no sexual arousal against the background of inflammation. This phenomenon is caused by the fact that pathogenic bacilli penetrate the bladder or prostate. Sometimes absence sexual arousal associated with severe roughening of the skin of the penis.
Deformations of the penis. Severe balanoposthitis can lead to changes in the shape of the penis. This usually happens with severe purulent tissue lesions, ulcerative-hypertrophic and gangrenous forms of the disease. All of these situations are characterized by extensive tissue damage. At the site of the resulting skin defects of the prepuce and head, scar tissue and adhesions subsequently form. Actually, because of them, the shape of the penis changes during erection, and sometimes even in a calm state. Surgery (penis plastic surgery) helps correct the situation.
If a doctor suspects a man has balanoposthitis, treatment and symptoms (photos) of the pathology are determined by him based on examination and laboratory test results. The fight against the disease is carried out using medication and surgical techniques.
Signs of balanoposthitis in men (photos)
Clinical manifestations of balanoposthitis in adult men depend on the type of disease and the causes of its occurrence. For example, ordinary catarrhal balanoposthitis in a male patient is accompanied by the following symptoms:
- pain in the head of the penis;
- swelling and redness of the foreskin;
- accumulation of pus in the preputial cavity (between the foreskin and the head of the genital organ);
- acute urinary retention, development of phimosis (these signs manifest themselves if there is no timely treatment for balanoposthitis).
Urogenital candidiasis provokes the development of candidal balanoposthitis in men, the symptoms and treatment of which are determined during a consultation with a urologist. The causative agent of the disease is Candida fungus, which is mistakenly considered to be the causative agent of exclusively female candidiasis.
For candidal balanoposthitis in men, the symptoms (photo) are as follows:
- the inner leaf of the prepuce and the head of the penis become purplish-red and swell;
- in some cases, the surface of the head of the penis becomes spotted;
- the head of the reproductive organ becomes covered with cheesy discharge, which appears as a result of the active activity of fungi (the discharge provokes itching and burning, and emits an unpleasant aroma);
- If there is no timely treatment for balanoposthitis, red spots on the head will transform into erosions or ulcers.
With the development of chronic balanoposthitis in men, special attention should be paid to symptoms and treatment. The disease occurs against the background of diabetes mellitus, due to the entry into the body of pathogens of sexually transmitted diseases or the herpes virus. Treatment for chronic balanoposthitis begins after the underlying disease has been eliminated.
The danger of chronic balanoposthitis lies in the fact that the inflammatory process passes from the foreskin to the internal organs of the genitourinary system, leading to the occurrence of pyelonephritis, prostatitis, and urethritis. If the pathogen enters the seminiferous tubules, the epididymis becomes infected. As a result, serious complications arise, the functioning of the male reproductive system is disrupted, and infertility develops. Chronic balanoposthitis can be recognized by the following signs:
- the head of the penis turns red, becomes dry and painful;
- the general symptoms of the disease almost do not appear, so the man for a long time does not suspect the presence of a dangerous pathology in the body.
- mild painful sensations in the foreskin and head of the penis, which become stronger over time;
- redness of the skin of the head of the penis, pronounced itching and slight swelling.
Untimely treatment of acute balanoposthitis leads to the transition of the disease to the chronic phase.
The symptoms of recurrent balanoposthitis in adult men are similar to those that occur in the acute form of the pathology. However, the severity of clinical signs is less, the disease periodically recedes and worsens, and there is a high risk of complications.
The development of purulent balanoposthitis in acute form is accompanied by the following symptoms:
- the appearance of deep purulent-necrotic foci on the head of the penis and the inner layer of the prepuce;
- severe swelling of the head, its color is bright red (a symptom of active inflammation).
Ulcerative balanoposthitis is a consequence of untimely treatment of milder forms of the disease. Its signs are:
- the head of the penis is inflamed and covered with numerous small ulcerations;
- the man experiences discomfort when walking, complains of painful urination and the inability to have sexual intercourse due to severe pain;
- the lymph nodes in the groin become inflamed due to the penetration of pathological microorganisms into them.
Traumatic balanoposthitis is a consequence of prolonged wearing of tight underwear and is characterized by the following symptoms:
- swelling and redness of the head of the penis (the pathological process can be local or complete);
- deformation of the penis shaft in areas with less sensitive skin.
Varieties of balanoposthitis include Zoon's balanitis and Queyra's erythroplasia. In the first case, the treatment prognosis is favorable, in the second, rapid radical measures (surgical intervention) are required, since Queyra's erythroplasia is malignant and in severe cases poses a danger to the patient's life. Both pathologies can be recognized by the following symptoms:
- the skin on the head of the penis atrophies, becomes covered with pink plaques (they are located separately and do not merge with each other);
- ulcers, erosions and vegetations appear on the head of the penis if the disease is too advanced;
- the patient complains only about the changed appearance of the penis, there are no other symptoms of the pathological condition (no pain or discomfort, urination is not impaired).
Allergic balanoposthitis develops after contact of the head of the penis or foreskin with allergic substances (latex, contraceptives, chemical personal care products, which contain a lot of dyes and flavors). Signs of the allergic form of balanoposthitis:
- rash;
- small blisters, erosive lesions of the skin of the penis;
- swelling of the foreskin and glans.
Adhesive balanoposthitis often develops in children, against the background of physiological phimosis. The disease is accompanied by swelling, redness and soreness of the tissues.
Men suffering from alcoholism or diabetes are more likely to experience nonspecific balanoposthitis. Its symptoms:
- initially the head of the penis becomes slightly inflamed, subsequently the unfavorable process is activated and provokes the development of phimosis;
- purulent discharge appears from the preputial sac.
Signs of gangrenous balanoposthitis:
- the skin of the penis is covered with multiple suppurating and inflamed lesions;
- general health deteriorates greatly;
- inguinal lymph nodes enlarge;
- body temperature rises to high levels;
- bleeding from the penis (early stage of gangrene);
- deformation or change in the shape of the penis due to the growth of connective scar tissue;
- death of the head of the reproductive organ (the most severe consequence of gangrenous balanoposthitis).
Diagnosis of one or another type of balanoposthitis based on existing symptoms is carried out in the urologist’s office. The specialist prescribes a series of tests for the man (to clarify the presence of an inflammatory process, differentiate the disease, exclude the possibility of inflammation spreading to the internal organs of the genitourinary system), conducts an external examination, talks with the patient and, based on the data obtained, draws up a clinical picture of the pathology.
Balanoposthitis in a child: symptoms and treatment according to Komarovsky
According to Dr. Komarovsky, with balanoposthitis in a child (photo), symptoms and treatment depend on how advanced the pathology is. In childhood, balanoposthitis affects the penis if hygiene rules are not followed. Signs of illness:
- burning and itching in the groin;
- heat;
- redness and swelling of the penis;
- enlarged inguinal lymph nodes;
- erosions on the skin, desquamation of the dermis.
Symptoms may vary depending on the type of disease. If the Disease becomes chronic, its symptoms are mild.
Chronic balanoposthitis
Chronic balanoposthitis is discussed by patients quite often on forums. What kind of disease is this, why does it occur, what is the incubation period for chronic balanoposthitis and how to properly treat the pathology? This will be discussed further.
How long does it take for balanoposthitis to become chronic?
The transition of balanoposthitis to the chronic phase does not have a strict time frame. The incubation period for this disease depends on the type of pathology, as well as the individual characteristics of the male body. For example, erosive chronic balanoposthitis (photo) develops on the 3rd -5th day of an acute condition. Chronication of candidal balanoposthitis occurs after a week. Sometimes the incubation period of chronic balanoposthitis extends to 2 weeks or even several months.
Chronic balanoposthitis in men: treatment
To effectively and permanently eliminate chronic balanoposthitis, treatment of this disease must be long-term and comprehensive. The course of therapy involves the use of a set of measures:
- medications, antibiotics, hormonal ointments;
- surgical intervention;
- traditional medicines;
- diet.
A qualified urologist will be able to answer the question “how to treat chronic balanoposthitis in men (photo) and what medications to use for this” after examining a patient with pathology. The choice of medicines is made depending on the causes of the disease, its nature and degree. Basically, therapy for chronic forms of balanoposthitis is carried out with tablets (containing antibiotics) and ointments. The most common drugs used in the fight against the chronic form of the disease are:
- anti-inflammatory ointments (Elidel, Lokoid);
- ointments with an antifungal effect (Miconazole, Clotrimazole);
- Levomekol ointment;
- Locacorten ointment;
- Acyclovir tablets (they are prescribed to patients with genital herpes);
- Fluconazole tablets (prescribed for urethral candidiasis);
- medications containing penicillin (help with the gonorrheal form of balanoposthitis);
- Metronidazole tablets (help cure chronic balanoposthitis caused by Trichomonas);
- Broad-spectrum antibiotics are prescribed for the treatment of chronic balanoposthitis, provoked by other pathogens or having an unclear etiology (Ceftriaxone, Azithromycin).
The treatment regimen for chronic balanoposthitis is developed by the attending physician individually for each patient.
Surgical manipulations in the treatment of chronic balanoposthitis are used if conservative therapy does not produce the desired effect. To remove the source of inflammation, the surgeon completely or partially trims the foreskin. The method allows you to achieve a complete cure.
As for home treatment of chronic balanoposthitis, it is carried out to reduce pain and eliminate acute symptoms. Traditional therapy is temporary in nature and is used during exacerbations of the disease and the presence of unfavorable factors that can provoke a relapse of chronic balanoposthitis, which is in remission. Tinctures and baths, based on antiseptic compositions made from St. John's wort, plantain leaves or chamomile, help relieve severe pain. Inflamed areas of the genital organ are washed with such tinctures several times a day. You can make healing compresses from them by moistening the bandage in a healing decoction and applying it to the affected areas of the penis.
Men diagnosed with chronic balanoposthitis should reconsider their diet and give preference to proper nutrition. The menu must include:
- cereals;
- beef, chicken, veal meat;
- abundance of greenery;
- low-fat fermented milk products;
- legumes (soybeans, beans);
- vegetables (beets, tomatoes, sauerkraut, cucumbers);
- bran bread;
- fruits and berries in large quantities (currants, blueberries, cranberries);
- green tea, freshly squeezed juices.
Dietary nutrition for chronic balanoposthitis helps restore the defenses of a weakened body and accelerate the processes of regeneration and healing of damaged tissues.
Chronic balanoposthitis in a child and features of its treatment
Chronic balanoposthitis in children is practically not amenable to conservative treatment. Urologists immediately recommend surgery to circumcise pathological areas of the foreskin. Surgical intervention is performed during the period of remission of the disease, when inflammation subsides. After it, the risks of relapse of chronic balanoposthitis are eliminated, as well as the likelihood of developing phimosis and paraphimosis. For this problem, circumcision of the foreskin is performed even on infant boys. Chronic balanoposthitis can develop from acute and candidiasis forms.
Candidiasis balanoposthitis

Candidal balanoposthitis is an inflammatory disease that disrupts the activity of the male genitourinary system. The causative agent of the disease is a fungus of the genus Candida. The fungal infection penetrates under the human skin and into the mucous membranes, forming multiple filamentous forms there. The disease is diagnosed in men of different ages. Males can pick up the causative agent of candidiasis balanoposthitis during unprotected sexual intercourse with a partner suffering from candidiasis vulvovaginitis (thrush). One of the questions about candidal balanoposthitis on the forums is related to the peculiarities of the treatment of this disease. Therapy for balanoposthitis caused by Candida fungi is carried out in accordance with its form (pathology can be acute or chronic).
Acute candidiasis balanoposthitis: photo and treatment
When the first symptoms of acute candidal balanoposthitis appear, a man should consult a urologist and undergo a series of tests. Their results will help the specialist confirm the nature of the disease, exclude or confirm the presence of pathogens of sexually transmitted diseases in the body. The main cause of candidal balanoposthitis may be associated with phimosis (narrowing of the foreskin). In this situation, doctors recommend the only effective method - circumcision surgery (circumcision of pathological areas of the foreskin). Therapy in the postoperative period is based on the use of restorative and antifungal therapy.
For acute candidal balanoposthitis in men (photo), treatment is based on the following procedures:
- taking antifungal medications in the form of capsules, tablets, creams or ointments;
- the use of antimicrobial, immunostimulating medications, as well as vitamins;
- baths with the addition of a small amount of potassium permanganate, dioxidin and furatsilin (the water should be warm, the duration of the healing procedure is 5-7 minutes);
- the use of medicinal ointments, which are recommended to be applied in a thin layer to the head and foreskin of the penis (Lamisil, Clotrimazole);
- powders made from crushed tablets of streptocide, xenoform, dermatol help dry wounds in areas of active inflammatory process;
- medications for oral use (Fluconazole, which has extensive antifungal effects, has proven itself well in the treatment of candidiasis balanoposthitis);
- vitamins must be present in the complex of therapeutic measures, since they strengthen the immune system well and accelerate the healing process (a man with candidiasis balanoposthitis especially needs amino acids, magnesium, zinc, potassium, vitamins A, B, C, E);
- immunomodulators in capsules and tablets normalize microflora and help restore the vitality of a weakened body.
Traditional medicines help to cope with the painful symptoms that occur during acute candidiasis balanoposthitis. In the fight against male thrush, it is recommended to use decoctions based on chamomile, calendula, cloves and barberry. Infusions are prepared from the same components and added to the bath before bathing. Decoctions based on medicinal herbs are suitable for treating affected areas of the skin of the penis before applying antifungal ointment.
For treatment of acute candidiasis balanoposthitis to be effective, the patient must carefully monitor intimate hygiene, wash with warm water and soap twice a day, thoroughly dry the penis after bathing, and change underwear every day. It is advisable to exclude from the diet foods that promote the proliferation of fungal bacteria. These include baked goods, sweets, carbonated drinks, smoked products, and alcohol. It is better to replace the listed components with fresh vegetables and fruits. Remember that the main condition for a quick and successful fight against candidal balanoposthitis is a timely visit to the doctor.
Candidal balanoposthitis: treatment at home
Therapy for candidal balanoposthitis at home is aimed primarily at relieving pain, inflammation and swelling. For this purpose, traditional medicine is used, which you can prepare yourself. The main advantage of such medicines is that they contain natural ingredients. They provide exceptional benefits to a weakened body. Treatment of candidal balanoposthitis at home is carried out using the following types of plants.
- Calendula. To prepare the medicine, you need to take dried calendula flowers (1 tbsp), pour them with 1 glass of refined sunflower or olive oil. The container with this composition is tightly closed with a lid and infused in a warm place for 2 weeks. Then the medicine is filtered and the affected areas of the penis are treated with it 2-3 times a day.
- Plantain. Fresh plantain leaves help well in the treatment of candidiasis balanoposthitis. One leaf of the plant is crushed a little so that the juice comes out. Then it is applied to the affected areas of the reproductive organ and secured with a bandage. The compress of plantain leaves is held for 30 minutes, then it is removed. It is recommended to repeat this procedure 4 times a day.
- St. John's wort. From this medicinal plant prepare a healing solution for baths. Dried St. John's wort leaves in the amount of 1 tbsp. pour a glass of boiling water, leave for half an hour, filter and add to the bath before bathing.
- Oak bark. Young oak bark is carefully ground to a powder. The prepared product is taken in the amount of 1 tablespoon, poured with a glass of boiling water and infused over low heat for about 20 minutes. Then the oak bark infusion is removed from the heat and left in the same container for another 10 minutes. Then the product is filtered, added to medicinal baths and used to wash the penis affected by candidiasis balanoposthitis.
Before using any folk remedy at home, a man must obtain permission to unconventional treatment from the attending urologist.
Chronic candidal balanoposthitis in men: treatment
To cure chronic candidal balanoposthitis in men (photo), doctors use general antibacterial drugs. The disease, which has become chronic, alternates with periods of attenuation and exacerbation of symptoms, and has a sluggish nature. Sometimes, at the time of relapse, one capsule or tablet is enough for the patient to destroy the source of infection. Subsequently, the course of therapy is prescribed and adjusted by the attending physician (if necessary). For the purpose of prevention, medications against candidiasis balanoposthitis can be used for 1 month or more. If chronic candidal balanoposthitis is not treated, the patient will develop ulcers on the genitals, and the head of the penis will shrink. According to statistics, this type of disease is most often diagnosed in men infected with pathogens of sexually transmitted pathologies.
Candidiasis balanoposthitis and ointments suitable for its treatment
The question “what to do if candidal balanoposthitis does not go away and how to treat this pathology” is relevant for men faced with the problem of candidiasis. A common way to combat pathology is the use of ointments. Local therapy continues for 7-14 days (depending on the severity of the disease). Doctors recommend paying attention to the recommendations for applying the medicinal composition.
Before applying the ointment, the genitals should be washed.
The antibacterial agent is applied to dry and clean skin.
The most popular drug in the fight against candidal balanoposthitis is Clotrimazole. It is applied to the head of the penis and foreskin. Local treatment of the disease in question can be carried out with other drugs. Among them:
- Ketoconazole;
- Pifamucin;
- Miconazole;
- Econazole
Sometimes Candida yeasts develop resistance to antifungal ointments. In this situation, it is recommended to replace them with methylene blue dye after completing a course of treatment for a period of 7-14 days. The main side effect of using the product is associated with the skin turning blue. Over time, the paint wears off, but until then a man can wear dark-colored underwear so that nothing is visible.
Triderm (complex drug) gives a good therapeutic effect for candidiasis balanoposthitis. It helps relieve itching, allergies, inflammation, and effectively fights pathogenic microflora. Suitable for the treatment of early stages and advanced forms of the disease. Triderm ointment is applied in a small amount to the inflamed areas of the penis and gently rubbed into the skin. Improper use of the drug leads to burning, itching, irritation, and excessive dryness of the skin.
Candidiasis balanoposthitis is one of the forms of acute balanoposthitis
Acute balanoposthitis
Acute balanoposthitis is the most well-known and common form of pathology. The duration of the disease is 1-2 weeks. This period of time is enough for complete recovery.
Acute balanoposthitis - photo and characteristics of the disease
The acute form of balanoposthitis develops due to certain provoking reasons. Often the pathology under consideration is preceded by microtraumas, sexually transmitted diseases, and allergic reactions to intimate hygiene products. The disease can occur due to pathogens entering the body or severe irritation of the skin on the penis.
The symptoms of acute balanoposthitis are pronounced. Men experience pain in the head of the penis, and the skin on the genitals turns red. At this stage of the development of the disease, it is important to consult a doctor and begin a course of therapy to prevent the development of complications. If acute balanoposthitis is not treated, literally after a few days it becomes purulent or ulcerative. This further complicates the therapeutic process. You cannot self-medicate the acute form of balanoposthitis and ignore its symptoms for a long time. This will lead to chronicity of the pathological process.
Acute balanoposthitis has several forms and in some cases can disappear on its own, without any treatment. This happens, for example, with catarrhal inflammation, when microbes multiply slowly, and the structure of healthy tissues is not disturbed. But you should still consult a doctor to prevent the unfavorable course of the disease.
Acute balanoposthitis in ICD-10
The International Classification of Diseases considers acute balanoposthitis as a separate disease belonging to the class of diseases of the genitourinary system and the subsection “diseases of the male genital organs”. If a man is diagnosed with acute balanoposthitis, his ICD 10 code is N48.1. This parameter is assigned to all types and forms of the disease.
Acute balanoposthitis in men and its types
Acute balanoposthitis occurs most often in adult men and lasts about 1-2 weeks. Treatment of the pathology must begin on time, otherwise the inflammatory process will become chronic and drag on for several months, or even years. Balanoposthitis can take the following forms:
- herpetic;
- candida;
- chlamydial;
- erosive;
- anaerobic;
- purulent;
- circinar;
- gangrenous;
- ulcerative-pustular.
Differential diagnosis of the disease usually does not cause any difficulties. A man should consult a doctor when the first symptoms of pathology appear. The specialist will conduct a thorough examination, prescribe a set of tests and, based on their results, confirm or exclude the diagnosis, and will also be able to prescribe the correct treatment. The symptoms of balanoposthitis are a little similar to syphilis. Taking this factor into account, the urologist issues a referral for RW analysis. The need for laboratory tests is due to the fact that the doctor needs to identify the causative agent of the infection that provoked balanoposthitis. For the purpose of research, a smear is taken from the mucous membrane of the urethra. General blood and urine tests, as well as a blood sugar test, help to exclude or confirm the presence of diabetes mellitus in a patient (this chronic endocrine disease often causes inflammation of the genital organ in men).
Acute balanoposthitis: treatment in men and its features
Treatment of acute balanoposthitis depends on its form, stage, and the body’s resistance to certain medications. Hospitalization in a hospital for this disease is not carried out. The man is undergoing therapy at home, according to a regimen drawn up by his attending physician. Treatment involves the use of antifungal medications (Fluconazole). At home, the affected areas of the genital organ are treated with an antibacterial solution of chlorhexidine. Diet is also required. The patient needs to avoid sweet, salty, peppery and pickled foods for the entire period of therapy. If a man is diagnosed with candidal balanoposthitis, it is better to avoid sexual contact during therapy, or use a condom for protection.
Acute balanoposthitis in boys - Komarovsky reveals the features of the disease
The famous Ukrainian pediatrician Evgeniy Komarovsky associates acute balanoposthitis in a child with the entry of pathogens into the body (staphylococci, streptococci, yeast, E. coli or herpes virus). This occurs due to poor hygiene and insufficient care of the external genitalia. In addition, acute balanoposthitis in boys (photo), according to Komarovsky, develops due to the influence of external unfavorable factors:
- wearing tight underwear;
- excessive genital hygiene using irritating chemicals;
- unauthorized retraction of the foreskin in infant boys;
- the child wearing diapers of the wrong size;
- obesity;
- avitaminosis;
- hypothermia;
- diabetes;
- allergic reaction to washing powder.
The emerging pathology provokes the emergence of questions that become relevant for parents. For example, Dr. Komarovsky is often asked how to treat acute balanoposthitis in children. The specialist advises using an integrated approach and be sure to consult with doctors about any therapeutic measures.
Traditional treatment of acute forms of childhood balanoposthitis is based on the use of the following medications:
- biseptol;
- amoxicillin;
- amoxiclav;
- cefuroxime;
- bicillin;
- antifungal drugs;
- non-steroidal anti-inflammatory drugs;
- flumethasone;
- prednisolone ointment.
- rivanol;
- furatsilin;
- dioxidin.
Warm baths help effectively combat acute balanoposthitis in children. It is recommended to add the following ingredients:
Antiseptic treatment of the affected areas of the penis is carried out with Miramistin or Chlorhexidine.
For acute balanoposthitis in boys, treatment with conservative methods does not always have a positive effect. In this case, the doctor recommends circumcision of the foreskin. The best folk remedies for acute childhood balanoposthitis are antiseptic decoctions based on chamomile, oak bark, aloe, calendula, sage, and St. John's wort. The child should be given more liquid (teas, fruit drinks, juices, clean water). This will increase the number of urinations and help flush out pathogens naturally. To relieve pain, the child can be given ibuprofen.
Acute balanoposthitis, regardless of the patient’s age, can take different forms. The most common are herpetic, purulent, and fungal.
Herpetic balanoposthitis
Herpetic balanoposthitis is a complicated form of acute balanoposthitis. The disease affects the tissues of the head of the penis.
Why does herpetic balanoposthitis occur (photo)?
The development of herpetic balanoposthitis occurs under the influence of viruses, bacteria, and fungal infections. The cause of the disease is also a strong mechanical impact on the genital organ (for example, constant irritation with urine or rubbing with tight clothing). Herpetic balanoposthitis sometimes becomes a consequence of skin pathologies (for example, psoriasis).
The disease in question is of infectious origin and develops as a result of the herpes virus entering the patient’s body. Herpetic balanoposthitis can be recognized by a specific vesicular rash covering the surface of the head of the penis. Against the background of the rash, the skin of the penis becomes very red, and the reproductive organ itself becomes swollen. The patient most often has no subjective sensations, but sometimes the disease is accompanied by severe burning and itching in the area of the head of the genital organ.
Herpetic balanoposthitis in men: photos, treatment
Therapy for herpetic balanoposthitis is carried out using anti-inflammatory corticosteroid ointments. Additionally, local antiviral treatment of the disease is carried out. Inflamed areas of the genital organ are treated locally - with ointments, pastes or creams.
One of the reasons why herpetic balanoposthitis does not go away when treated with medications is the weakened immunity of the patient. For treatment of the disease to be successful, it is necessary to include immunostimulating drugs in the treatment complex. They will increase the body's resistance to adverse external factors.
Balanoposthitis of the herpetic form is characterized by a chronic relapsing course. Its treatment is carried out periodically and is aimed at preventing exacerbations.
Purulent balanoposthitis

The purulent form of balanoposthitis is always characterized by sudden and rapid development. The occurrence of acute inflammation and the formation of a purulent process are provoked by stagnation of urine and secretory secretions under the preputial sac. Purulent balanoposthitis is often a complication of advanced phimosis. The disease is very severe, has unpleasant symptoms, pain and serious complications.
Purulent balanoposthitis in children: symptoms and treatment
Purulent balanoposthitis in a child (photo) occurs for the following reasons:
- microorganisms belonging to a special, pyogenic microflora get onto damaged skin or inside the urethra;
- active destruction of healthy tissues by pathogenic bacteria (Escherichia coli, streptococci, staphylococci);
- worsening of the condition with ordinary catarrhal balanoposthitis;
- spread of purulent processes occurring in the kidneys or bladder to the urethra and urethra (with purulent cystitis or pyelonephritis).
Basically, purulent balanoposthitis in boys is a consequence of untimely attempts to lift the foreskin. Incorrect actions by parents lead to tears and small cracks appearing on the skin, into which infection penetrates. Bathing a baby in a bath with a lot of foam, using irritating hygiene products, and rarely changing diapers can also trigger the occurrence of acute purulent balanoposthitis.
Purulent forms of inflammation of the head and foreskin of the penis are accompanied by severe redness of the skin on the reproductive organ and its swelling. In particularly difficult situations, the head of the penis turns blue. In individual cases, the child may develop rashes, the boy becomes capricious, restless, constantly cries and complains of soreness in the genital organ. Another sign of purulent balanoposthitis is the appearance of diaper rash in the folds of the skin, in the groin area. Diaper rash does not disappear after using special ointments, powders or creams.
Purulent balanoposthitis in newborn male babies can be a consequence of damage to the mucous membranes of the oral cavity. Outwardly, it looks like an accumulation of milk clots. Stomatitis can also provoke inflammation of the genital organs in childhood.
Purulent balanoposthitis in men: signs and factors
The occurrence of purulent balanoposthitis in an adult is associated with insufficient or improper hygiene of the external genitalia, advanced inflammation or phimosis. With this form of the disease the following symptoms occur:
- swelling of the penis, a pronounced inflammatory process with redness of the skin;
- discharge of pus with an unpleasant odor from under the foreskin or from the urethral canal;
- the formation of pustules and ulcers on the surface of the head of the penis.
Correct and timely treatment of purulent balanoposthitis prevents the development of complications, helps destroy pathogens and helps maintain health.
Purulent balanoposthitis in a child: treatment
Therapy for purulent forms of balanoposthitis is carried out with special creams or ointments. Dermatologists recommend using Levomekol and Lorinden ointments. Warm baths with the addition of furatsilin and potassium permanganate will have an additional therapeutic effect.
Compared to ordinary inflammation, purulent balanoposthitis is considered a more dangerous condition. Its development in children is accompanied by a deterioration in health and an increase in body temperature. To speed up the process of treatment and recovery, surgical opening of existing abscesses is performed, followed by washing of the pathological areas with antiseptic solutions. Control over the treatment process for adult men is carried out by a surgeon, dermatologist or venereologist, and for little boys - by a pediatrician. Drug therapy can be supplemented with herbal decoctions and tinctures of chamomile, calendula, and oak bark. They rinse the affected organ and use it to create healing compresses and lotions.
At the diagnostic stage, purulent balanoposthitis must be differentiated from fungal inflammation, in which pus can also be released from the penis.
Fungal balanoposthitis
Fungal balanoposthitis is a common type of inflammatory process in the male genitourinary system. The causative agent of the disease is fungi of different structures, but most often the inflammatory process develops due to the entry of Candida bacilli into the urethral canal.
Fungal balanoposthitis in men - photos, etiology and symptoms
The causative agents of fungal balanoposthitis live on the mucous membranes of the oral cavity, in the female vagina or intestines. They infect the body through sexual contact, as well as through the use of common household items (towels, soap) or due to poor hand hygiene.
Clinical manifestations of fungal infection in men may be absent for a long time. Symptoms appear only when the immune system is weakened (for example, as a result of prolonged antibiotic therapy).
Fungal balanoposthitis (photo) is accompanied by the following symptoms:
- pain in the penis during sexual intercourse;
- burning, itching and dryness at the site of development of the inflammatory process;
- difficulties when trying to remove the head of the genital organ;
- cutting pain occurs during urination;
- severe redness of the skin of the foreskin and glans;
- a white-gray cheesy coating with a sour odor on the skin of the reproductive organ.
If the infection during fungal balanoposthitis spreads to the internal mucous membranes of the urethral canal, urethritis develops. With this complication, sharp pain occurs, and blood and mucus are released when urinating. Advanced fungal balanoposthitis leads to the development of cystitis, pyelonephritis, vesiculitis or prostatitis. However, if you go to the hospital in a timely manner, the course of treatment is quick and successful.
Fungal balanoposthitis: treatment
Balanoposthitis of a fungal nature is treated with medication and folk methods. After diagnosing this form of the disease, the doctor prescribes systemic medications (Fluconazole, Nystatin, Ketoconazole), local medications (Mikogel, Dermazol), treatment with antiseptic solutions of Miramistin, Chlorhexidine, Furacilin, Dioxidine and a weak mixture of potassium permanganate and water. During treatment, the patient should avoid sexual intercourse. At the same time as the man, his sexual partner must undergo a therapeutic course. It is advisable to include vitamin supplements and medications that strengthen the immune system in the course of treatment. Also, a patient with fungal balanoposthitis should reconsider his diet. Preference should be given to lean meat, cereals, fish, fruits, vegetables, and nuts. It is better to avoid sweets, salty and smoked foods, flour and bakery products, and canned foods.
Traditional medicines prepared on the basis of calendula (oil infusion, decoction), chamomile, sage, and St. John's wort will also help speed up the process of treating fungal balanoposthitis.
Balanoposthitis and its treatment

For balanoposthitis in men, treatment (photo) always begins with a set of diagnostic measures. The doctor invites the patient to undergo tests to identify the cause of the developing pathology and determine the type of pathogen. The results of laboratory tests are used as a basis when drawing up a treatment plan.
How to cure balanoposthitis - drugs, ointments, tablets or surgery?
Before starting treatment for balanoposthitis, the doctor gives the patient recommendations, compliance with which helps prevent the development of complications and relapses of the disease.
The first rule for successful treatment of the disease is daily hygiene of the foreskin and glans.
Fighting the pathogen with local means (herbal decoctions and tinctures, antiseptic solutions to relieve inflammation).
The use of antiviral and antibacterial drugs (the treatment regimen is developed by the urologist individually for each patient).
Men suffering from inflammation of the foreskin and head of the genital organ, first of all, want to find out how and how balanoposthitis is treated (tablets, ointments, antiseptics or surgical methods). The attending physician determines the method of therapy based on the complexity and severity of the disease, the form of balanoposthitis, and the presence of complications. The main ways to combat this disease are described below.
Regardless of the form of balanoposthitis, local anti-inflammatory ointments (combined and corticosteroid) are used for its treatment. Dermatologists and urologists advise giving preference to the drugs Triderm and Levomekol.
If balanoposthitis occurs with complications, as an additional treatment, the patient is prescribed medications that strengthen the immune system and increase the resistance of the immune system to attacks by pathogens.
Balanoposthitis of the candidiasis form is treated with antifungal agents (Clotrimazole ointment, Nizoral).
To cure anaerobic balanoposthitis, antibiotics are used (for example, Azithromycin).
Treatment of balanoposthitis through surgery is carried out if phimosis develops against the background of the disease. In this situation, the man's foreskin is cut off.
Alternative medicine and its techniques relieve pain and eliminate swelling in balanoposthitis of any form. Compresses, baths, washing the skin of the penis and penis with herbal infusions or antiseptics - all these methods help cope with pain and alleviate the patient's condition during an acute inflammatory process.
How to treat balanoposthitis in men?
Therapy for balanoposthitis in adult men is based on an integrated approach. The doctor prescribes medications from the following list:
- ointments (synthomycin, Levomekol, Triderm);
- medications (Clotrimazole solution or aerosol, Diflucam tablets, Nystatin, Levorin);
- folk remedies (decoctions of oak bark, chamomile, string, dill, sage; solutions of potassium permanganate, soda, dioxidin, furatsilin; aloe, dill and plantain juice).
An adult patient can treat balanoposthitis with ointments and creams at home. To disinfect the inflamed genital organ before applying the ointment, use antiseptic compounds. For example, many doctors recommend using furatsilin for balanoposthitis (treatment (photo) is carried out by adding the named remedy to a healing bath). Furacilin is also used to create lotions. The drug is an antimicrobial drug that helps fight gram-positive and gram-negative microorganisms. They treat wounds, purulent inflammations, and bacterial dysentery. Its analogues are a solution of potassium permanganate, chlorhexidine, and hydrogen peroxide. The advantage of furatsilin is that it is available over-the-counter in pharmacies. The anti-inflammatory, antimicrobial regenerating drug Bepanten has the same advantage. It comes in the form of a cream, lotion or ointment. Bepanten cream gives a good therapeutic effect for balanoposthitis in children. It is prescribed for the prevention and treatment of the disease, eliminating rashes from constant contact with diapers in newborn babies, as well as treating diaper rash.
Balanoposthitis in a child: treatment
Children's balanoposthitis is treated by a urologist. Therapy for the disease is mandatory, since the inflammatory process will not go away on its own. Moreover, the absence of medicinal measures will lead to aggravation of the problem - the pathological condition of the foreskin and glans will become chronic. Before starting treatment, the doctor prescribes a set of tests for the small patient and conducts differential diagnostics. If balanoposthitis is diagnosed in a child (photo), treatment is based on the use of conservative methods. It is recommended to use ointments, baths with herbal decoctions, antibacterial tablets, lotions, antiseptic solutions (a good remedy is Miramistin ointment or solution for balanoposthitis in a child). If the disease is severely advanced, the child is sent to a surgeon and his foreskin is cut off. In the early stages of balanoposthitis, antiseptic powders help well. They remove diaper rash.
Balanoposthitis and diabetes: treatment of combined pathologies and its features
Particular attention should be paid to the treatment of balanoposthitis that develops against the background of diabetes mellitus. Primary treatment in this situation is aimed at eliminating the symptoms of diabetes. If you immediately take measures to treat the inflammatory process on the reproductive organ, they will not give any result. Balanoposthitis, in fact, is a complication of diabetes mellitus. If you do not get rid of the underlying disease, inflammation of the head of the penis and foreskin will become chronic. To relieve the symptoms of balanoposthitis, it is necessary to normalize the level of glucose in the patient’s blood (after all, diabetes itself is an incurable chronic pathology). The treatment process is controlled by a urologist and endocrinologist. You should not self-medicate, since balanoposthitis can cause complications in the form of decreased sensitivity of the head, painful sexual intercourse and problems with urination. Circumcision of the foreskin in diabetes is not advisable until blood glucose levels are stabilized.
The main conservative method of treating balanoposthitis involves the use of antibiotics and ointments.
Antibiotics for balanoposthitis
When balanoposthitis develops in men (photo), treatment with antibiotics helps eliminate inflammation, prevent re-infection with pathogens and overcome pathogenic microflora. Usually, after diagnosing balanoposthitis, doctors prescribe medications to the patient in the form of ointments, creams or tablets. If the disease is in the acute stage, treatment is carried out with intramuscular injections. The course of antibacterial treatment is developed individually for each patient. There is no universal cure for this disease. The action of one or another group of antibiotics is aimed at destroying pathogens of a certain category. Before starting antibiotic therapy, the doctor uses test results and symptoms to determine the nature of the disease. The main indication for immediate initiation of antibiotic treatment is advanced forms of non-infectious balanoposthitis, as well as complications that arise after injuries. In addition, a course of antibacterial treatment is carried out when pathogens of sexually transmitted infections are detected in the patient’s body.
Balanoposthitis in men: treatment with antibiotics. When is it recommended to use antibacterial drugs?
Antibiotics for balanoposthitis in men receive mixed reactions from patients in reviews. The reason for the ineffectiveness of these drugs is often associated with incorrect identification of the form of the disease. Antibacterial therapy does not give the desired results if balanoposthitis is caused by fungi or viruses or is non-infectious. The doctor’s task before prescribing a course of antibiotics is to do allergy tests of the medications that the patient will take. The presence of an allergy to a certain group of drugs is a contraindication to starting antibiotic therapy.
What antibiotics treat balanoposthitis?
The attending physician can answer the question of how to treat balanoposthitis and which antibiotics are most effective for this disease. He carefully studies the patient’s medical history, looks at test results, determines the type of pathogen, and selects a group of medications and dosage. If balanoposthitis occurs against the background of sexually transmitted diseases, the course of treatment is controlled by a venereologist. If the nature of the disease is different, the patient is treated by a urologist.
To find out which antibiotics to take for balanoposthitis, a man needs to undergo a full examination. Most often, the doctor prescribes medications in film-coated tablets. In order for them to give the desired therapeutic effect, they must be taken correctly.
Do not take tablets before bedtime.
It is better to take medications in tablets 1 hour before a meal or 2 hours after a meal.
The medicine should be taken with plenty of water (at least 1 glass).
You need to take the tablets with non-carbonated purified water (boiled or distilled). Do not take tablet medications with milk, tea, coffee or juice.
Antibacterial treatment of balanoposthitis is most often carried out using drugs from the following list.
Triderm. A drug for external use containing antifungal and hormonal components, as well as the antibiotic gentamicin. The ointment is suitable for compresses and rubbing, the duration of use is 1-2 weeks. The drug can be combined with oral medications. The use of Triderm does not lead to adverse side effects associated with the development of a fungal infection.
Suprax (against sexually transmitted infections). A drug in capsules from the group of cephalosporins with the active substance cefixime. The product is well tolerated by the body, is highly resistant to enzymes that can destroy antibiotics, and is suitable for patients with weakened immune systems. Suprax actively affects gonococci, pneumococci, salmonella, E. coli, streptococci. However, it does not provide a therapeutic effect in the fight against listeria, staphylococci, and Pseudomonas aeruginosa. The daily dosage of the drug is 1 capsule. The treatment period is determined by the doctor individually.
Suprax (antimicrobial, helps remove purulent microflora, staphylococci and streptococci). Medicine in film-coated tablets. The active component furazidan effectively destroys pathogenic microorganisms, staphylococci and streptococci. With its help, suppuration is quickly removed, pain and discomfort when urinating are reduced. An overdose of a medicine can cause side effects.
Azithromycin. One of the most effective drugs for balanoposthitis of any form. The antibiotic is suitable for the treatment of diabetic, non-infectious, sexually transmitted forms of pathology. The drug is available in capsules and contains azithromycin. The duration of therapy depends on the general condition of the patient and the type of infectious agent. Azithromycin should not be combined with other medications. The use of other medications is permitted a few days after completion of treatment with this drug.
Doxycycline. Tetracycline group drug in tablets. Suitable for the treatment of balanoposthitis of various forms, there is no adverse effect on the functioning of the digestive organs. The medicine has a minimal number of contraindications; it can be used to treat balanoposthitis in weakened and elderly patients. The dosage and duration of treatment are calculated individually, but the doctor immediately draws attention to the fact that Doxycycline should be combined with laxatives containing magnesium, iron supplements, and antibiotics from the penicillin group.
Levomycetin. A popular remedy for balanoposthitis. The active components of Levomycetin have a good effect on many pathogenic microorganisms (Staphylococcus aureus, smegma microbacteria, streptococci, Staphylococcus aureus, gonococci, Pseudomonas aeruginosa). The active substance of the same name is quickly absorbed into the blood and gives the first therapeutic effect after 2-3 hours. The advantage of Levomycetin is that pathological microorganisms slowly get used to its components. The tablets destroy the existing bacterial microflora and suppress its vital activity. Most often, Levomycetin is used to treat initial forms of balanoposthitis.
Antibiotics provide a powerful antibacterial effect, but their use for balanoposthitis is not always possible. Find out what contraindications exist for using this drug.
Balanoposthitis and antibiotic treatment, side effects and contraindications
Potent antibacterial drugs cannot be used to treat balanoposthitis if the following factors are present:
- malignant tumors;
- autoimmune diseases;
- severe chronic pathologies;
- liver and kidney failure;
- blood clot formation, thrombosis;
- allergies to antibiotic components;
- heart failure.
An incorrectly formulated course of treatment or an overdose of the drug leads to the development of side effects. They are associated with the following unfavorable conditions:
- dizziness;
- headache;
- convulsions;
- vomit;
- nausea;
- convulsions;
- persistent stool disorder;
- loss of consciousness;
- temporary deterioration of visual functions.
To enhance the therapeutic effect of taking antibiotics, the urologist prescribes additional auxiliary agents to the patient.
Therapy for balanoposthitis after antibiotics or how to supplement the main course of treatment?
Treatment of balanoposthitis in adult men, on the one hand, benefits the body by killing pathogenic microflora. But at the same time, such drugs also destroy beneficial microorganisms, reduce the patient’s immunity and provoke the development of a fungal infection. To reduce the negative effects of antibiotics, they should be supplemented with other medications. For example, to prevent and prevent fungal diseases (mycoses, candidiasis), the patient must take antifungal medications (Pimafucin, Clotrimazole, Pimafucort, Miconozol).
It is convenient to combine oral medications against balanoposthitis with medicinal ointments, alternating courses of 7-10 days. If there is damage to the skin of the genital organ, appropriate medications are used to accelerate regeneration ( the best way Levomekol ointment is considered in this category).
Antiseptic treatment of the inflamed genital organ is also important and necessary. It is carried out using special solutions (Chlorhexidine, Miramistin). The preparations are suitable for creating lotions, douching, and washing the affected organ. There are no contraindications to the use of antiseptics; the course of therapy with their use is 1-2 weeks. Antiseptic solutions can treat acute and chronic forms of balanoposthitis.
Homemade antibacterial remedies in the form of decoctions and infusions of chamomile or a weak solution of potassium permanganate can be used to create healing baths. If small wounds and ulcers appear on the head and foreskin of the genital organ, they are cauterized with Fukortsin or similar antiseptics for topical use.
Traditional methods of treatment
Patients diagnosed with balanoposthitis traditional treatment prescribed to achieve an auxiliary therapeutic effect. It is used to eliminate severe and unpleasant symptoms of the disease. In general, home therapy for balanoposthitis is allowed only in the initial stages of the disease, when it has not yet been complicated by concomitant ailments. Having noticed the first signs of the disease, a man should immediately strengthen the rules of intimate hygiene. Sometimes, to eliminate the onset of pathology, it is enough to thoroughly wash the head of the penis for several days with antibacterial soap and warm water.
If water procedures with soap do not give a positive result, you should begin antiseptic treatment of the genital organ. Washing the penis with antibacterial solutions of Miramistin or Chlorhexidine is carried out during the 1st week. Before using antiseptics, the head of the penis is washed with the same water and soap. Furacilin and hydrogen peroxide give a good effect in home treatment of initial forms of balanoposthitis. It is better not to use other solutions for disinfecting an inflamed organ (iodine, alcohol tinctures, potassium permanganate), as they provoke a decrease in the sensitivity of receptors on the genital organ and burns.
The ineffectiveness of antiseptics indicates reduced immunity, and in this situation the problem can only be solved with the help of a urologist. He will select the necessary medications and prescribe the dosage, focusing on the individual parameters of the patient’s body. To achieve the highest effectiveness of treatment of balanoposthitis, a daily change of underwear and hygiene procedures will help, during which the secretory fluid accumulated there is thoroughly washed out from under the folds of the foreskin.
Balanoposthitis: folk remedies for treating the disease, giving the best effect
In patients with balanoposthitis, treatment at home (photo) is based on the use of herbal remedies for external and internal use. Medicines prepared according to recipes from the folk piggy bank help to overcome inflammation and cope with the disease. These include:
- decoctions and infusions of medicinal herbs (chamomile, calendula);
- antiseptic solutions (furacilin, miramistin, chlorhexidine);
- applications and compresses of antimicrobial ointments (the best therapeutic effect is provided by Levomekol, and fungal balanoposthitis is recommended to be treated with Candida or Clotrimazole).
At home, you can make baths for balanoposthitis using herbal decoctions or antiseptics. With their help, itching, burning, inflammation, swelling and redness of the genital organ are eliminated. Regular use of baths allows you to get rid of ulcers on the penis and purulent discharge. Disinfecting baths help eliminate the symptoms of balanoposthitis at the very beginning of its development. Below is a selection of 5 good recipes for preparing such baths.
- Furacilin. To prepare the solution, you need to buy a 0.02% solution of furatsilin at the pharmacy. Before the procedure, fill the bathroom with water at room temperature. The active component of the antiseptic drug is the substance nitrofuran. Some patients experience individual intolerance to the drugs. It is necessary to clarify this point in advance and, if such a feature is present, to refuse treatment of balanoposthitis with furatsilin.
- Potassium permanganate (potassium permanganate). This component is diluted in boiled water in proportions of 1:5000. The finished potassium permanganate solution should turn out pale pink. Crystals of potassium permanganate must be completely dissolved in water, since solid particles of the substance cause a burn when they come into contact with the skin. Take a bath with potassium permanganate for 3-10 minutes.
- Soda. A good component that can cure balanoposthitis is soda (sodium bicarbonate). It is added to antibacterial baths before bathing. The product does not cause allergic reactions on the skin, and there is no risk of overdose when using it. Soda in the amount of 1 tbsp. diluted in water at room temperature. The duration of the procedure reaches 3-10 minutes.
- Dioxidine. Baths with the addition of 1% dioxidine solution are recommended for the treatment of purulent forms of balanoposthitis. The bath is taken for 10-15 minutes and it is very important that the antiseptic solution gets onto all areas of the penis and even under the foreskin (where pus usually accumulates).
- Oak bark. Dry oak bark, ground into powder, is an excellent antiseptic. A decoction for baths is prepared from it (1 tablespoon of powder is poured into 1 glass of boiling water and boiled over low heat for about 20 minutes). Next, the broth is cooled and infused for half an hour, then the product is added to the bath, after diluting with 1 glass of water at room temperature. The duration of the treatment procedure is 10-15 minutes.
- After taking a disinfectant bath, it is not recommended to vigorously wipe the penis with a towel. It is better to blot the organ with clean, dry wipes. After such treatment, be sure to wear clean underwear.
How to treat balanoposthitis in men at home
Home therapy for balanoposthitis in adult men is based on solving several important problems.
Careful intimate hygiene of the genital organs. The penis must be washed daily with soap and the head must be cleaned of accumulated secretory fluid. If balanoposthitis is detected in a timely manner in men, treatment at home for this pathology is successfully carried out using hygienic measures alone. Just a few days of thorough cleansing of the genital organ with soap and water - and drug therapy may not be needed at all.
To cure an advanced form of balanoposthitis, it is necessary to use local antiseptics for 1 week. Chamomile decoction helps a lot.
If antiseptic therapy at home is ineffective, the patient can work on strengthening the immune system. General strengthening therapy is based on the total saturation of the weakened body with vitamins. It is recommended to drink decoctions and teas from black currant leaves, burdock roots, and aspen bark. It is necessary to include fresh juices in your diet and adhere to a diet.
Treatment of balanoposthitis in men at home also depends on the form of the disease. For example, garlic and garlic oil help get rid of a fungal type of illness. In addition, the fragrant cloves have a powerful bactericidal effect. Garlic can be taken orally or applied to the glans penis as a compress. The second treatment option is recommended to be carried out with caution in order to prevent burns to the sensitive tissues of the penis.
A highly effective remedy for home treatment of balanoposthitis in an adult are applications and compresses from medicinal plants. They are applied fresh to the inflamed head of the penis and changed every 30 minutes. To create applications for balanoposthitis, phytocomponents from the following list are used.
Aloe. The plant relieves swelling, inflammation, itching and pain well. To treat balanoposthitis, use leaves of a 3-year-old plant, plucked from the lower part of the trunk and previously peeled. Aloe juice is suitable for creating lotions and compresses.
Plantain. The plant has long been famous for its analgesic and anti-inflammatory properties. Before use, fresh leaves of the plant are washed, kneaded and fixed on the affected area with a bandage. Every half hour the used piece of paper is replaced with a new one.
Eleutherococcus. Natural broad-spectrum antibiotic. It is best to use it in the form of tea, brewing 1 tablespoon in 200 ml of water.
Yarrow. A healing tea is also prepared from this plant, which helps destroy enterococci and streptococci. Add 1 tsp to 1 glass of boiling water. dried yarrow herb, leave for 1 hour, filter and consume internally.
Honey. The main bee product is used to enhance the healing effect of medicinal herbs. If the patient has no contraindications to the use of honey (for example, individual intolerance or allergies), it can be added to herbal teas, infusions and decoctions.
Calendula. Olive oil mixed with calendula flowers is a good treatment for balanoposthitis, complicated by wounds and ulcers on the genitals. To prepare the medicinal composition, 20 g of dried and carefully crushed calendula flowers are poured into a glass container, then poured with olive oil (1/3 cup), closed with a lid and left in the sun or in a warm, dry place for 3 weeks. Then the calendula oil is filtered and used to treat the affected areas of the penis.
Sage. The dried plant in an amount of 20 g is dissolved in 0.5 liters of boiling water. Then the composition is removed in a warm place for half an hour, after which it is filtered and used to create compresses or rinses of the penis.
St. John's wort. St. John's wort flowers (30 pieces) are crushed and poured with boiling water (200 ml). The finished composition is infused for 1-2 hours, filtered through gauze and washed with it on the penis.
Chamomile. Dried flowers of a medicinal plant (30 g) are brewed with boiled water (30 ml). Then gauze is moistened with this mixture, and chamomile flowers are placed on it. The finished compress is applied to the inflamed area of the genital organ.
Cabbage. A compress of cabbage leaves, finely chopped and mixed with vinegar and boiled beans, is used to lubricate the head of the penis. It is recommended to carry out the procedure before a night's rest, and to wrap the penis in a towel or terry cloth after applying the cabbage and bean paste.
Traditional methods of therapy help eliminate balanoposthitis in a child, and treatment at home with their use demonstrates a good effect. A good remedy for this disease would be regular laundry soap. It is grated and diluted with clean boiled water to form a semi-liquid paste. Then the inflamed penis is washed with this mixture.
Balanoposthitis: how to treat at home with diet
Treatment of balanoposthitis at home (photo) is recommended to be supplemented proper nutrition. Lifestyle correction for this disease requires the fulfillment of several important conditions.
The patient should have proper rest and adhere to an optimal sleep schedule.
You should completely give up alcohol, energy drinks, cocktails, beer, stop smoking and not expose your body to stress during the entire treatment and after it.
You need to adhere to a balanced diet, exclude fatty, spicy, overcooked foods from the menu, add berries, dairy products, fruits and vegetables to your diet.
If you have balanoposthitis, you should not drink strong coffee or tea.
Every man should remember that alcohol and alcoholic beverages provoke the development of obesity, reduce immunity and generally go very poorly with taking medications. During the treatment of balanoposthitis, exposure to tobacco tar and nicotine vapor on the body is extremely undesirable. The patient should stop smoking classic cigarettes and their electronic substitutes.
Personal hygiene during balanoposthitis is best done in the shower. Taking hot baths, going to the bathhouse or sauna is stopped for a while. Traditional methods of treating balanoposthitis can be included in complex therapy, used together with antibiotics and ointments.
Ointments for balanoposthitis

Men whose doctors have diagnosed balanoposthitis use ointment to treat this disease as part of a comprehensive therapeutic regimen. Its analogues are antibacterial gels and creams. Do ointments always help cure balanoposthitis? Can they be replaced with tablets or is it better to use such medications in combination? This will be discussed further below.
Balanoposthitis in men - treatment with ointments or tablets, what to choose?
Ointments, gels and creams for balanoposthitis most often have increased fat content and a dense texture. They contain not only active antimicrobial components, but also pure paraffin, cosmetic lanolin, natural wax, synthetic and plant origin. After application to the skin, they form a thin film on it. Fatty formulations are ideal for the treatment of erosive and simple balanoposthitis. To treat a fungal type of illness, it is better to use a cream with a light structure.
Therapy for balanoposthitis with ointments is good because the drugs act on the affected area locally and practically do not penetrate into the blood. The active components of the remedy are quickly eliminated from the body without accumulating in the internal organs. Male patients often ask urologists the question of which forms of antibacterial drugs for balanoposthitis can be called more effective - are they ointments, tablets? Doctors pay attention to the fact that oral medications can be used in complex treatment inflammatory process simultaneously with ointments and creams. The difference between these drugs is the method of action. The tablets are taken orally and provide a general therapeutic effect and eliminate the causes of the disease. Ointments work locally, on the surface of the skin, helping to cope with the consequences of the inflammatory process (burning, itching, redness of the skin). In addition, the active substances take longer to be eliminated from the body after taking the tablets.
Treatment of balanoposthitis: the best ointment
Ointment for balanoposthitis in men is selected individually by the attending physician. There are several main drugs recommended for use in the treatment process. Ointments from the following list are considered the best in the fight against inflammation of the male genital organ.
- Triderm. Reviews about the treatment of balanoposthitis with Triderm are mostly positive. Patients call this remedy effective and the best for treating inflammation of the head of the penis and foreskin. The drug gives a good effect in all forms of the disease. Triderm for balanoposthitis in men is used for 3-4 weeks. They apply it to the affected areas of the genital organ three times a day. The anti-inflammatory and antibacterial drug contains 3 important components: gentamicin (helps cope with the activity of pathogenic microorganisms), clotrimazole (destroys fungal agents), betamethasone (anti-inflammatory and antiallergic ingredient). True, there are situations when Triderm does not help with balanoposthitis. This occurs due to the patient’s individual intolerance to the components of the drug, as well as in advanced cases when balanoposthitis is accompanied by phimosis and surgical intervention is required to eliminate the disease.
- Clotrimazole. The drug actively fights pathogenic microorganisms and bacteria. The ointment includes methyllaraben, paraffin and active ingredients that help fight the cause of the disease and eliminate the inflammatory process. The ointment is applied to the inflamed areas of the skin of the penis 2 times a day. The course of therapy is 3 weeks, but in individual cases and in the presence of complications, the doctor can extend it to 1 month.
- Miramistin. This drug kills pathogens and bacteria quite quickly, so doctors recommend using it to treat bacterial-type balanoposthitis. Apply a thin layer of ointment to the skin of the penis once a day, before going to bed at night. Miramistin can be used in the form of compresses (a bandage or gauze soaked in it is applied to the affected areas of the penis and held there for 2-3 hours).
- Levomekol. An antibacterial agent against balanoposthitis, containing the active component methyluracil. This drug treats acute and chronic inflammation well. Pediatricians and urologists recommend using Levomekol for balanoposthitis in a child. This ointment gives the best effect if used as part of a compress. The drug is applied to a bandage folded in several layers, and then applied to the inflamed skin of the penis 1-2 times a day.
- Pimafukort. An effective medicine to combat balanoposthitis, it perfectly relieves inflammation, destroys the causative agent of the disease, and removes pain. Due to the presence of several components in the composition of the product (hydrocortisone, natamycion, neomycion), it has a complex therapeutic effect on the body. It is recommended to apply the ointment 3 times a day for 3 weeks. True, Pimafucort has a number of side effects (skin itching, formation of stretch marks, skin rash).
- Lamisil. The action of this drug is aimed at destroying microbes and fungi. Doctors recommend using Lamisil as an additional remedy against acute balanoposthitis. At the same time, experts point out that Lamisil is not suitable for people with very sensitive skin and children under 12 years of age. Most often, the drug is applied to damaged skin of the genital organ, but in severe situations it is used as part of a gauze compress. It is applied in the evening and left on the penis overnight.
- Fluconazole. Answering the question of how to treat fungal balanoposthitis and which ointments help best in the fight against this disease, urologists immediately recommend Fluconazole. The drug is ideal for the treatment of candidal balanoposthitis; it is quickly absorbed into the skin and has a long period of action. Fluconazole is applied to the affected areas of the penis once a day, before going to bed at night.
- Pimafucin. The action of this product is aimed at destroying fungal infections and yeast bacteria. To increase the effectiveness of the medicine, it is combined with Pimafucin tablets (they are taken orally).
- Akriderm. An antiallergic medicine that can treat not only balanoposthitis, but also allergic rashes of a different nature. The ointment quickly eliminates itching and inflammation in the external genitalia. The manufacturer's instructions recommend using it for 3-4 weeks.
- Syntomycin ointment. This drug has the same principle of action as Triderm cream for balanoposthitis. Synthomycin ointment can treat any form of balanoposthitis, including pathology accompanied by suppuration. The drug is applied 3 times a day, in a thin layer, to the skin of the inflamed reproductive organ.
All of the above ointments are only an additional aid for balanoposthitis. They help relieve acute symptoms, but do not always have an effect on the cause of the disease. In addition, such drugs have many side effects, due to which the doctor has to adjust the treatment regimen.
Balanoposthitis(from the Greek balanos - “acorn”, “head of the penis”, posthe - “foreskin”, and itis - “inflammatory process”) is an inflammation of the head of the penis (balanitis) and the foreskin (posthitis).
Anatomical features of the glans and foreskin of the penis
The human penis consists of a body and a head, between which there is a narrowed part - the neck (coronal groove).The head of the penis is acorn-shaped and contains the external opening of the urethra, which serves both for urination and ejaculation.
The head of the penis is covered with thin pink skin, which contains many glands that secrete lubricant - smegma. It performs a protective and bactericidal function.
Normally, the head is completely or partially covered by the foreskin - a fold of skin that covers its body in the upper part of the penis and passes into the skin of the pubis, and in the lower part into the skin of the scrotum. In the lower part, between the foreskin and the glans, another fold of skin runs longitudinally - the frenulum of the penis.
Smegma, which is produced by the skin glands, accumulates between the skin and the head of the penis.
Causes of balanoposthitis
The causes of balanoposthitis are divided into infectious and non-infectious.Causes of infectious balanoposthitis(mainly sexually transmitted infections):
- Gonorrhea– sexually transmitted infection ( STI), caused by gonococcus.
- Trichomoniasis- a sexually transmitted infection that occurs in 10% of the world's population. It ranks first in prevalence among both STIs and diseases of the genitourinary system.
- Candidiasis– a fungal disease that develops mainly with decreased immunity.
- Genital herpes is a viral infection that mainly affects the skin and genitals.
- Syphilis – Balanoposthitis may be the first sign of primary syphilis.
- Gardnerellosis – in women it occurs as a result of a violation of the normal biocenosis (composition of microflora) of the vagina, and in men it manifests itself in the form of balanoposthitis.
- HPV (human papillomavirus) – a common viral disease that affects the skin and mucous membranes, which often manifests itself in men in the form of balanitis, posthitis, balanoposthitis.
- Nonspecific pathogens – Among them, the most common are streptococci and staphylococci.

- Irritative balanoposthitis – associated with mechanical or other irritation of the skin of the glans and foreskin of the penis.
- Diabetes - complicated by balanoposthitis as a result of damage to small vessels of the penis, decreased protective functions.
- Psoriasis – a dermatological disease that is mainly of an autoimmune nature.
- Lichen planus – non-infectious chronic skin disease.
- Rarely occurring diseases: Keir's erythroplasia, Behçet's disease, xerotic balanoposthitis obliterans, Zoon's plasma cell balanitis.
- Failure to comply with personal hygiene rules: Moreover, dirt and smegma, which accumulate between the foreskin and the head of the penis, are an excellent breeding ground for the proliferation of pathogenic microorganisms.
- Phimosis: a disease in which the foreskin is so narrowed that it is impossible to expose the head of the penis. In this case, personal hygiene is difficult.
- Allergic diseases and immune disorders.
- Chronic infections in the body: pathogenic microorganisms enter the skin of the glans penis through the bloodstream.
- Promiscuity: high risk of contracting sexually transmitted infections.
- Infections of the genitourinary system: cystitis, prostatitis, urethritis, etc.

Symptoms of balanoposthitis
 Most often, balanoposthitis develops as a result of a banal violation of personal hygiene rules and is accompanied by typical symptoms. The dominant signs depend on the stage of the disease.
Most often, balanoposthitis develops as a result of a banal violation of personal hygiene rules and is accompanied by typical symptoms. The dominant signs depend on the stage of the disease. Symptoms of balanoposthitis at different stages of the disease
Simple balanoposthitisThe mildest form of inflammation of the glans penis and foreskin. Most often, balanoposthitis occurs in this way; complete recovery occurs in 5 to 7 days.
Symptoms of simple balanoposthitis:
- Itching and burning. They are often the first symptoms of the disease. These sensations intensify when touching the head of the penis and its foreskin, from rubbing underwear, during urination.
- Unpleasant sensations when opening the head of the penis.
- Redness of the glans penis and foreskin. A characteristic sign of the inflammatory process.
- Swelling
- Maceration of the skin of the foreskin and glans penis. Maceration is swelling resulting from the skin becoming saturated with edematous fluid.
- Formation of erosions on the skin– superficial defects that are especially painful.
- Purulent discharge from the external opening of the urethra.
A characteristic sign of this form of balanoposthitis is the formation of erosions on the skin of the glans and foreskin of the penis. First, a white thin film appears in a certain small area, which consists of a superficial dead layer of cells. Then it falls off, and in its place a very painful, itchy red spot forms. After the erosions heal, no trace remains in their place.
Often, erosive balanoposthitis is accompanied by enlarged and painful lymph nodes in the groin area.
Gangrenous balanoposthitis
The most severe form of the disease.
Signs of gangrenous balanoposthitis:
- violation of the patient’s general condition: malaise, fever, weakness;
- ulcers: appear on the head of the penis and its foreskin, are red in color, blood and pus appear in them, they are very painful;
- phimosis(inability to expose the glans penis): occurs as a result of swelling of the glans and foreskin;
- scarring: remain in place of healed ulcers and can also lead to the development of phimosis;
- perforations (holes) in the foreskin, which are also a consequence of the formation of ulcers.
Symptoms of balanoposthitis caused by certain sexually transmitted infections
| Type of balanoposthitis | Signs |
| Gonorrheal | Accompanied by classic signs of balanoposthitis, it is almost always combined with urethritis - damage to the urethra. |
| Chlamydial | Most often it occurs in the form of balanitis - inflammation of the glans penis. The lesions in the form of red spots have clear contours. |
| Trichomonas | Most often it occurs as a complication of urethritis, but can develop independently. A large amount of pus accumulates between the head of the penis and the foreskin, which has a yellow or white color, a foamy consistency, and an unpleasant odor. The head of the penis is either completely swollen and red, or is affected in the form of many spots. |
| Candida | The disease begins with itching and burning of the skin of the penis, then pain occurs. Subsequently, a white coating appears on the head of the penis, which is easily removed and forms lumps similar to cottage cheese. |
| Herpetic | A large number of blisters filled with transparent watery contents appear on the skin of the glans penis and foreskin. When they open, erosions of a red-pink color remain in their place, in place of which pigment spots then remain. Herpetic balanoposthitis most often occurs in a chronic form. |
| Syphilitic | With syphilis, balanoposthitis is associated with the formation of a primary chancre on the skin of the glans penis and foreskin. |
| Balanoposthitis with gardnerellosis | The symptoms resemble simple balanoposthitis, but are very scarce. If the man’s immune system is normal, then the disease goes away on its own within 2 to 3 days. |
| Papillomavirus balanoposthitis | It manifests itself, like human papillomavirus infection in other areas, in the form of genital warts. |
Specific symptoms of some types of balanoposthitis caused by non-infectious causes
| Type of balanoposthitis | Symptoms |
| For diabetes | The severity of symptoms depends on the patient’s age, duration of diabetes mellitus, and concomitant diseases:
|
| Psoriatic | In most cases, balanoposthitis in psoriasis is combined with skin lesions in other places. In this case, small red nodules appear, covered with scales. |
| For lichen planus | Flat, irregularly shaped nodules appear on the skin of the penis, mainly in the area where the body passes into the glans (near the neck of the penis). On their surface there are white scales. The skin itself in these places is slightly reddish. Individual nodules can merge with each other. They are found not only on the penis, but also in other places. |
Features of balanoposthitis in children
 Balanoposthitis is one of the most common reasons why parents of boys turn to pediatricians and pediatric surgeons. Most often it is a simple infectious or irritative balanoposthitis, which lasts for 5 days and then goes away.
Balanoposthitis is one of the most common reasons why parents of boys turn to pediatricians and pediatric surgeons. Most often it is a simple infectious or irritative balanoposthitis, which lasts for 5 days and then goes away. Sexually transmitted infections are practically never encountered in childhood.
The most common causes of balanoposthitis in childhood:
- secretion of a large amount of smegma and its accumulation between the head of the penis and the foreskin;
- overdeveloped foreskin, which hangs in front of the head of the penis and is difficult to move back - hypertrophic phimosis;
- phimosis is a condition when the foreskin is so narrowed that exposure of the head of the penis becomes impossible;
- non-compliance with personal hygiene rules, rare changes of underwear.
Diagnosis of balanoposthitis
 Diagnostic techniques used for balanoposthitis:
Diagnostic techniques used for balanoposthitis:- General blood analysis– a routine examination that is performed on all patients. An increase in the content of leukocytes and an acceleration of ESR (erythrocyte sedimentation rate) indicate the presence of an inflammatory process in the body.
- General urine analysis- a routine test that is prescribed to all patients. An increase in the number of leukocytes in the urine indicates the presence of an inflammatory process.
- Bacteriological examination of urine and determination of the sensitivity of microorganisms to antibiotics. Makes it possible to identify the causative agent of the disease and prescribe the correct antibiotic therapy.
- PCR– polymerase chain reaction. Laboratory research, which makes it possible to isolate the DNA of a pathogenic microorganism and clarify its type.
- Examination of a scraping from the urethra (urethra) for Treponema pallidum- the causative agent of syphilis. This test should be performed on all adult patients to rule out the presence of syphilis.
Treatment of balanoposthitis
Local procedures for balanoposthitis
| Procedure | Efficacy and indications | Method of application and course duration |
| Baths with potassium permanganate (potassium permanganate). | Potassium permanganate is a powerful antiseptic that kills most pathogenic microorganisms. Sold in pharmacies in powder form, which is intended for dilution in water. | For younger children: Dilute a small amount of potassium permanganate in the bath so that the water is slightly tinted. Carry out a regular bath in this water, during which you open the head of the penis. For older children and adults: Dilute potassium permanganate powder in a glass so that the solution has a pale pink color. Place the penis with the head open in the glass for about 5 to 10 minutes. Repeat the procedure 1 – 3 times a day, as prescribed by the doctor. |
| Baths with furatsilin. | Furacilin is a medicinal substance with antimicrobial and antiseptic effects. It is sold either as a ready-made solution in bottles or in tablet form. | When used in a bottle: Pour the solution from the bottle into a glass. When using tablets: Dissolve 2 tablets in a glass of water (250 ml). Immerse the penis with the bare head in a glass with the solution for 10 minutes. Repeat the procedure 1 – 3 times a day, depending on the doctor’s instructions. |
| Baths with chamomile, sage, plantain, string, St. John's wort, oak bark (one of the plants to choose from). | These medicinal plants have anti-inflammatory and antiseptic effects. They are able to relieve inflammation and destroy pathogens that cause balanoposthitis. | Take 2 - 3 tablespoons of the medicinal plant. Dilute in 1 cup (200 ml) boiling water. Cool. Immerse the penis with the bare head in the infusion for 15 to 20 minutes. Repeat the procedure 4 – 6 times a day for 3 – 5 days. |
| The use of medicinal ointments for balanoposthitis |
||
| An ointment containing two active ingredients:
| Before applying the ointment, you need to perform thorough hygiene of the external genitalia. To treat balanoposthitis, bandages with levomekol are applied to the penis and left overnight. The procedure is repeated for 3 to 5 days. |
| Xeroform ointment consists of two active components:
| Before applying xeroform ointment, perform thorough hygiene of the external genitalia. To treat balanoposthitis, bandages with xeroform ointment are applied to the penis and left overnight. The procedure is repeated for 3 to 5 days. Source: Vidal reference book, 2008. |
Ointments based Flumatasone Pivalate:
| Flumatazone Pivalate is a medicinal substance that has pronounced antiallergic and anti-inflammatory properties. Refers to preparations of hormones of the adrenal cortex. Most effective for balanoposthitis caused by autoimmune reactions, severe pain, itching, inflammation. | Before applying ointments based on Flumatasone Pivalate, perform thorough hygiene of the penis. Take a small amount of ointment and rub into the affected skin. The procedure is repeated 2–3 times a day. Source: Vidal reference book, 2008. |
Other based ointments hormones of the adrenal cortex:
| Adrenal cortex hormone preparations have a strong anti-inflammatory and antiallergic effect. Ointments based on them are especially effective for autoimmune inflammation, when balanoposthitis is accompanied by severe itching and burning, pain, swelling and redness of the glans penis and foreskin. | Ointments should be applied only to cleansed skin before performing thorough personal hygiene. Typically, ointments based on adrenal hormones are applied to the skin of the penis once a day at night (sometimes 2-3 times.) Source: Vidal reference book, 2008. |
| Ointments with antibiotics with infectious balanoposthitis. | There are a large number of ointments whose active ingredients are antibacterial drugs. | The ointment is selected for each patient individually and only by the attending physician. It is necessary to take into account the type of pathogenic microorganisms and their sensitivity to different antibiotics. |
Ointments based on antifungal drugs:
| They have an antifungal effect and are prescribed in cases where it is proven that balanoposthitis is caused by Candida or other fungi. | Usually the ointment is applied to the skin 2 times a day. It is rubbed into the skin. Before doing this, you need to thoroughly wash your genitals. Treatment in most cases lasts for 2–4 weeks; more specific periods are determined by the attending physician. |
Antibacterial therapy for balanoposthitis
 Prescription of antibiotics for balanoposthitis is carried out only in severe cases, when inflammation is accompanied by a severe disturbance in the general condition of the patient, with ulcerative and gangrenous forms, as well as with all types of balanoposthitis that are caused by sexually transmitted infections. Antibacterial drugs for balanoposthitis, as for other diseases, must be used in strict accordance with certain rules:
Prescription of antibiotics for balanoposthitis is carried out only in severe cases, when inflammation is accompanied by a severe disturbance in the general condition of the patient, with ulcerative and gangrenous forms, as well as with all types of balanoposthitis that are caused by sexually transmitted infections. Antibacterial drugs for balanoposthitis, as for other diseases, must be used in strict accordance with certain rules: - An antibiotic should be prescribed only by the attending physician, taking into account the type of microorganism and its sensitivity to antibacterial drugs;
- independent use of these medications, especially in mild forms of balanoposthitis, is strictly contraindicated;
- antibacterial drugs should be used only in the dosages in which they were prescribed;
- Antibiotics are always used strictly on time, otherwise they will not be effective and may have side effects.
Antibiotics prescribed for balanoposthitis:
| Drugs | Mechanism of action | Directions for use and doses |
| Broad-spectrum antibiotics for balanoposthitis caused by nonspecific pathogens |
||
| An antibacterial drug that destroys many types of pathogens. Available in tablets and also in powder for intramuscular administration. The injection form is most preferable, as it is more effective. | Use in adults: 0.5–1.0 g of powder diluted in distilled water or saline intramuscularly, 6–8 times a day, depending on the doctor’s prescription. Use in children: At the rate of 20 - 50 mg per kilogram of body weight, the total dose is divided into 3 - 4 doses during the day. Contraindications: Cefazolin should not be used in pregnant and breastfeeding women, or in people who are allergic to this group of drugs. Source: M. D. Mashkovsky |
| A broad-spectrum antibiotic that can destroy many types of pathogenic microorganisms. Belongs to the group of cephalosporin antibiotics. Ceftriaxone is available in tablets and powder form for intramuscular injection. The most preferred injection form, as it is more effective. | Use in adults and children over 12 years of age: 1 - 2 grams of ceftriaxone powder are dissolved in distilled water or saline and injected once a day. The dosage is selected by the attending physician. Use in children under 12 years of age: The dosage of the powder is selected by the attending physician at the rate of 20–100 mg per kilogram of the child’s weight. Contraindications: Ceftriaxone should not be used in pregnant and breastfeeding women, in persons with bleeding and enterocolitis (inflammation of the small intestine and colon), in persons with an allergy to cephalosporins and in children under 2.5 years of age. Source: M. D. Mashkovsky |
| An antibiotic from the macrolide group that acts on a wide range of pathogens. Prescribed in tablet form. Most pharmacies distribute a branded drug called Sumamed. | Take 1 g (2 - 4 tablets, depending on the dosage) once at the onset of the disease before meals. Contraindications: Azithromycin is contraindicated in diseases that are accompanied by severe disorders of the kidneys and liver. For arrhythmias (heart rhythm disturbances), the drug is prescribed with caution. Source: M. D. Mashkovsky |
| Antibacterial drugs that are used for gonorrheal balanoposthitis |
||
| An antibacterial drug that belongs to the group of beta-lactam antibiotics and is effective against gonococci. Available in the form of tablets of 200 or 400 mg. | Use in adults and children over 12 years of age weighing more than 50 kg: Take 1 (400 mg) or 2 (200 mg) tablets per day at regular intervals. Use in children under 12 years of age weighing less than 50 kg: 8 mg or 4 mg per kilogram of the child’s body weight every 12 hours. The duration of treatment is determined by the doctor individually depending on the severity of the disease. Contraindications: allergic reactions to antibiotics from this group. |
| Ciprofloxacin | An antibacterial drug from the group of fluoroquinolones, which are active against most pathogens of genitourinary system infections, including gonococci. Available in tablet form. | For gonorrhea, adults are advised to take ciprofloxacin in a single dose of 500 mg. In the future, treatment continues in accordance with the doctor’s prescriptions. Contraindications: Ciprofloxacin is contraindicated in children and adolescents under 15 years of age. In elderly people, the dosage should be reduced. You can administer a solution of ciprofloxacin for intravenous use at a dosage of 100 mg of the active substance. Source: M. D. Mashkovsky |
| Ofloxacin | An antibiotic from the fluoroquinolone group, which serves as an alternative to ciprofloxacin. | For gonorrhea, take 400 mg of ofloxacin in tablet form once. In the future, treatment is continued in accordance with the doctor’s prescriptions. Contraindications: Epilepsy, children and adolescents under 15 years of age, pregnant and breastfeeding women. Source: M. D. Mashkovsky |
| Antibacterial drugs that are used for balanoposthitis caused by Trichomonas |
||
| An antibacterial drug that is effective against protozoan microorganisms, including Trichomonas. | Use in adults: 2 grams orally once or for 5 days, 0.5 g 2 times a day. In men, trichomonas are usually not detected during repeated testing after 1 day from the start of treatment. Approximate dosages in children:
Contraindications: Source: M. D. Mashkovsky |
| Antibacterial drugs used for candidiasis |
||
| An antifungal drug that is effective against fungi of the genus Candida. Available in capsules | When treating candidal balanoposthitis and urethritis, 0.2 - 0.4 g of the drug per day is prescribed. Take 1 time. The duration of treatment depends on the severity of the disease and is determined by the doctor. Contraindications: pregnancy, breastfeeding, child under 1 year of age. Source: M. D. Mashkovsky “Medicines. A manual for doctors." 15th edition, revised and expanded, Moscow, “New Wave”, 2005. |
| Antiviral drugs prescribed for balanoposthitis caused by the herpes virus |
||
| An antiviral drug that is active against herpes viruses. | For balanoposthitis, adults need to take acyclovir in a dosage of 0.2 g 5 times a day. There is a break for the night. The duration of treatment is determined by the attending physician. Contraindications: During pregnancy and breastfeeding The drug can be used, but this should be done only for health reasons. Source: M. D. Mashkovsky |
Surgical treatment for balanoposthitis
 In uncomplicated balanoposthitis, surgical treatment is most often not required.
In uncomplicated balanoposthitis, surgical treatment is most often not required. Indications for performing circumcision (circumcision) surgery for balanoposthitis:
- Frequent relapses, chronic course, in which conservative methods do not allow getting rid of balanoposthitis. Before performing surgery, the inflammatory process must subside.
- Complication in the form of cicatricial phimosis. As a result of severe frequent inflammatory processes, scars form on the foreskin, it narrows greatly, and exposure of the head of the penis becomes difficult or impossible.
Prevention of balanoposthitis:
- careful personal hygiene;
- frequent washing, frequent change of underwear;
- exclusion of frequent promiscuity;
- health of the partner: she must also exercise careful intimate hygiene of the genital organs and appear in a timely manner for examinations by the gynecologist;
- It is advisable to bathe young children in water to which a small amount of potassium permanganate has been added;
- if a boy has difficulty opening the head of the penis, then he needs to sit in warm water for a while, after which the head will open easily, better hygiene can be performed;
- Boys need to be brought in for routine examinations with a pediatric surgeon on time.
Why does balanoposthitis develop in boys? How to recognize and how to help?
Balanoposthitis in boys is the main reason for visits to a pediatric urologist. Redness of the foreskin and glans is especially often noticed by parents of children under one year old.Causes of balanoposthitis in children not quite the same as in adults:
- Foreskin hygiene. In boys, the foreskin is physiologically narrowed. In most of them, it is possible to completely retract it and expose the head of the penis only by the age of 3-5, which is considered the norm. But many parents are too zealous with hygiene, and when washing, they greatly pull back and injure the foreskin. Bacteria penetrate into the skin through the resulting microcracks, which can cause inflammation.
- Injuries. Irritation from urine causes itching of the genitals. By scratching this area, the child injures the skin and causes infection. Although other injuries cannot be ruled out at an early age.
- Overheating. Wearing diapers or warm clothes increases moisture in the genital area and promotes the growth of bacteria.
- Candidiasis. After a course of antibiotic treatment, fungi of the genus begin to multiply intensively Candida, causing candidiasis or thrush. In babies, it often appears in the mouth, and sometimes on the genitals.
- Inflammation of the genitourinary system. In children, urinary tract inflammation occurs more often than in adults. This is due to age-related development of the urinary, immune and nervous systems. Often the bladder does not empty completely, and the remaining urine serves as a reservoir for bacterial growth.
- Allergic reaction. Redness of the glans and foreskin may be an allergy, which is associated with:
- diapers;
- use of medications;
- skin care products – powder, baby oil;
- washing powder used to wash children's clothes;
- sweets, berries or other food products.
- Redness and swelling at the end of the penis, sometimes throughout the entire organ.
- The foreskin does not retract well(provided that it moved well before).
- White-yellow discharge on the head, underwear or diaper.
- Baby cries while urinating. Older children refuse to sit on the potty.
- Itching. The child is restless, constantly scratching or retracting the penis. She often cries at the same time because the touch causes pain.
- Frequent, painful urination- indicates that the inflammation has spread to the opening of the urethra.
- Lack of urination, although the child complains that he wants to go to the toilet - this may be due to irritation and swelling of the urethra and bladder.
 A urologist treats balanoposthitis in boys. The specialist will prescribe treatment based on symptoms and test results. But If you do not get an appointment with a doctor, you can alleviate the child’s condition yourself:
A urologist treats balanoposthitis in boys. The specialist will prescribe treatment based on symptoms and test results. But If you do not get an appointment with a doctor, you can alleviate the child’s condition yourself:
- Place your baby in a warm bath. Warm (not hot) water reduces discomfort. Wash the outside of the genitals with neutral baby soap, without additives or fragrances, so as not to aggravate an allergic reaction, if any.
- Pull the skin of the penis upward without exposing the head. Using a syringe without a needle, inject 10 ml of a warm solution of furatsilin or ectericide into the resulting gap. The liquid under pressure washes away the smegma that has accumulated between the head and the foreskin.
- You can immerse the penis in a container with a warm solution of furatsilin, a slightly pink solution of potassium permanganate or chamomile decoction for 5-10 minutes.
- Drop a few drops of oil solution A, E, Vaseline or olive oil into the gap or onto the head. Boiled and cooled sunflower oil will do.
Prevention of balanoposthitis in children is based on compliance with hygiene rules. The genitals are washed daily with warm water and baby soap or neutral shower gel. If there is no redness and nothing bothers the baby, then it is not recommended to move the foreskin during washing.
Why are balanoposthitis and urethritis dangerous?
Balanoposthitis and urethritis often occur together. The fact is that bacteria and fungi from the head spread quite quickly up the urethra. In this case, the mucous membrane of its walls becomes inflamed. This usually occurs 3-7 days after the onset of symptoms of balanoposthitis.Symptoms of balanoposthitis and urethritis
- Changes appearance glans and foreskin - redness, white coating, erosion, spots, fine blistered rash;
- Pain and burning when urinating;
- Purulent or mucous discharge from the urethral opening;
- Swelling of the tissues surrounding the opening of the urethra;
- The initial portion of urine is cloudy, contains mucus, pus, leukocytes, while the remaining portion is transparent;
- The temperature may rise to 38°C.
Balanoposthitis and urethritis are treated with antibiotics and nitrofuran drugs (Furagin, Furamag), which penetrate the mucous membrane of the urinary tract and destroy the causative agent of the disease.
Additionally carry out local treatment:
- baths with potassium permanganate, 2 times a day for 2 weeks;
- clotrimazole 1% cream, 2 times a day for 2 weeks on the affected area.
What can be the complications of balanoposthitis?
Complications of balanoposthitis develop in weakened patients, as well as in men who do not follow doctor’s instructions and ignore hygiene rules.
Why does chronic balanoposthitis develop and how is it treated in men?
Chronic balanoposthitis in men is not a rare phenomenon. Its symptoms are not as pronounced as in the acute form of the disease, but rashes on the head and itching bring a lot of concern. Often men complain that symptoms subside only during treatment. But as soon as they stop using ointments and taking pills, the signs of the disease return.Symptoms of chronic balanoposthitis
- Itching and burning on the scalp, intensifying during an erection or after sexual intercourse.
- Unpleasant sensations occur with increased humidity and physical activity.
- Periodically, the skin of the head and foreskin turns red or becomes covered with spots with clear edges.
- The skin of the head is moist, saturated with interstitial fluid.
- White plaque (sometimes in grains) accumulating in the area of the coronal sulcus.
- Rashes in the form of small pink papules.
- Increased dryness and painful cracks.
1.
Apply Lamisil spray to washed and dried genital skin 2 times a day for 2 weeks.
2.
Laser phoresis with Lamisil spray. Lamisil spray is applied to the skin of the genital organs. After this, the affected area is exposed to a laser through a sterile tube. The duration of the procedure is 5 minutes. Course 7 sessions, every other day.
Read also...
- M. V. Koltunova language and business communication. Language and business communication Etiquette and protocol of business communication
- The Last of the Mohicans Fenimore Cooper The Last of the Mohicans
- Descriptive phrase for the word flower
- Mikhail Zoshchenko - Don't lie: Fairy tale Don't lie Zoshchenko genre